|
 |
- Search
| Asian Spine J > Volume 7(3); 2013 > Article |
Abstract
Purpose
To evaluate the reliability and validity of the adapted Korean version of the Neck Pain and Disability Scale (NPDS).
Overview of Literature
The validity of Korean version of NPDS has not been completely demonstrated yet.
Methods
Translation/retranslation of the English version of NPDS was conducted, and all steps of the cross-cultural adaptation process were performed. The Korean version of the visual analog scale (VAS) measure of pain, NPDS and the previously validated Short Form-36 (SF-36) were mailed to 91 patients, who had been surgically treated for degenerative cervical disease. Eighty-one patients responded to the first mailing of questionnaires and 69 of the first time responder returned their second survey. Factor analysis and reliability assessment by kappa statistics of agreement for each item, the intraclass correlation coefficient and Cronbach's Îą were conducted. Concurrent and construct validity were also evaluated by comparing the responses of NPDS with the results of VAS and responses of SF-36.
Results
Factor analysis extracted 3 factors. All items had a kappa statistics of agreement greater than 0.6. The NPDS showed excellent test/re-test reliability. Internal consistency of Cronbach's Îą was found to be very good. The NPDS was correlated with the VAS. The Korean version of NPDS showed good significant correlation with SF-36 total score and with single SF-36 domains scores.
Neck pain is a major health problem and can have a profound impact on an individual's functional activity. The aim of treatment is to improve patient's function, and thus functional status is an important outcome variable in clinical trials that investigate neck pain. During recent years, there has been a tendency to supplement objective assessments of the spine with subjective measures of functional status using validated questionnaires in patients with neck pain.
Self-completed disability questionnaires have been used as an outcome measure for people with neck pain [1]. These questionnaires can provide a convenient method of collecting and synthesizing a large amount of information on activity limitation [2,3]. In clinical studies, the scales can be used for monitoring the patients with neck pain and assessing their functional status. For these purposes, several disability scales have been developed for the clinical evaluation of patients with neck pain.
The Neck Pain and Disability Scale (NPDS) was developed as a self-reported questionnaire and a comprehensive measure of neck pain [4,5]. The NPDS consists of 20 items concerning neck problems, pain intensity, effect of neck pain on emotions, and effect on life activities. Each single question has a visual analog scale graded from 0 (normal function) to 5 (the worst possible situation your pain problem has taken you). Studies have reported that the test/re-test reliability, validity and responsiveness of NPDS are adequate [4-6], and it has successfully adapted across cultures [2,3,7-12]. Although, Lee et al. [10] developed and established the psychometric properties of Korean versions of 4 neck pain and disability questionnaires, Korean version of NPDS did not have the process of back translation. Moreover, the validity of Korean version of NPDS has not been completely demonstrated and some other measures of similar constructs that had previously been validated should be needed. Thus, the objectives of the present study were to translate a culturally adapted version of the NPDS into the Korean language and to validate the Korean version of the NPDS in Korean patients.
