Introduction
Lumbar spondylolysis is commonly seen at the fourth and fifth lumbar vertebrae. Spondylolysis at the fourth and fifth lumbar vertebrae accounts for more than 95% of the total cases of spondylolysis1. However, multiple lumbar spondylolysis is an unusual and relatively rare finding. The incidence of multiple lumbar spondylolysis appears to vary between 1.2%2,3 to 5.6%4. Al-Sebai and Al-Khawashki5 have previously had reported on a rare case of bilateral three level lumbar spondylolysis that was associated with one level spondylolisthesis. We report here on a rare case of asymmetric four level lumbar spondylolysis.
Case Report
A 19-year-old Korean woman visited our out-patient clinic for severe back pain that had developed spontaneously. The patient was a student at the college of physical education. The patient initially noticed a kyphosis in the lumbar area around three years ago. However, since it was not associated with any significant disability or pain, she was treated conservatively at that time. Yet after a routine exercise program for entering the college of physical education, she developed low back pain for which she was prescribed oral medication. However, the back pain did not improve with the oral analgesics and it started to increase in intensity.
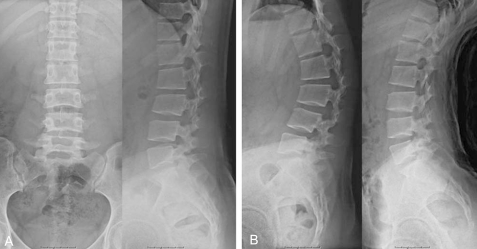
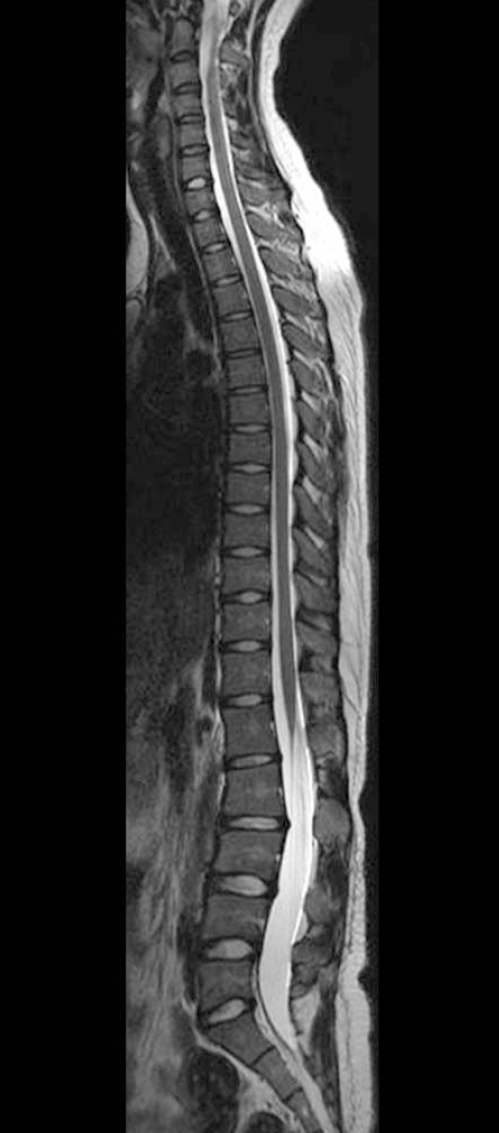
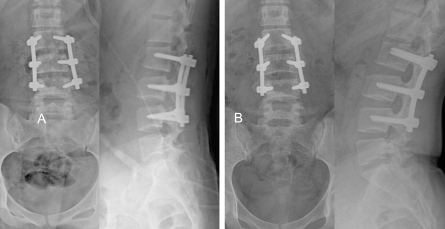
At the time of presentation at our outpatient clinic, a lumbar kyphosis was noticed in the standing position. Grossly, the kyhosis and instability of the lower back were moderate to severe. The kyphosis was found to be flexible because the kyphosis could be corrected when the low back area was pushed anteriorly by the surgeon's hands. She had severe lower back pain. The visual analogue score (VAS) was 8 points. The patient also showed generalized ligamentous laxity. There were no neurological signs or symptoms. The initial radiographs showed a hypoplastic change in the spinous processes and lamina of the lumbar vertebrae, multiple spondylolysis and lumbar instability (Fig. 1). The magnetic resonance imaging (MRI) demonstrated the presence of kyphosis of the upper lumbar spine and multiple levels of spondylolysis (Fig. 2). A three dimensional computed tomography (CT) scan was performed to get a complete picture of the lesions. The CT scan showed asymmetric complete spondylolysis at the left L2/3/4 levels (Fig. 3A) and the right L1/2/3 levels (Fig. 3B). The activities of daily living were severely limited, and so a surgical operation was performed. Obvious instability of the L2/3/4 segments was noted intraoperatively. The pars interarticularis of L2/3/4 were dystrophic, so defect repair was impossible. Posterior lumbar interbody fusion was not chosen. Because the patient had no neurologic symptoms, we did not need to open the neural canal, and laminectomy was not done. A two level posterior and posterolateral fusion was carried out at the L2/3/4 levels with intersegmental fixation by using pedicle screws and an auto iliac bone graft (Fig. 4A). The harvest site of the auto iliac bone was located beneath the Bikini line. The preoperative segmental angle of the operated levels was 15 degrees of kyphosis while the