|
 |
- Search
| Asian Spine J > Volume 8(6); 2014 > Article |
Abstract
Overview of Literature
Cryotherapy has generally been performed subsequent to surgery on joints and in this application its clinical effects are well understood. However, cryotherapy has yet to be used following spine surgery. Its clinical efficacy in this context is unknown.
Methods
Thirty six patients had undergone one level microendoscopic surgery. Sixteen were enrolled into the cooling group, with the remaining 20 making up the no postoperative cryotherapy control group. Cryotherapy was performed at 5â using an icing system. A silicone balloon catheter with a thermo sensor on the tip was placed in the surgical wound. The temperature in the wound was recorded every 30 minutes until the next morning. The relationship between the depth of the sensor and the temperature in the wound were investigated using simple linear regression analysis. Laboratory data, visual analogue scale (VAS) for wound pain and postoperative bleeding were investigated.
Results
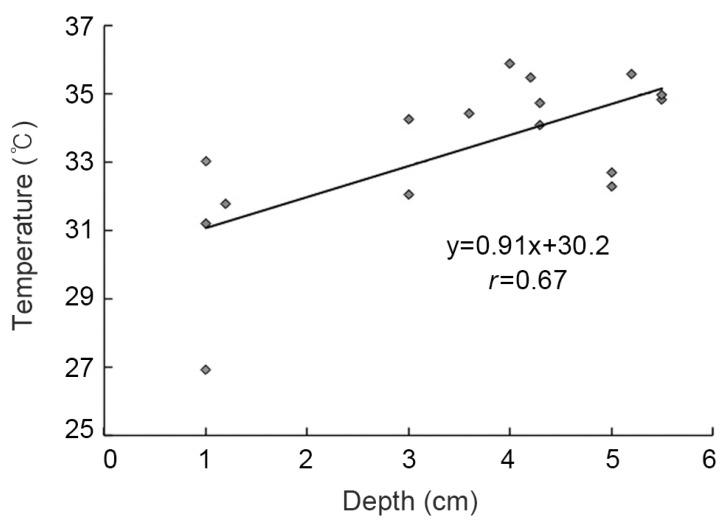
The mean temperature in the surgical wound was 37.0 in the control group and 35.0â in the cooling group (p<0.001). There was a positive correlation between the depth of the thermo sensor and the temperature in the wound in the cooling group (y=0.91x+30.2, r=0.67, p=0.004). There were no significant differences between the groups in terms of laboratory data, VAS or postoperative bleeding.
Cryotherapy has generally been performed subsequent to joint surgery. Tissue metabolism is suppressed because the temperature of tissues decreases, which lessens pain, edema and postoperative bleeding, and promotes rapid recovery of range of motion after surgery [1,2,3,4,5]. Cooling is generally performed with an ice bag or a cooling pad [6,7], which does decrease the temperature in the joint [5,6,8]. Cryotherapy has not yet generally been used following spinal surgery. Only a few reports have been concerned with cryotherapy with a cooling pad post spinal surgery, in which cryotherapy reduced postoperative pain and decreased the length of hospitalixation [9,10,11]. However, its clinical efficacy in this context has not yet been established. Also, whether or not cooling of the body surface decreases the temperature of the deep tissues of the body trunk is unclear.
The current study examined subjects following spinal surgery cryotherapy to assess whether the temperature of the deep tissues in the surgical wound decreases, whether clinical benefits including reduction of inflammation, pain and postoperative bleeding are obtained and complications or unpleasant conditions, such as limitation in postural movement.
