 |
 |
- Search
| Asian Spine J > Volume 13(4); 2019 > Article |
|
Abstract
Purpose
We hypothesized that larger the C1ŌĆōC2 fusion angle, greater the severity of the sagittal malalignment of C0ŌĆōC1 and C2ŌĆōC7.
Overview of Literature
In our experience, instances of sagittal malalignment occur at C0ŌĆōC1 and C2ŌĆōC7 following atlantoaxial fusion in patients with Os odontoideum (OO).
Methods
We assessed 21 patients who achieved solid atlantoaxial fusion for reducible atlantoaxial instability secondary to OO. The mean patient age at the time of the operation was 42.8 years, and the mean follow-up duration was 4.9 years. Radiographic parameters were preoperatively measured and at the final follow-up. The patients were divided into two groups (A and B) depending on the C1ŌĆōC2 fusion angle. In group A (n=11), the C1ŌĆōC2 fusion angle was Ōēź22┬░, whereas in group B, it was <22┬░. The differences in the radiographic parameters of the two groups were evaluated.
Results
At the final follow-up, the C1ŌĆōC2 angle was increased. However, this increase was not statistically significant (18┬░ vs. 22┬░, p=0.924). The C0ŌĆōC1 angle (10┬░ vs. 5┬░, p<0.05) and C2ŌĆōC7 angle (22┬░ vs. 13┬░, p<0.05) significantly decreased. The final C1ŌĆōC2 angle was negatively correlated with the final C0ŌĆōC1 and C2ŌĆōC7 angles. The final C0ŌĆōC1 angle (4┬░ vs. 6┬░, p<0.05) and C2ŌĆōC7 angle (8┬░ vs. 20┬░, p<0.05) were smaller in group A than in group B. After atlantoaxial fusion, the C0ŌĆōC1 range of motion (ROM; 17┬░ vs. 9┬░, p<0.05) and the C2ŌĆōC7 ROM (39┬░ vs. 31┬░, p<0.05) were significantly decreased.
Conclusions
We found a negative association between the sagittal alignment of C0ŌĆōC1 and C2ŌĆōC7 after atlantoaxial fusion and the C1ŌĆōC2 fusion angle along with decreased ROM. Therefore, overcorrection of C1ŌĆōC2 kyphosis should be avoided to maintain good physiologic cervical sagittal alignment.
The surgical treatment of patients with C1ŌĆōC2 instability with Os odontoideum (OO) is proven successful when using a combination of fusion and internal fixation technique [1-4]. Indications for surgical treatment can be simply considered in conjunction with the existence of OO and OO associated with occipitocervical pain and/or with neurologic signs and symptoms. Other factors that may help determine the need for stabilization and/or decompression include C1ŌĆōC2 instability, associated deformities, and spinal cord compression.