postoperative angle for the fused segment was 8 degrees of lordosis. After operation, the patient's lower back pain was much relieved and the VAS was 4 points. The postoperative 1 year follow-up of the patient showed no neurological deficit, no lumbar instability and no hardware failure (Fig. 4B). There was a very good improvement of her symptoms and she was satisfied with the cosmetic result. The patient was completely relieved of lower back pain after the surgery, and the VAS was 2 points.
Discussion
Lumbar spondylolysis is common at the fourth and fifth lumbar vertebrae. The frequency of spondylolysis in the upper lumbar vertebrae has been estimated by various authors to be between 0.2% and 1.5%6. Two factors play a determinant role in the pathogenesis of spondylolysis: the genetic factor and the mechanical factor of the lumbar spine. Familial occurrence of spondylolysis has been demonstrated by Friberg7 and Willis8 and Wiltse9, and it supports that a genetic factor can be involved with this malady, but the specific gene that affects spondylolysis is unknown. The spondylolysis is not present in embryos, the fetus or at birth and it usually appears as soon as the child begins to stand and walk9. Pfeil10 found 17 cases of spondylolisthesis and spondylolysis among 500 children. In the report by Wiltse, the youngest patient with spondylolysis was eight and a half months. It is thought that spondylolysis is associated with the upright position. There may be a relation between repetitive trauma and spondylolysis. People employed in heavy industry and people who participate in contact sports seem to be particularly vulnerable to this condition11,12. So, multiple spondylolysis is more commonly seen among men. In our case, the patient's symptoms were aggravated after a routine exercise program. We consider that the mechanical factor of the lumbar spine affects a development of spondylolysis for people who are vulnerable due to a genetic factor. In a study of lumbar spondylolysis among 1598 subjects, only two were found to have lesions in the upper three lumbar vertebrae13. Furthermore, multi-level spondylolysis at the upper lumbar vertebra is even rarer, and in these case reports, a diagnosis of multiple spondylolysis was made according to the plain radiography14. Various radiological modalities like plain radiography, CT and MRI are useful for diagnosing spondylolysis. On the plain radiography, the dynamic flexion-extension views are very useful for assessing the vertebral stability. Three-dimensional (3D) CT reconstruction has greatly increased the reliability and value of a CT examination15. In our case, we could confirm the levels of lumbar spondylolysis by using three dimensional CT. We consider that three dimensional CT is a very good and useful tool for the diagnosis of multiple spondylolysis and for making the decision on what level to fuse. In our case, because the patient had constant severe lower back pain for a long time and a spinal deformity and severe instability had developed, the patient underwent a single stage posterolateral fusion and instrumentation. After the operation, the patient was free from her pain and spinal instability. We report here on a well-treated case of multiple spondylolysis.