From January 2008 to April 2009, 37 consecutive patients (24 males and 13 females) who had undergone one level microendoscopic decompression for lumbar spinal stenosis or one level microendoscopic discectomy for lumbar disc herniation were included in this study. All procedures were performed at our institution by a single surgeon who was experienced in microendoscopic spinal surgery. Exclusion criteria included patient refusal of cryotherapy, two or more levels of microendoscopic decompression or discectomy and multiple operations on the back. One patient was excluded due to conversion to open surgery. No patient refused cryotherapy and none had undergone multiple operations on the back. All subjects who received cryotherapy consented to participate.
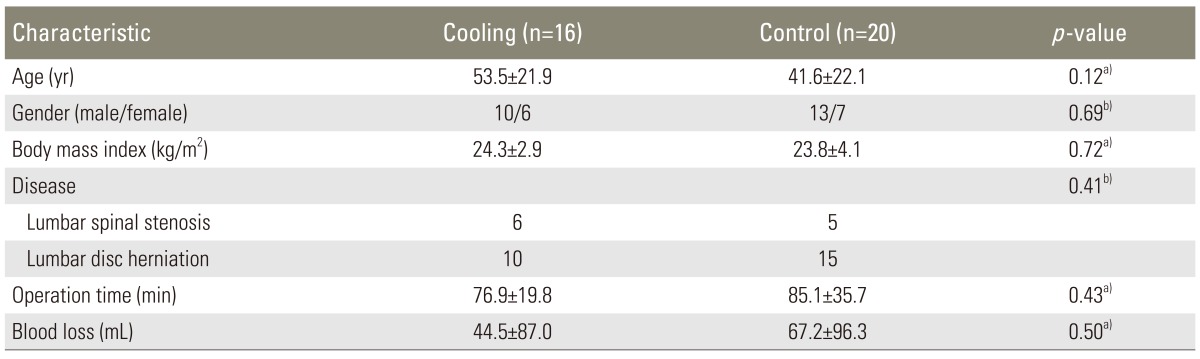
Postoperative cryotherapy was performed in 16 consecutive patients (10 males and 6 females) between September 2008 and April 2009 (cooling group), and postoperative cryotherapy was not performed for 20 consecutive patients (13 males and 7 females) between January 2008 and August 2008 (control group) (Table 1).
Cryotherapy was performed by using an Icing System CF3000 (Japan Sigmax, Tokyo, Japan). After surgery, a cooling pad (288 mmĂ330 mm) was applied to the wound site over a light dressing and clothes, and secured with a bust band (Fig. 1). The wound site was cooled for 15 to 20 hours until the next morning. The temperature of the cooling device was set at 5â.
A 4.0 mm-diameter silicone balloon catheter with a thermo sensor on the tip (Terumo, Tokyo, Japan) was placed in the surgical wound and used for suction drainage. The temperature in the wound was automatically recorded repeatedly every 30 minutes until the next morning by using a Coretemp CM-210 (Terumo). In the cooling group, the depth of the thermo sensor was measured on the lateral view of a postoperative plain roentgenogram. Relationships between the depth of the thermo sensor and the temperature in the wound were investigated using simple linear regression analysis.
Laboratory data of creatine phosphokinase (CPK) (preoperation, postoperative day 1) and C-reactive protein (CRP) (postoperative day 3), visual analogue scale (VAS) assessing wound pain (postoperative day 1 and 7) and the amount of postoperative bleeding until the next morning were recorded. We performed statistical analyses between the two groups using the Mann-Whitney U-test and the Fisher exact probability test were used, with p<0.05 indicating statistical significance.
Complications and unpleasantness during cryotherapy were also investigated. Our institutional review board approved this study.
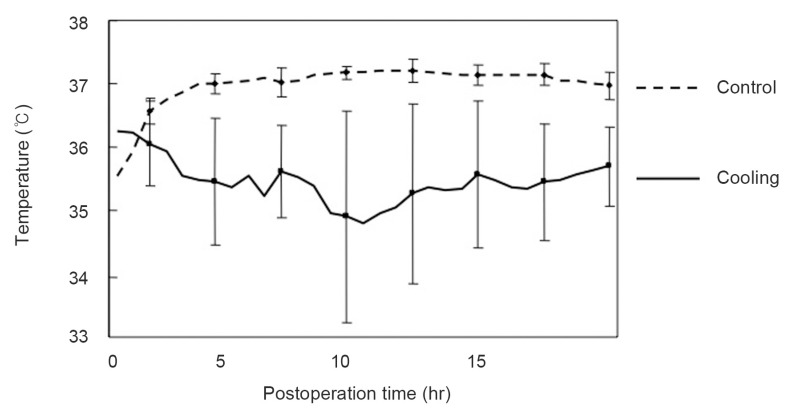