Several techniques have been used to stabilize the C1 and C2 vertebrae in patients with OO [1-11]. The early surgical techniques of C1ŌĆōC2 fusion include posterior sublaminar wiring techniques, such as the Gallie technique and BrooksŌĆōJenkins technique [5-7]. The transarticular screw fixation technique, introduced by Magerl and Seemann [8], is most typically relied upon because it provides immediate rigid fixation postoperatively and has higher fusion rates than posterior sublaminar wiring techniques [9]. Recently, another C1ŌĆōC2 posterior fixation technique that uses a C1 lateral mass screw with C2 pedicle screw fixation, introduced by Goel and Laheri [10] and modified by Harms and Melcher [11], has become widely accepted as a standard treatment.
Although the clinical results for atlantoaxial instability (AAI) are satisfactory, some patients show postoperative reduction in occipitocervical and subaxial cervical lordosis. Several studies have reported that the appearance of occipitocervical and subaxial sagittal malalignments may be attributable to hyperlordotic C1ŌĆōC2 fusion [12-14]. However, the condition of most patients in these studies was complicated with the presence of rheumatoid arthritis (RA). Occipitocervical and subaxial sagittal malalignments may develop as part of the natural course in this kind of disease. Therefore, the treatment results in non-rheumatoid arthritic patients who underwent posterior C1ŌĆōC2 fusion require further investigation.
Therefore, we performed retrospective evaluation of the influence of atlantoaxial fusion on the sagittal alignment of the occipitocervical and subaxial spines in OO patients with AAI.
We retrospectively analyzed 21 patients (10 women and 11 men) who achieved solid fusion for OO with reducible AAI and were followed up of for at least 24 months. The criteria for C1ŌĆōC2 fusion were as follows: (1) difference of <2┬░ between the flexion and extension lateral radiographs, (2) formation of a bony bridge, (3) no findings of implant failure, and (4) radiolucency in <50% of the tissue around the implant [15]. The mean age at the time of operation was 42.8 years (range, 5ŌĆō73 years), whereas the mean follow-up duration was 4.9 years (range, 2ŌĆō12 years). Eight patients complained of intractable occipitocervical pain, and 13 complained of myelopathy. All the patients with myelopathy showed intramedullary signal change and retrodental reactive lesions (two cystic and 11 fibrocartilaginous lesions) on magnetic resonance imaging. Magnetic resonance images were produced using a 1.5-tesla unit (Siemens, Munich, Germany) in 13 myelopathy patients. Subjects who (1) had RA, (2) underwent combined surgery on the subaxial cervical spine, (3) had non-union, (4) underwent revision surgery, and (5) had combined cervical deformity of ŌēżC2 level were excluded.
