|
 |
- Search
| Asian Spine J > Volume 13(2); 2019 > Article |
|
Abstract
Purpose
Overview of Literature
Methods
Results
Acknowledgments
Notes
Author Contributions
Masayuki Ohashi wrote and prepared the manuscript. Masayuki Ohashi, Kei Watanabe, Toru Hirano, Kazuhiro Hasegawa, Keiichi Katsumi, Hirokazu Shoji, and Tatsuki Mizouchi contributed to the conception and design of this study, data acquisition, and analysis and interpretation of the data. Takao Homma and Naoto Endo contributed to the study design, analysis and interpretation of data, and supervision. All authors have read, reviewed, and approved the article.
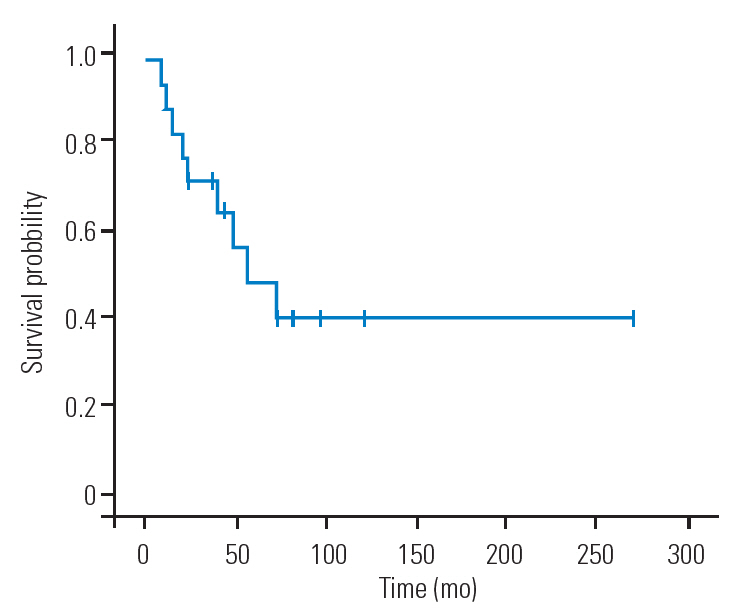
Fig.┬Ā1.

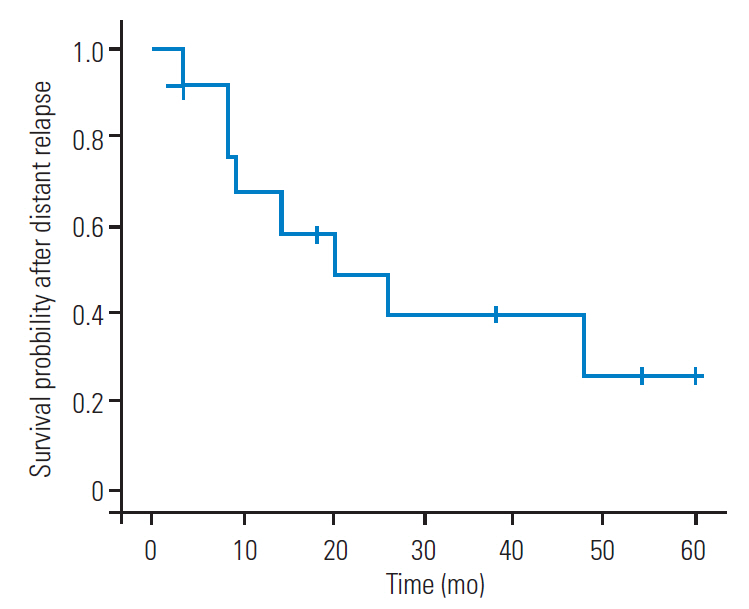
Fig.┬Ā2.
Table┬Ā1.
Table┬Ā2.
| Case | Date of EBS (yr) | Approach | Resected areaa) | Time (min) | Intraoperative blood loss (g) | Adjuvant therapy |
Perioperative complications |
Frankel gradeb) | |
|---|---|---|---|---|---|---|---|---|---|
| Intraoperative | Postoperative | ||||||||
| 1 | 1991 | C-AP | T6 | 715 | 4,300 | None | None | Pneumonia | E |
| 2 | 1995 | C-AP | T12 | 680 | 2,625 | C+RAI | None | None | E |
| 3 | 2001 | C-AP | T9, 10, 11 | 1,073 | 3,478 | None | None | Paralytic ileus | D |
| 4 | 2001 | P | T (6), 7, (8) | 1,067 | 410 | R | None | Pneumonia | D |
| 5 | 2004 | C-AP | T6, (7) | 713 | 1,744 | None | None | None | E |
| 6 | 2004 | S-AP | T10, (11) | 1,015 | 18,070 | None | None | ND, UTI | D |
| 7 | 2005 | S-AP | L3 | 922 | 3,891 | C | None | None | E |
| 8 | 2007 | S-AP | T8, 9, 10 | 1,110 | 2,125 | C | None | ND, SSI | E |
| 9 | 2008 | S-AP | (T12), L1 | 834 | 8,245 | C | Durotomy | SSI | D |
| 10 | 2009 | S-AP | T9 | 627 | 1,670 | C | None | None | E |
| 11 | 2010 | S-AP | T12 | 755 | 1,235 | None | None | None | E |
| 12 | 2011 | S-AP | L (2), 3, (4) | 632 | 7,512 | RAI | Durotomy | None | E |
| 13 | 2012 | S-AP | L5 | 881 | 3,215 | R | Vena cava tear | ND, DVT | E |
| 14 | 2013 | S-AP | T12, L1 | 780 | 1,715 | None | Durotomy | None | D |
| 15 | 2013 | S-AP | T12 | 609 | 1,790 | None | Durotomy | None | E |
| 16 | 2014 | P | T12 | 447 | 1,180 | None | None | None | E |
| 17 | 2014 | S-AP | T11, 12 | 783 | 330 | C | None | SSI | E |
| 18 | 2015 | S-AP | L (1), 2 | 712 | 3,245 | None | Aorta and vena cava tear | SSI | D |
EBS, en bloc spondylectomy; C-AP, combined anterior and posterior approach; C, chemotherapy or hormonal therapy; RAI, radioactive iodine therapy; P, posterior approach; R, radiation therapy; S-AP, simultaneous anterior and posterior approach; ND, neurological deficits; UTI, urinary tract infection; SSI, surgical site infection; DVT, deep venous thrombosis.