The translation and adaptation processes were carried out by following published guidelines for the cross-cultural adaptation of self-report measures [13]. The translation procedure in this study had 3 stages, namely, forward translation, back translation, and an expert committee discussion. In addition, a pilot study was performed to test whether Korean patients with neck pain could understand the pre-final version correctly. The final version was achieved by discussion of an expert committee and tested for its validity and reliability with the Korean version of the Short Form-36 (SF-36) [14].
The forward translation was completed by 2 native Korean translators. The first translator, also the author of this article, is an orthopedic surgeon, and the other is a professional translator, with no medical background and the person was not initially informed of the purpose of the translation. The 2 translators' versions and the original version were compared and discussed by the 2 translators and an orthopedic professor, until a synthesis of the translation was reached.
The back translation was independently completed by 2 bilingual translators, whose native language was English. Both of these translators lacked a medical background and were not informed or aware of the prior translation procedures.
All the versions of the translation, as well as the original, were discussed by the 4 translators and an expert committee comprised of 3 bilingual experts, 2 orthopedic professors and a Korean translation expert. This committee discussed the translation procedure and results until a consensus was reached on discrepancies. Accordingly, based on the synthetic forward translation, the pre-final version of NPDS was created.
This pre-final version of the NPDS was given to 30 Korean-speaking patients with neck pain. All were receiving one or more therapeutic interventions (non-steroidal anti-inflammatory drug medication and/or physical therapy) at other spine center. Subsequently, these patients were questioned regarding their understanding of the questionnaire items and their responses. These 30 patients included 19 females and 11 males with a mean age of 41.2 years (range, 30-52 years). The interviewer was asked to document any problems that occurred during the administration of the questionnaire. In addition, at the end of the interview each patient was asked to provide comments about the questionnaire and to identify any words that were difficult to understand. The majority of the 30 patients correctly understood the questionnaire. The final form of the Korean version of the NPDS was determined by the expert committee, with the participation of all translators and a consensus was achieved (Suppl. 1).