All the surgeries were performed by a single senior surgeon. The direction of AAI was defined as the direction of displacement of the spinolaminar line during flexion and extension (Fig. 1). Eleven patients with anterior AAI underwent posterior sublaminar wiring alone, and 10 patients with combined (anterior+posterior) AAI underwent posterior sublaminar wiring and transarticular screw fixation. Autogenous iliac bone graft was used for all patients. The operative techniques used were as described. The patients were placed in the prone position with the skull fixed with a Mayfield clamp. The neck was positioned to optimize access by flexing it slightly at the occiput while extending the subaxial spine. We attempted to reduce the C1ŌĆōC2 articulation during this positioning process. The procedures were assisted with fluoroscopy. A midline incision was made over C1ŌĆōC2 but distally extended to allow the required drill angulation, and the posterior aspects of C1 and C2 were fully exposed. Subperiosteal exposure of the C1 arch and C2 posterior elements was performed. Cannulated screws were placed for bilateral transarticular fixation under lateral fluoroscopic guidance. Following screw placement, the modified sublaminar wiring method was used to fix an iliac bone graft. A Philadelphia collar or Halovest was applied for 12 weeks after the procedure.
Plain anteroposterior and lateral radiographs of the cervical spine were recorded preoperatively, postoperatively, and at the final follow-up with subjects in the upright neutral, flexion, and extension positions. Radiographic parameters were measured preoperatively and at the final follow-up. The C0ŌĆōC1, C1ŌĆōC2, and C2ŌĆōC7 angles were measured on neutral lateral radiographs. The C0ŌĆōC1, C1ŌĆōC2, and C2ŌĆōC7 range of motions (ROMs) were measured on flexion and extension lateral radiographs (Fig. 2). The differences in the radiographic parameters from before the surgery to that at the final follow-up were evaluated using paired T-test. The patients were divided into two groups as per the C1ŌĆōC2 fusion angle. In group A (n=11), the C1ŌĆōC2 fusion angle was Ōēź22┬░, whereas that in group B was <22┬░ (Table 1). The differences in the radiographic parameters of the two groups were evaluated using independent T-test. Correlation between the C1ŌĆōC1, C0ŌĆōC1, and C2ŌĆōC7 angles was analyzed using Pearson test. A p-value of <0.05 was considered statistically significant. This retrospective study was approved by the Institutional Review Board of the Uijeongbu St. Mary's Hospital (e-IRB UC17R ESI0145) and informed consent was waived.
The C1ŌĆōC2 angle was increased from 18.4┬░┬▒5.8┬░ preoperatively to 21.6┬░┬▒9.1┬░ at the final follow-up. However, this improvement was not statistically significant (p=0.924). The C0ŌĆōC1 angle was reduced from 9.73┬░┬▒7.2┬░ preoperatively to 4.9┬░┬▒2.3┬░ at the final follow-up (p<0.05). The C2ŌĆōC7 angle was also significantly decreased from 21.8┬░┬▒13.2┬░ to 13.3┬░┬▒10.6┬░ (p<0.05). The final C1ŌĆōC2 angle was negatively correlated with the final C0ŌĆōC1 angle (correlation