 |
 |
- Search
| Asian Spine J > Volume 13(3); 2019 > Article |
|
Abstract
Purpose
The study aimed to analyze mechanisms underlying chronic low back pain (CLBP) using magnetic resonance imaging (MRI) T2 mapping of the intervertebral disc (IVD).
Overview of Literature
MRI T2 mapping utilizes the T2 values for quantifying moisture content and collagen sequence breakdown. We previously used MRI T2 mapping for quantifying the extent of IVD degeneration (IVDD) and showed a correlation between the degeneration of the posterior annulus fibrosus (AF) and CLBP.
Methods
We enrolled 40 patients with CLBP (17 males, 23 females; mean age, 50.8┬▒1.6 years; range, 22ŌĆō60 years). IVDs were categorized as the anterior AF, nucleus pulposus (NP), and posterior AF, and T2 value for each disc was measured. T2 values, assessed using the Japanese neuropathic pain (NeP) screening questionnaire, of the NeP and nociceptive pain (NocP) groups were compared.
Results
T2 values of the NocP and NeP groups were 64.7┬▒5.6 ms and 58.1┬▒2.3 ms for the anterior AF; 67.0┬▒4.6 ms and 59.6┬▒2.1 ms for NP; and 70.7┬▒4.6 ms and 51.0┬▒1.2 ms for the posterior AF, respectively. T2 values for IVDD were significantly lower in the NeP group than those in the NocP group (p<0.01).
Low back pain (LBP), a frequently observed condition, is one of the most serious physiological issues worldwide [1]. Various problems in any part of the complex such as the interconnected network of spinal muscles, bones, discs, nerves, or tendons in the lumbar spine can cause LBP. Intervertebral disc (IVD) degeneration (IVDD) is considered to be the primary condition causing LBP [2]. Many studies have reported on discogenic LBP considering its pathology, diagnosis, and treatment; however, the underlying mechanism and treatments are still to be elucidated. Reportedly, discography is used for supporting the diagnosis of discogenic pain; however, it has a high false-positive rate [3] and is associated with risks that accelerate IVDD [4].
Pain symptoms including LBP are classified into two broad categories based on the mechanism of pain: neuropathic pain (NeP) caused by nervous system injury and nociceptive pain (NocP) caused by tissue-injury and/or inflammation [5,6]. Since different type of pains require different treatment approaches [7], early identification of NeP involvement in patients with chronic pain is crucial for appropriate management [8].
Magnetic resonance imaging (MRI) is an important modality for diagnosing degenerative IVD. Signal variation of the discs observed on T2-weighted images corresponds to the disc age and degeneration and allows for the determination the extent of disc degeneration. Specifically, since MRI signal strength is associated with moisture and proteoglycan content, changes in the MRI signal strength of the nucleus pulposus (NP) can indicate IVDD [9,10]. IVDD has been classified using T2-weighted images using the classification system described by Pfirrmann et al. [11], but since this classification is based on visual evaluation, quantifying disc degeneration using this strategy is unclear. Recently, several attempts have been made to utilize MRI T2 and MRI T1p mappings for quantifying lumbar disc degeneration [12-15]. MRI T2 mapping utilizes T2 relaxation time for quantifying moisture content and collagen sequence breakdown. Previously, we used MRI T2 mapping for quantifying the extent of IVDD and demonstrated a significant correlation using the Pfirrmann classification [14]. Furthermore, we quantitatively evaluated IVDD with MRI T2 mapping and demonstrated a correlation between the degeneration of the posterior annulus fibrosus (AF) and chronic LBP (CLBP) [15].
Thus, this study aimed to analyze pain mechanisms underlying discogenic LBP using MRI T2 mapping.
The institutional review board of the Sapporo Medical University approved this study (IRB approval no., 262-1074). All subjects were provided with written and verbal explanations of the study prior to obtaining their consent before participating in the study.
This study enrolled patients with non-specific CLBP, which was defined as pain, stiffness, and discomfort of the lower back from the 12th rib to the lumbar or lumbosacral area, whose source was difficult to identify, and whose symptoms persisted even following conservative treatment including medication or therapeutic exercise for >3 months. Patients with neoplasm, infection, fracture, or a history of lumbar vertebral surgery were excluded. Additionally, patients with neurologic symptoms of the lower leg or obvious instability, which could be identified as a source of LBP and may improve with surgical treatment, were excluded. Intervertebral instability was defined as a sagittal posterior opening of >5┬░ on flexion/extension radiographs or a translation of >3 mm or segmental motion of >20┬░. The severity of LBP was assessed using the Visual Analog Scale (VAS, 0ŌĆō100) and Japanese NeP Screening Questionnaire after 4 weeks of a washout period of at least 4 weeks [16] (Table 1). Patients with a Japanese NeP Screening Questionnaire score of Ōēź4 and <4 points were categorized in the NeP and NocP groups, respectively.