The Korean version of the visual analog scale (VAS) measure of pain, NPDS and SF-36 were mailed to 91 patients, who had been surgically treated for degenerative cervical disease in one spine center and had a minimum follow-up of 2 years. First mailing contained a consent form, a description of the study, the Korean versions of VAS measure of pain, NPDS and SF-36 and an addressed and stamped return envelope. Eighty-one patients (53 female, 28 male) responded to the first set of questionnaires. Sixty-nine (47 female, 22 male) of the first-time respondents returned their second survey. The average age of the 69 patients was 41.0 years (range, 29-56 years) at the time of survey. The average time between first and second mailings was 2 weeks.
Test-retest reliability was measured by comparing responses to the first and second assessments of NPDS. Reliability was assessed using kappa statistics of agreement for each item and the intraclass correlation coefficient (ICC). Cronbach's Îą was used to evaluate internal consistency. To determine the dimensionality of the items of NPDS, factor analysis was also performed. An item loading on each factor âĽ0.4 was considered as satisfactory. Concurrent and construct validity was evaluated by comparing the responses of NPDS with the results of VAS and responses of SF-36 by using Pearson's correlation coefficient. All statistical analyses were performed with the SPSS ver. 16.0 (SPSS Inc., Chicago, IL, USA).
A total of 81 native Korean-speaking patients with degenerative cervical disease were enrolled in this study. Sixty-nine patients completed the second assessment. Table 1 summarizes the demographic characteristics of the study population.
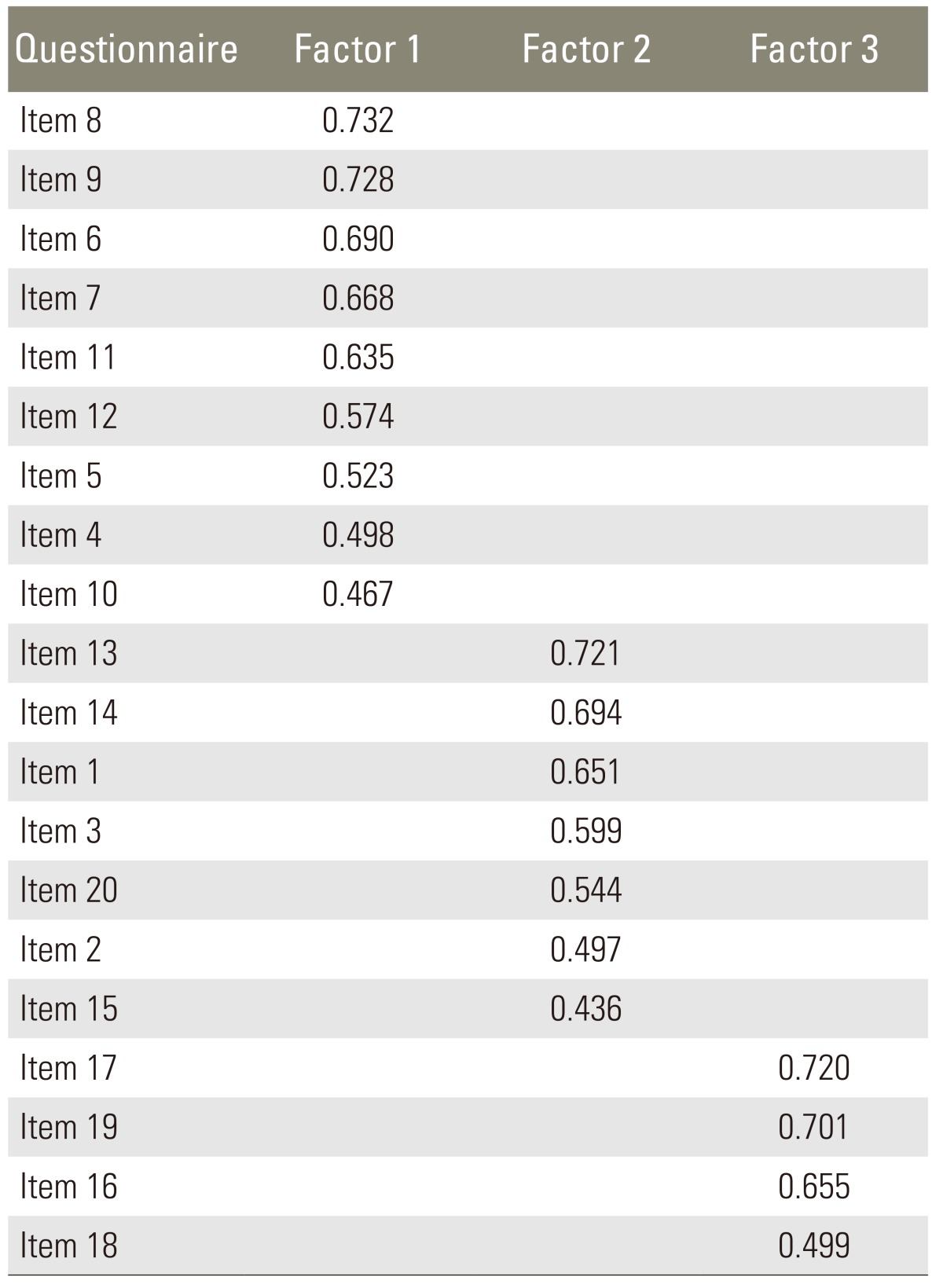
Factor analysis of Korean NDPS revealed a 3-factor structure that in the whole explained 65.3% of variance and extracted 3 factors with eingen values superior to 1 (Table 2). The first factor represents neck dysfunction related to activities (item 8, 9, 6, 7, 11, 12, 5, 4, 10); the second factor represents neck pain and emotion (item 13, 14, 1, 3, 20, 2, 15); and the third factor represents motion of neck (item 17, 19, 16, 18).
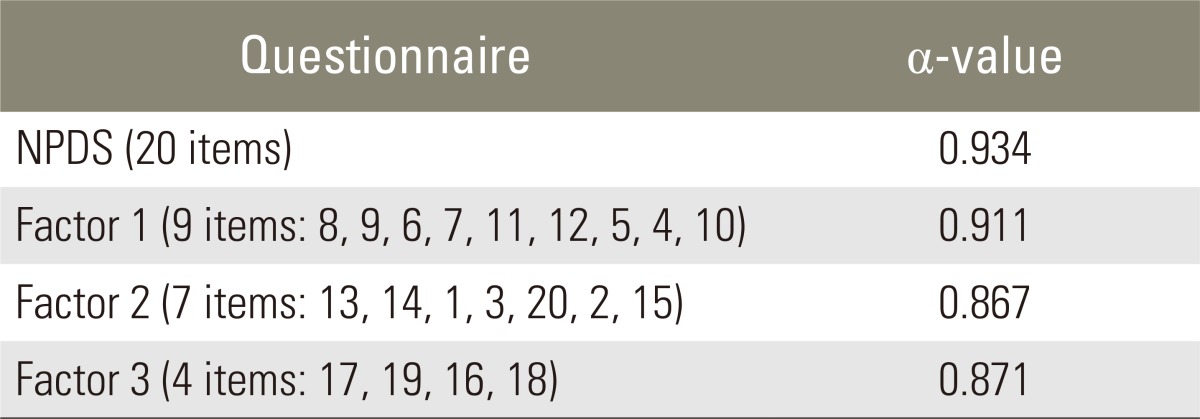
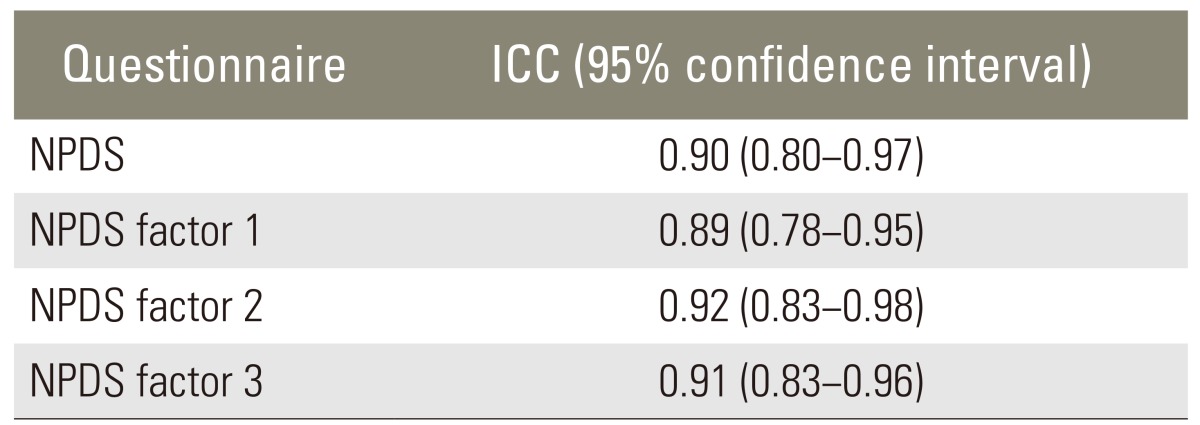
All the items of NPDS had a kappa statistics of agreement greater than 0.6 and ranged from 0.64 to 0.93. The ICC of the test/re-test reliability was 0.90 for the 20 items of NPDS, 0.89 for factor 1, 0.92 for factor 2, and 0.91 for factor 3 (Table 3). In addition, internal consistency was found to be very good with Cronbach's Îą (Table 4).
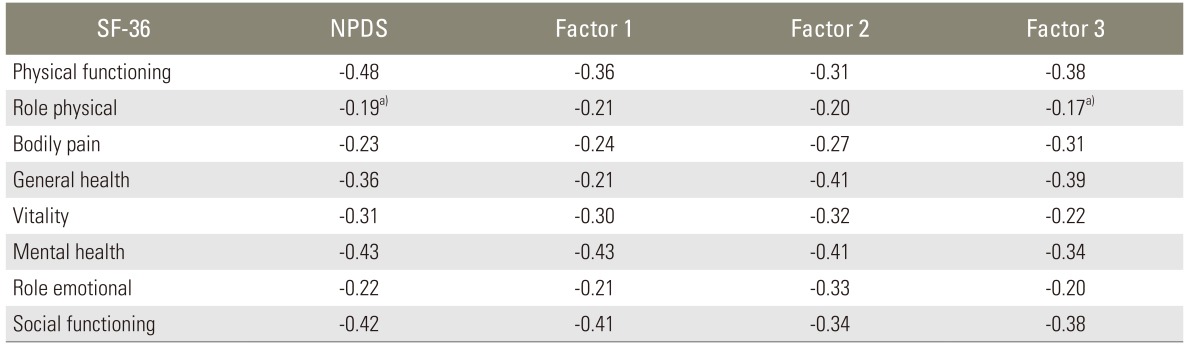
Concurrent validity was evaluated by comparing the responses to the NPDS with the results of VAS by using the Pearson correlation coefficient, and positive correlations were found between NPDS and VAS (r=0.538; p<0.001 for the 20 items of NPDS, r=0.498; p<0.001 for factor 1, r=0.443; p<0.001 for factor 2, and r=0.598; p<0.001 for factor 3). Construct validity based on the comparison with SF-36 questionnaire is shown in Table 5. When we investigated the relationship between NPDS and SF-36 scores, we obtained an r value of -0.41. The Korean version of NPDS showed good significant correlation with functional scales of SF-36.