In the control group, the temperature in the surgical wound gradually increased after surgery, reaching a thermostatic phase several hours after surgery. In the cooling group, the temperature in the surgical wound gradually decreased after surgery, reaching a thermostatic phase a few hours after surgery (Fig. 2). The mean temperature in the surgical wound was 37.0âÂą0.36â in the control group and 35.0âÂą0.56â in the cooling group; the difference was statistically significant (p<0.001). Regarding the relationship between the thermo sensor depth and the wound temperature, in the cooling group the temperature of the shallow tissues in the surgical wound was lower but the temperature of the deep tissues was higher. There was a positive correlation between the depth of the thermo sensor and the wound temperature in the cooling group (y=0.91x+30.2, r=0.67, p=0.004) (Fig. 3).
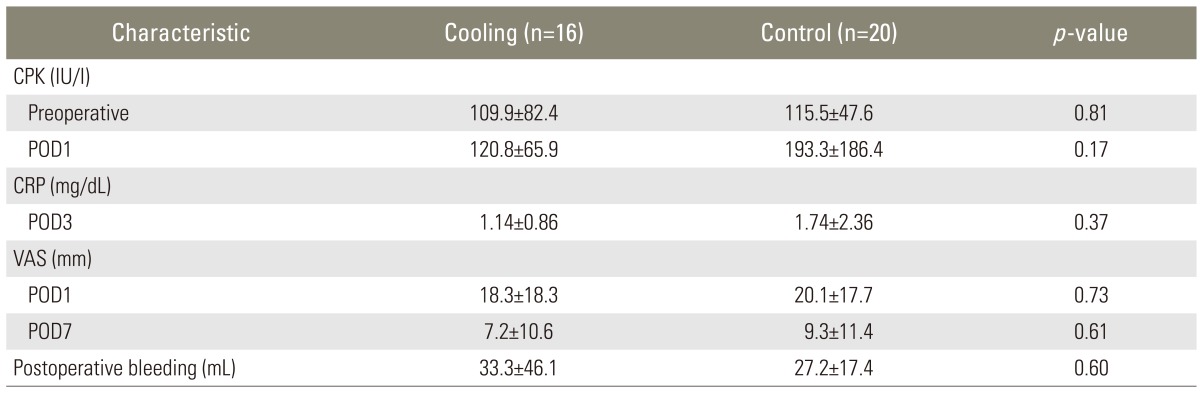
CPK, CRP, VAS, and the amount of postoperative bleeding were not significantly different between the groups (Table 2). No patients complained of unpleasantness by cooling and cryotherapy did not disturb postural movement. There were no complications, such as infection or sensory disturbance.
This is the first report of the measurement of temperature of the deep tissue of the body trunk directly during cryotherapy. Cryotherapy has generally been performed with an ice bag. However, it has been difficult to cool the body trunk, especially the spine in the supine or lateral position, which is why ice bag cryotherapy has not been employed after spinal surgery.
The icing system CF3000 is a device that can establish a liquid temperature from 0â to 13â by the Peltier effect, circulating the liquid to the pad and cooling the wound once the pad is attached. In this study, use of the icing system CF3000 enabled cryotherapy in the supine or lateral position following spinal surgery. None of the patients complained of unpleasantness or sensory disturbance, and there were no complications including infection or delayed healing of the surgical wound.
There have been only a few reports concerning cryotherapy with a cooling pad post spinal surgery. Reduced postoperative pain and decreased length of hospital stay have been reported [10,11], as has reduced postoperative bleeding [11]. However, no studies have yet been performed to establish whether cooling of the skin decreases the temperature of the deep tissues and reduces inflammatory mediator release.
Presently, the temperature in the wound in the cooling group was decreased to a statistically significant degree compared with the control group. However, the difference was small (2.0â) and there were no clinical benefits, such as reduction of inflammation, pain, or postoperative bleeding. In addition, the regression line between the depth of the thermo sensor and the temperature in the wound demonstrated that the cooling effect to the deep tissues of the body trunk was very small.