coefficient, -0.547; p<0.05) and final C2ŌĆōC7 angle (correlation coefficient, -0.705; p<0.01). Following atlantoaxial fusion, the C1ŌĆōC2 ROM (16.6┬░┬▒9.8┬░ versus 0┬░, p<0.001), C0ŌĆōC1 ROM (16.6┬░┬▒4.4┬░ versus 8.7┬░┬▒3.8┬░, p<0.05), and C2ŌĆōC7 ROM (38.9┬░┬▒20.6┬░ versus 31┬░┬▒15.2┬░, p<0.05) were significantly decreased. The final C0ŌĆōC1 angle (3.8┬░┬▒1.2┬░ versus 6.2┬░┬▒3.4┬░, p<0.05) and the C2ŌĆōC7 angle (7.7┬░┬▒9.9┬░ versus 20.0┬░┬▒7.2┬░, p<0.05) were smaller in group A than in group B (p<0.05 for both) (Figs. 3, 4, Table 1).
Atlantoaxial articulation is an anatomic feature with a full ROM in the spine that is dependent for its stability on ligamentous support and the integrity of the odontoid. AAI etiology includes trauma, congenital malformations, OO, RA, malignancy, and skeletal dysplasia. OO is an anomaly defined as an ossicle with smooth circumscribed margins and no osseous continuity with the C2 body [1,2,4,16]. OO patients with instability can be asymptomatic or can present several symptoms, including occipitocervical pain alone, myelopathy, or intracranial symptoms from vertebrobasilar ischemia [16]. Clinically, patients with OO experience severe neck pain and myelopathy due to craniocervical instability and spinal cord compression. In our study, eight of the 21 subjects complained of neck or suboccipital pain, whereas 13 complained of myelopathy.
The surgical techniques to address OO vary from sublaminar wiring to segmental fixation. The early surgical techniques of Brooks and Jenkins [6] and Gallie [5] achieved variable fusion results [17]. Lowry et al. [7] described a 20% non-union rate with Brooks-type atlantoaxial fusion in patients with OO. To achieve successful fusion, stability reconstruction between C1 and C2 combined with bone grafting is necessary. Transarticular screw fixation with strut grafts produces superior fusion rates than those with sublaminar wiring. Based on a large series of 121 patients, nine of whom had OO, Dickman and Sonntag [17] showed a 98% fusion rate with this technique versus a rate of 86% with posterior wiring. Moreover, Farey et al. [18] showed a 33% instability rate with the Gallie technique using immobilization versus 100% with arthrodesis using transarticular screws in 27 patients, six of whom had OO. To our knowledge, only one study has shown good fusion with this technique [19]. The latest generation of posterior spinal instrumentation is the polyaxial screw-rod system. This approach has been applied to atlantoaxial fusion by Harms and Melcher [11] in a series of 6 patients with OO.