The objectives of this study were to produce a Korean version of NPDS by translation and adaption. The Korean version of NPDS was found to be clearly understood and easily administered to the patients. The results of this study indicate that the Korean version of the NPDS is a reliable and valid instrument for measuring outcome in Korean patients with neck pain, and its reliability levels were similar to those of the Brazilian-Portuguese [2], Dutch [3], French [12], Hindi [7], Italian [11] and Turkish versions [8,9].
Regarding factor analysis, although Wheeler's original version demonstrated four-factor structure, this study revealed three-factor solutions for the NPDS. A three-factor structure was also identified previously by Monticone et al. [11] (Italian version), Cook et al. [2] (Brazilian-Portuguese version) and by Wlodyka-Demaille et al. [12] (French version). On the contrary, Bicer et al. [8] (Turkish version), Kose et al. [9] (Turkish version), Agarwal et al. [7] (Hindi version) and Lee et al. [10] (Korean version) did not performed a factor analysis in their study.
Regarding internal consistency, Wheeler et al. [5] and Goolkasian et al. [4] reported 0.93 of internal consistency for the English version. The Cronbach's Îą values obtained from this study were 0.934 for the NPDS, 0.911 for factor 1, 0.867 for factor 2 and 0.871 for factor 3 and were also similar to those reported by other studies [2,11]. This result shows that this translated version is reliable and has a low standard error of measurement.
The reproducibility of each of the 20 items was satisfactory with kappa statistics of agreement superior to 0.6 in our study. Although several validation studies of the NPDS have been published, an average reproducibility of NPDS item has not been addressed. If the first and second questionnaires were completed by patients themselves while visiting the clinic, it enables an average reproducibility of item to see lower for other items. The results were explained by some patients who had answered "yes" to an item during their first visit and answered "no" during their second visit, and these patients probably had to wait for a longer time than others for the consultation before being received by the interviewer, which perhaps was not the case during the second visit [15]. To avoid this bias, we mailed the Korean version of the VAS for pain, NPDS and SF-36 to 91 patients, who had been surgically treated for degenerative cervical disease. The agreement of all the items was very good in this study. In fact, an ICC of 0.90 is a very good measure of reliability of the Korean version of the NPDS and is in accordance with other translated versions with ICCs ranging from 0.81 to 0.97 [5,7,9-12].
Reliability of functional status questionnaires may be measured using an interval of 1 to 2 weeks between assessments, because during this time, clinical status is unlikely to change appreciably in patients with chronic pain in the absence of specific intervention [16], and thus we used this aspect in the present study.