Warren et al. [6] reported that when cryotherapy was performed on 12 knees for 60 minutes, the intraarticular temperature decreased by 9.7â on average. Moreover, Ohkoshi et al. [5] reported that when cryotherapy was performed on 7 knees at 5â for 48 hours after anterior cruciate ligament reconstruction, the intraarticular temperature showed a mean decrease of 6.4â during the low-temperature phase that lasted for several hours after the surgery. In the joint, the decrease in the intraarticular temperature is presumed to be strong, because it is possible to cool all surrounding areas. On the other hand, in the body trunk, the cooling effect on the deep tissues of the body trunk is presumed to be weaker because it is impossible to cool all the surrounding parts. This study demonstrated that cryotherapy after spinal surgery was less effective than when used subsequent to joint surgery.
There are some potential limitations of this study. First, this study was not a randomized trial. However, since all procedures were performed by a single surgeon with experience in microendoscopic surgery, and because in our institutions spinal microendoscopic surgery has been performed on more than 100 patients, it is likely that there was no difference in surgical technique and postoperative therapy among the subjects. Second, the subjects were treated using less invasive microendoscopic procedures. The effects of cryotherapy in patients who undergo more invasive spinal surgery, such as spinal fusion, need to be determined. Finally, we were not able to find significant differences between the groups in the laboratory data or the amount of postoperative bleeding, possibly due to the small sample size. Power analysis using G*Power 3.1 software (freely available on the Internet) showed that approximately 58 patients in the cooling group and 72 patients in the control group would be necessary to obtain sufficient power, around 0.8, an effect size of 0.5, and an a error probability of 0.05. Consequently, the results of previous studies [10,11], which showed clinical benefits, are not invalidated by the results of the present study.
We performed cryotherapy after one level microendoscopic lumbar spine surgery using the Icing System CF3000. This is the first report measuring temperature of the deep tissue of the body trunk directly during cryotherapy. Although no significant differences between the groups in the laboratory data and the amount of postoperative bleeding were observed, wound temperature decreased significantly after spinal surgery cryotherapy.
References
1. Cohn BT, Draeger RI, Jackson DW. The effects of cold therapy in the postoperative management of pain in patients undergoing anterior cruciate ligament reconstruction. Am J Sports Med 1989 17:344â349. PMID: 2729484.