Although there are several reports on C1ŌĆōC2 fusion, few studies have focused on the association between C1ŌĆō2 fixation angle and postoperative subaxial sagittal alignment change. It has been reported that subaxial kyphosis after posterior C1ŌĆō2 fusion is associated with an increased C1ŌĆōC2 fusion angle [12,14,19-23]. Yoshimoto et al. [12] documented that in any type of C1ŌĆōC2 posterior fusion surgery, C1ŌĆōC2 fixation in a hyperlordotic position led to postoperative subaxial kyphosis. Ishii et al. [20] also found that excessive correction of the C1ŌĆōC2 angle may cause postoperative hyperlordosis and lead to the development of subluxations of subaxial spine in RA. Huang et al. [21] investigated the cervical sagittal alignment in non-rheumatoid arthritic patients following posterior C1ŌĆōC2 fusion and identified a correlation between the C1ŌĆōC2 fusion angle and postoperative cervical sagittal alignment. They also found that posterior C1ŌĆōC2 fusion in hyperextension may lead to kyphotic change of the atlantooccipital alignment and increase the forward tilt of the cervical spine. Our results also showed smaller final C0ŌĆōC1 and C2ŌĆōC7 angles in the C1ŌĆōC2 hyperlordotic group (C1ŌĆōC2 fusion angle Ōēź22┬░) than in the group with C1ŌĆōC2 fusion angle <22┬░. Further analyses could potentially reveal that increased posterior C1ŌĆōC2 fusion angle is associated with kyphotic change of occipitocervical and subaxial alignments in patients with OO. Unless the corrected C1ŌĆōC2 angle is satisfied, surgeons should attempt to make an adjustment during the operation. Matsumoto et al. [22] recommended the application of structural interlaminar spacers instead of autologous bone that can maintain a proper cervical angle.
Thus, there is still no consensus regarding the ideal C1ŌĆōC2 fusion angle. Nojiri et al. [23] stated that the mean C1ŌĆōC2 angle in healthy men is 26.5┬░ and that in healthy women is 28.9┬░. Moreover, several investigators have noted that the optimum C1ŌĆōC2 angle for C1ŌĆōC2 fixation should be approximately 20┬░ [14,24]. Kato et al. [24] regarded over-reduction as a C1ŌĆōC2 angle reduction of >20┬░ [25]. Huang et al. [21] also commented the change of postoperative C2ŌĆōC7 angle between final C1ŌĆōC2 angle less than 20┬░ group and more than 22┬░ group. They showed that patients with a correction of >20┬░ in the C1ŌĆōC2 angle are more likely to present a significant postoperative loss of cervical lordosis. We believe that in OO patients with AAI, C0ŌĆōC1 and C2ŌĆōC7 segments have been adapted to the C1ŌĆōC1 kyphosis for a long time. In the present study, the preoperative C1ŌĆōC2 angle was 18.4┬░. Therefore, an acute overcorrection of C1ŌĆōC2 kyphosis can negatively affect C0ŌĆōC1 and C2ŌĆōC7 in the long-term follow-up. Based on our results, we postulate that fusing the C1ŌĆōC2 angle at <22┬░ can decrease the likelihood of sagittal malalignment of C0ŌĆōC1 and C2ŌĆōC7.