Our analysis of concurrent validity showed a positive correlation between the Korean version of NPDS and VAS. In the analysis for construct validity, the NPDS was expected to reveal correlations with health related quality of life scales. Therefore, we analyzed construct validity by comparing the total scores of the Korean version of NPDS to a total score of SF-36; a high correlation was found (p<0.001), which suggests confirming the multidimensional qualities of the scale. We also compared the total scores of NPDS and 3 subscales to each domain of SF-36. High correlations (p<0.001) were found when total score of NPDS was compared with each of the 8 domains of SF-36, with the exception of physical role domain which, though significant, was of the lowest correlation (p=0.037). In addition, high correlations were also found between 3 subscales and each of the 8 domain, with the exception between factor 3 and physical role domain (p=0.043). According to subscales meanings, the correlations between factor 1 of NPDS and physical functioning domain of the SF-36, between factor 2 and mental health and/or role emotional domains, and between factor 3 and physical functioning domain were expected to be stronger than other functional domains of the SF-36; all these correlations were quite confirmed (p<0.001). These results are similar to previous study that used the SF-36 to evaluate construct validity [2,11].
Before interpreting our results, several limitations must be considered. First, the number of samples tested was relatively small. Second, the current cohort study might not be fully adequate to be considered representative, because this is not a multicenter based study. Finally, this validation was performed only in patients, who underwent surgery for degenerative cervical disease. The weakness of this study is that the patient sample did not involve patients with degenerative cervical disease, who did not undergo surgery as well as the patients with degenerative cervical disease prior to surgery.
To the authors' knowledge, this Korean version of the NPDS is the condition-specific outcome instrument for the validation of neck pain in Korean population. The development and validation of multiple-language versions of existing validated questionnaires plays a key role in standardizing outcome measurements and increasing the statistical powers of clinical studies. The results of this study demonstrated that the NPDS was successfully translated into Korean version without losing the psychometric properties of the original version. Accordingly, the Korean version of the NPDS appears to be a reliable and valid outcome measure of functional status in patients with neck pain. Thus, we recommend that this Korean version of the NPDS can be utilized for future clinical studies in Korea.
Supplementary materials
Suppl. 1
Korean Version of the Neck Pain and Disability.
Supplementary material can be found via http://www.asianspinejournal.org/src/sm/asj-7-178-s001.pdf
References
1. Pietrobon R, Coeytaux RR, Carey TS, Richardson WJ, DeVellis RF. Standard scales for measurement of functional outcome for cervical pain or dysfunction: a systematic review. Spine (Phila Pa 1976) 2002 27:515â522. PMID: 11880837.