2. Kullenberg B, Ylipaa S, Soderlund K, Resch S. Postoperative cryotherapy after total knee arthroplasty: a prospective study of 86 patients. J Arthroplasty 2006 21:1175â1179. PMID: 17162178.


3. Lessard LA, Scudds RA, Amendola A, Vaz MD. The efficacy of cryotherapy following arthroscopic knee surgery. J Orthop Sports Phys Ther 1997 26:14â22. PMID: 9201637.


4. Levy AS, Marmar E. The role of cold compression dressings in the postoperative treatment of total knee arthroplasty. Clin Orthop Relat Res 1993 (297): 174â178. PMID: 7902225.

5. Ohkoshi Y, Ohkoshi M, Nagasaki S, Ono A, Hashimoto T, Yamane S. The effect of cryotherapy on intraarticular temperature and postoperative care after anterior cruciate ligament reconstruction. Am J Sports Med 1999 27:357â362. PMID: 10352774.


6. Warren TA, McCarty EC, Richardson AL, Michener T, Spindler KP. Intra-articular knee temperature changes: ice versus cryotherapy device. Am J Sports Med 2004 32:441â445. PMID: 14977671.


7. Whitelaw GP, DeMuth KA, Demos HA, Schepsis A, Jacques E. The use of the Cryo/Cuff versus ice and elastic wrap in the postoperative care of knee arthroscopy patients. Am J Knee Surg 1995 8:28â30. PMID: 7866800.

8. Martin SS, Spindler KP, Tarter JW, Detwiler K, Petersen HA. Cryotherapy: an effective modality for decreasing intraarticular temperature after knee arthroscopy. Am J Sports Med 2001 29:288â291. PMID: 11394596.


9. Brandner B, Munro B, Bromby LM, Hetreed M. Evaluation of the contribution to postoperative analgesia by local cooling of the wound. Anaesthesia 1996 51:1021â1025. PMID: 8943591.


10. Fountas KN, Kapsalaki EZ, Johnston KW, Smisson HF 3rd, Vogel RL, Robinson JS Jr. Postoperative lumbar microdiscectomy pain. Minimalization by irrigation and cooling. Spine (Phila Pa 1976) 1999 24:1958â1960. PMID: 10515023.


11. Steffee AD, Booher JW, Biscup RS. Evaluation of cold therapy in postoperative spine patients. Surg Technol Int 1996 5:385â387. PMID: 15858767.

Fig. 1
Use of the cooling pad. The cooling pad (288 mmĂ330 mm) (A) was fixed from the patients' clothes to the body trunk using a bust band (B), and sticks in both supine (C) and lateral position (D).
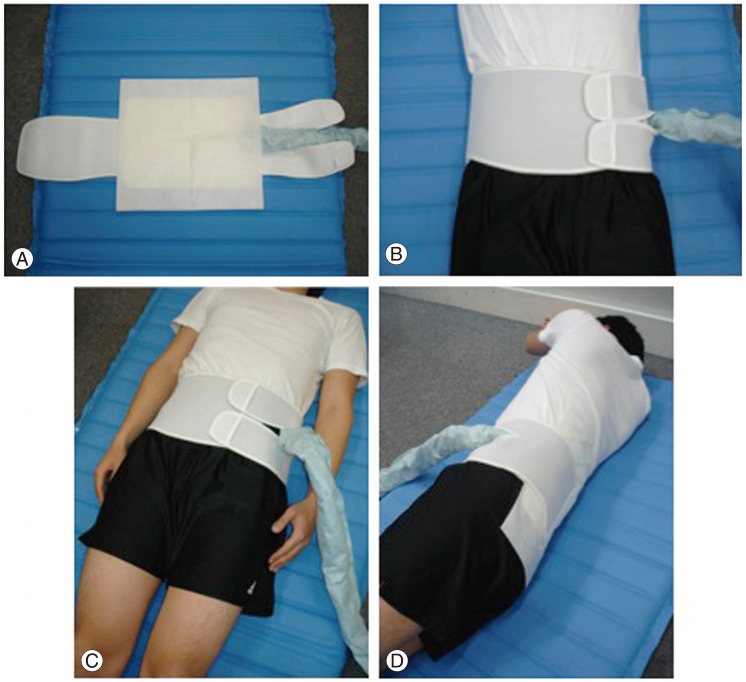
Fig. 3
The temperature of the shallow tissues in the surgical wound was lower, but the temperature of the deep tissues was higher.
- TOOLS
-
METRICS

- Related articles in ASJ
-
Functional Outcome after Spinal Meningioma Surgery2022 October;16(5)
Esophageal Perforation after Anterior Cervical Spine Surgery2019 December;13(6)
Response to: Hypoglossal Nerve Unjury after Cervical Spine Surgery2015 August;9(4)
Hypoglossal Nerve Injury after Cervical Spine Surgery2015 August;9(4)