This study has certain limitations. First, it is a retrospective case series with a relatively small study population owing to the rarity of this pathologic condition. However, to our knowledge, no study has evaluated >20 cases of OO, especially using a traditional sublaminar wiring technique and/or transarticular screw fixation. Second, we did not include a control group for comparison, such as patients undergoing C1ŌĆōC2 polyaxial screw fixation. Huang et al. evaluated the relation between the C1ŌĆōC2 fusion angle and postoperative cervical alignment using C1ŌĆōC2 segmental fixation [21]. They also reported that over-reduction of the C1ŌĆōC2 angle and hyperlordotic C1ŌĆōC2 fusion leads to sagittal malalignment. Therefore, the results of the present study are also applicable for conventional C1ŌĆōC2 segmental fixation technique.
Fig.┬Ā1.
(A, B) The direction of the AAI was defined as the direction of displacement of the spinolaminar line during flexion and extension. AAI, atlantoaxial instability.
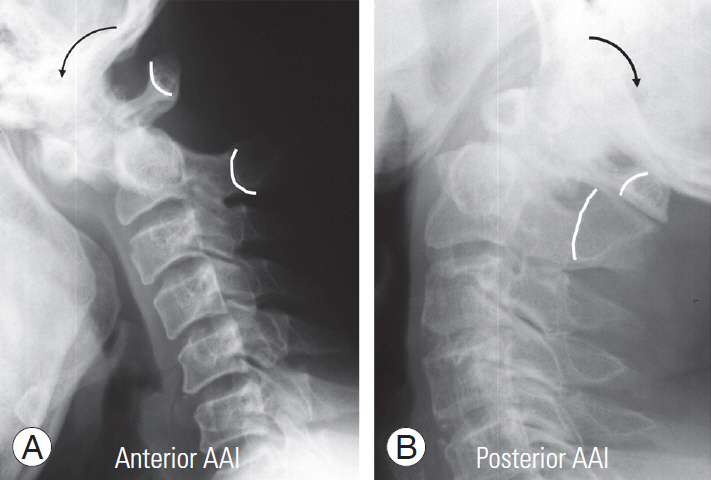
Fig.┬Ā2.
The C0ŌĆōC1, C1ŌĆōC2, and C2ŌĆōC7 angles were measured on neutral (A) lateral radiographs. The C0ŌĆōC1 angle was measured between the McRae line and the line passing through the centers of the C1 anterior and posterior arches. The C1ŌĆōC2 angle was measured between the line passing through the centers of the C1 anterior and posterior arches and line tangential to the inferior border of the C2 body. The C2ŌĆōC7 angle was measured using the Cobb angle between the line on the inferior endplate of C2 and superior endplate of C7. The C0ŌĆōC1, C1ŌĆōC2, and C2ŌĆōC7 range of motions were measured on flexion (B) and extension (C) lateral radiographs.
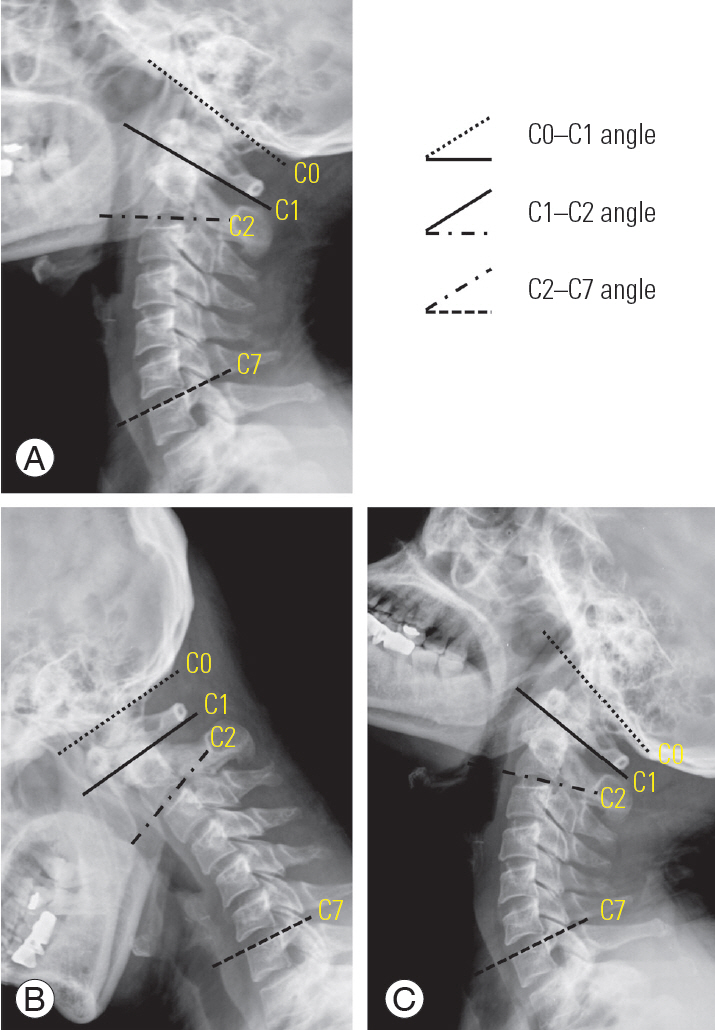
Fig.┬Ā3.
(AŌĆōD) A 44-year-old man with Os odontoideum underwent C1ŌĆōC2 posterior sublaminar wiring and fusion. The C1ŌĆōC2 angle was overcorrected from 23┬░ preoperatively to 30┬░ at the final follow-up. The C0ŌĆōC1 angle decreased from 10┬░ to 9┬░ preoperatively, whereas the C2ŌĆōC7 angle decreased from 10┬░ to ŌłÆ5┬░ at 2 years postoperatively. OP, operative; POD, postoperative day.
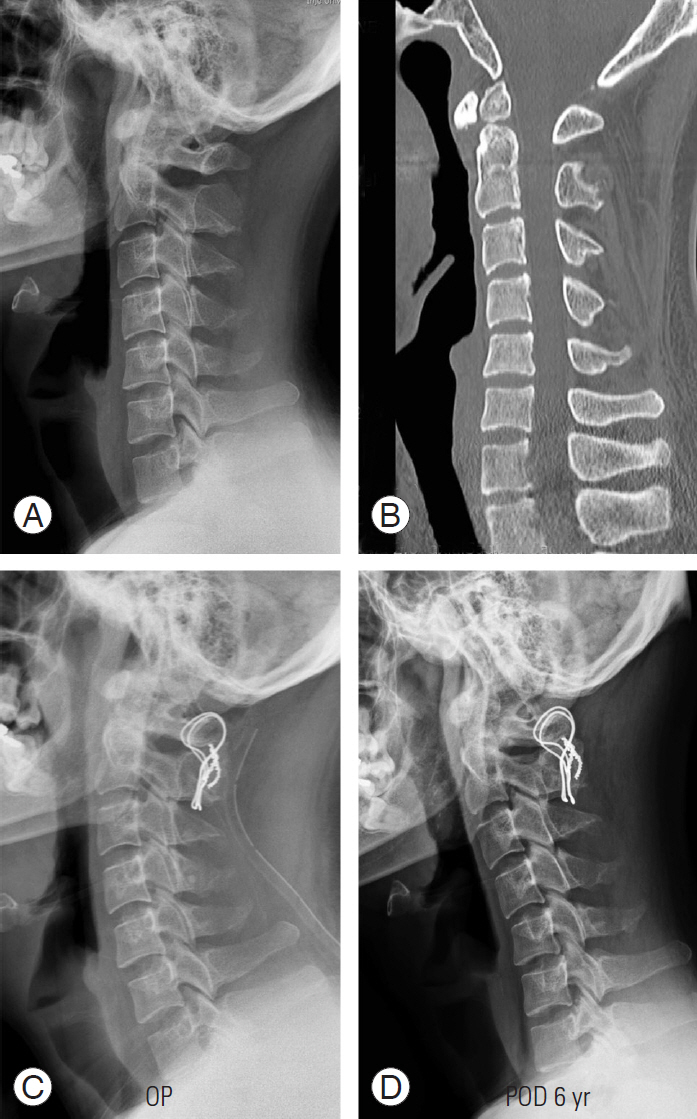
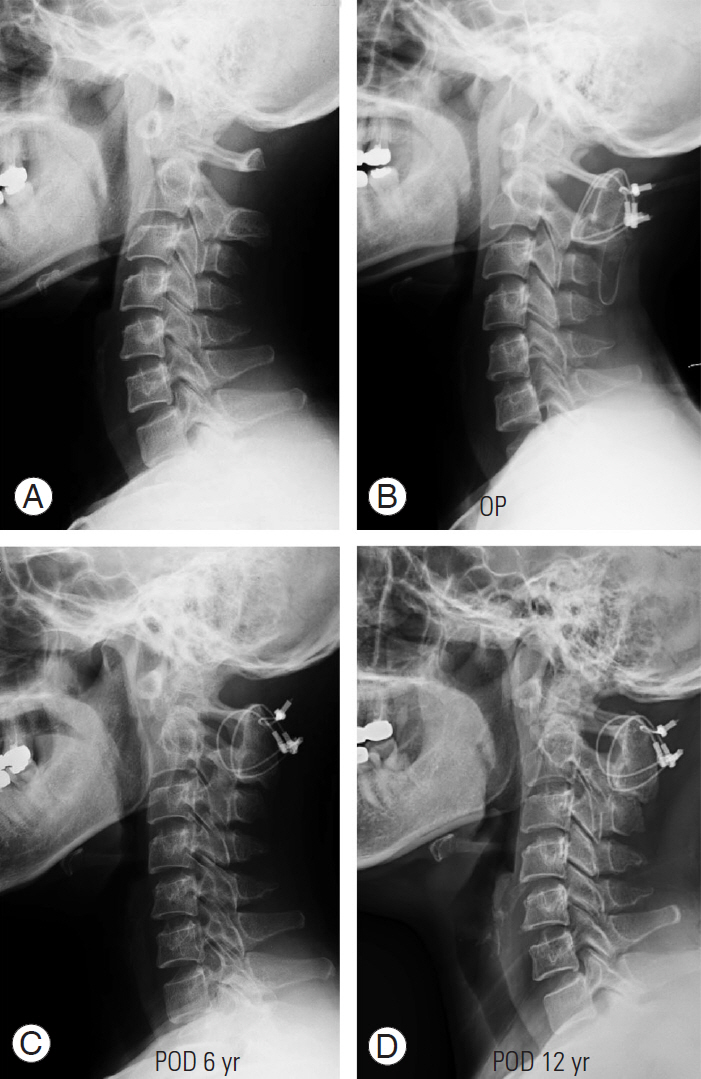
Fig.┬Ā4.
(AŌĆōD) A 36-year-old woman with Os odontoideum underwent C1ŌĆōC2 posterior sublaminar wiring and fusion. The C1ŌĆōC2 angle was maintained from 20┬░ preoperatively to 20┬░ at 12 years postoperatively. Sagittal alignment was well maintained at a C0ŌĆōC1 angle of 10┬░ and C2ŌĆōC7 angle of 22┬░ at 12 years postoperatively. OP, operative; POD, postoperative day.
Table┬Ā1.
Demographic and radiological data according to final C1ŌĆō2 fusion angle
References
1. Klimo P Jr, Kan P, Rao G, Apfelbaum R, Brockmeyer D. Os odontoideum: presentation, diagnosis, and treatment in a series of 78 patients. J Neurosurg Spine 2008 9:332ŌĆō42.