2. Cook C, Richardson JK, Braga L, et al. Cross-cultural adaptation and validation of the Brazilian Portuguese version of the Neck Disability Index and Neck Pain and Disability Scale. Spine (Phila Pa 1976) 2006 31:1621â1627. PMID: 16778699.


3. Jorritsma W, de Vries GE, Geertzen JH, Dijkstra PU, Reneman MF. Neck Pain and Disability Scale and the Neck Disability Index: reproducibility of the Dutch Language Versions. Eur Spine J 2010 19:1695â1701. PMID: 20424872.



4. Goolkasian P, Wheeler AH, Gretz SS. The neck pain and disability scale: test-retest reliability and construct validity. Clin J Pain 2002 18:245â250. PMID: 12131066.


5. Wheeler AH, Goolkasian P, Baird AC, Darden BV 2nd. Development of the Neck Pain and Disability Scale. Item analysis, face, and criterion-related validity. Spine (Phila Pa 1976) 1999 24:1290â1294. PMID: 10404569.


6. Blozik E, Himmel W, Kochen MM, Herrmann-Lingen C, Scherer M. Sensitivity to change of the Neck Pain and Disability Scale. Eur Spine J 2011 20:882â889. PMID: 20694734.


7. Agarwal S, Allison GT, Agarwal A, Singer KP. Reliability and validity of the Hindi version of the Neck Pain and Disability Scale in cervical radiculopathy patients. Disabil Rehabil 2006 28:1405â1411. PMID: 17071572.


8. Bicer A, Yazici A, Camdeviren H, Erdogan C. Assessment of pain and disability in patients with chronic neck pain: reliability and construct validity of the Turkish version of the neck pain and disability scale. Disabil Rehabil 2004 26:959â962. PMID: 15371043.


9. Kose G, Hepguler S, Atamaz F, Oder G. A comparison of four disability scales for Turkish patients with neck pain. J Rehabil Med 2007 39:358â362. PMID: 17549325.


10. Lee H, Nicholson LL, Adams RD, Maher CG, Halaki M, Bae SS. Development and psychometric testing of Korean language versions of 4 neck pain and disability questionnaires. Spine (Phila Pa 1976) 2006 31:1841â1845. PMID: 16845361.


11. Monticone M, Baiardi P, Nido N, Righini C, Tomba A, Giovanazzi E. Development of the Italian version of the Neck Pain and Disability Scale, NPDS-I: cross-cultural adaptation, reliability, and validity. Spine (Phila Pa 1976) 2008 33:E429âE434. PMID: 18520930.


12. Wlodyka-Demaille S, Poiraudeau S, Catanzariti JF, Rannou F, Fermanian J, Revel M. French translation and validation of 3 functional disability scales for neck pain. Arch Phys Med Rehabil 2002 83:376â382. PMID: 11887120.


13. New medical therapy for the common cold, influenza and bronchitis. Translation by F.F. Kao of an excerpt of a Chinese book. Am J Chin Med (Gard City N Y) 1975 3:187â205. PMID: 1124735.

14. Han CW, Lee EJ, Iwaya T, Kataoka H, Kohzuki M. Development of the Korean version of Short-Form 36-Item Health Survey: health related QOL of healthy elderly people and elderly patients in Korea. Tohoku J Exp Med 2004 203:189â194. PMID: 15240928.


15. Maaroufi H, Benbouazza K, Faik A, et al. Translation, adaptation, and validation of the Moroccan version of the Roland Morris Disability Questionnaire. Spine (Phila Pa 1976) 2007 32:1461â1465. PMID: 17545917.


16. Johansson E, Lindberg P. Subacute and chronic low back pain: reliability and validity of a Swedish version of the Roland and Morris Disability Questionnaire. Scand J Rehabil Med 1998 30:139â143. PMID: 9782540.


- TOOLS