2. Reilly CW, Choit RL. Transarticular screws in the management of C1-C2 instability in children. J Pediatr Orthop 2006 26:582ŌĆō8.


3. Gluf WM, Schmidt MH, Apfelbaum RI. Atlantoaxial transarticular screw fixation: a review of surgical indications, fusion rate, complications, and lessons learned in 191 adult patients. J Neurosurg Spine 2005 2:155ŌĆō63.


4. Ni B, Zhu Z, Zhou F, et al. Bilateral C1 laminar hooks combined with C2 pedicle screws fixation for treatment of C1-C2 instability not suitable for placement of transarticular screws. Eur Spine J 2010 19:1378ŌĆō82.



6. Brooks AL, Jenkins EB. Atlanto-axial arthrodesis by the wedge compression method. J Bone Joint Surg Am 1978 60:279ŌĆō84.


7. Lowry DW, Pollack IF, Clyde B, Albright AL, Adelson PD. Upper cervical spine fusion in the pediatric population. J Neurosurg 1997 87:671ŌĆō6.


8. Magerl F, Seemann P,Stable posterior fusion of the atlas and axis by transarticular screw fixation. Kehr P, Weidner A, editors. Cervical spine I. New York (NY): Springer-Verlag; 1987. p.322ŌĆō7.
9. Yoshida M, Neo M, Fujibayashi S, Nakamura T. Comparison of the anatomical risk for vertebral artery injury associated with the C2-pedicle screw and atlantoaxial transarticular screw. Spine (Phila Pa 1976) 2006 31:E513ŌĆō7.


10. Goel A, Laheri V. Plate and screw fixation for atlanto-axial subluxation. Acta Neurochir (Wien) 1994 129:47ŌĆō53.


11. Harms J, Melcher RP. Posterior C1-C2 fusion with polyaxial screw and rod fixation. Spine (Phila Pa 1976) 2001 26:2467ŌĆō71.


12. Yoshimoto H, Ito M, Abumi K, et al. A retrospective radiographic analysis of subaxial sagittal alignment after posterior C1-C2 fusion. Spine (Phila Pa 197 6) 2004 29:175ŌĆō81.

13. Oshima S, Sudo H, Ito M, Abumi K. Subaxial sagittal alignment after atlantoaxial fixation techniques. J Spinal Disord Tech 2015 28:E49ŌĆō55.


14. Yoshida G, Kamiya M, Yoshihara H, et al. Subaxial sagittal alignment and adjacent-segment degeneration after atlantoaxial fixation performed using C-1 lateral mass and C-2 pedicle screws or transarticular screws. J Neurosurg Spine 2010 13:443ŌĆō50.


15. Kandziora F, Pflugmacher R, Scholz M, et al. Treatment of traumatic cervical spine instability with interbody fusion cages: a prospective controlled study with a 2-year follow-up. Injury 2005 36 Suppl 2:B27ŌĆō35.


17. Dickman CA, Sonntag VK. Posterior C1-C2 transarticular screw fixation for atlantoaxial arthrodesis. Neurosurgery 1998 43:275ŌĆō80.


18. Farey ID, Nadkarni S, Smith N. Modified Gallie technique versus transarticular screw fixation in C1-C2 fusion. Clin Orthop Relat Res 1999 359:126ŌĆō35.

19. Grob D, Crisco JJ 3rd, Panjabi MM, Wang P, Dvorak J. Biomechanical evaluation of four different posterior atlantoaxial fixation techniques. Spine (Phila Pa 1976) 1992 17:480ŌĆō90.


20. Ishii K, Matsumoto M, Takahashi Y, et al. Risk factors for development of subaxial subluxations following atlantoaxial arthrodesis for atlantoaxial subluxations in rheumatoid arthritis. Spine (Phila Pa 1976) 2010 35:1551ŌĆō5.


21. Huang JC, Qian BP, Qiu Y, Yu Y, Ni HB. Surgical overreduction and hyperlordotic fusion of C1-C2 joint are associated with cervical sagittal malalignment. Arch Orthop Trauma Surg 2017 137:1631ŌĆō9.



22. Matsumoto M, Chiba K, Nakamura M, Ogawa Y, Toyama Y, Ogawa J. Impact of interlaminar graft materials on the fusion status in atlantoaxial transarticular screw fixation. J Neurosurg Spine 2005 2:23ŌĆō6.


23. Nojiri K, Matsumoto M, Chiba K, et al. Relationship between alignment of upper and lower cervical spine in asymptomatic individuals. J Neurosurg 2003 99:80ŌĆō3.


- TOOLS