Standard VAS scores for diagnosing patients with LBP are not clearly defined. A previous study diagnosed LBP when the VAS score of patients was >30 mm; therefore, in this study, patients with VAS scores were >30 mm were diagnosed with LBP. Patients underwent MRI to detect disc degeneration. The clinical radiologist examined and graded MRI T2-weighted images of the five lumbar discs in the midsagittal section as I to V using the Pfirrmann classification [11]. Patients who had disc degeneration at L4ŌĆō5 level of grade III to V were screened. Other disc degenerations were graded I to II, as it is likely that L4ŌĆō5 disc degenerations are the source of discogenic LBP. Finally, 40 patients (17 males, 23 females; mean age, 50.8┬▒1.6 years; range, 22ŌĆō60 years) were enrolled. The distribution of T2-weighted image-based Pfirrmann grade classifications was as follows: grade III, 16 discs; grade IV, 21 discs; and grade V, 3 discs.
In this study, previously described MRI protocol and analysis methods were used for MRI T2 mapping [14,15]. MRI examinations were performed using a 1.5 Tesla whole-body scanner (Signa HDxt; GE Healthcare, Milwaukee, WI, USA) using a spine coil. Briefly, a T2 map was created using T2 values in the midsagittal section from sagittal sections centered on the lumbar midline region with an optimized 8 echo multi-spin echo (repetition time/first echo time [TE], 1,000/14.8; last echo TE, 118.6; receiver bandwidth, ┬▒15.63 kHz; field-of-view, 22 cm; matrix, 320├Ś256; slice thickness/gap, 4 mm/4 mm, 5 slices; number of excitations, 2; total scan time, 8 minutes and 34 seconds) obtained using the Advantage Workstation (version 4.4, Functool; GE Healthcare). However, first echo from the multi-spin system was excluded so as to minimize the effect of the stimulated echo. The T2 map was determined in each pixel from the signal intensity (SI) in the respective TE using the following formula: SI 1Ōüä4 e_TE=T2.
For assessment, the IVD was divided into five equal areas based on previous studies: the front fifth was designated as the anterior AF, the middle fifth as the NP, and the last fifth as the posterior AF [14,15]. Mean T2 values in the region of interest (ROI) were measured by a researcher (H.T.) using the MedCalc ver. 10.2.0.0 (MedCalc Software, Mariakerke, Belgium) (Fig. 1). The number of pixels for the selected ROI was a minimum of 152 and a maximum of 416. Second-echo images of MRI T2 mapping of patients with NocP and those with NeP are presented in Fig. 2A and 2B, respectively.
T2 values of the NeP and NocP groups were compared. Demographic data concerning the number of males and females were analyzed using the chi-square test. Differences among groups were compared using the MannŌĆōWhitney U-test. A p-value of <0.05 indicated statistical significance. All numerical data are expressed as mean┬▒standard error of the mean.
As shown in Table 2 and Fig. 3, the patients were categorized into the NocP (n=25) and NeP (n=15) groups. The study cohort comprised an almost equal number of males and females, with no significant difference (p=0.80). Moreover, mean age was not statistically significant between the groups (p=0.62). Average values of NeP scores were 2.1┬▒0.2 and 5.8┬▒0.3 in the NocP and NeP groups, respectively.
T2 values for IVD in the NocP and NeP groups are shown in Fig. 4. T2 values for the NocP and NeP groups were 64.7┬▒5.6 ms and 58.1┬▒2.3 ms for the anterior AF (Fig. 4A), 67.0┬▒4.6 ms and 59.6┬▒2.1 ms for NP (Fig. 4B), and 70.7┬▒4.6 ms and 51.0┬▒1.2 ms for the posterior AF, respectively (Fig. 4C). T2 values for IVD were significantly lower in the NeP group than those in the NocP group for the posterior AF (p<0.01).
Non-specific LBP is estimated to account for >85% of all LBP cases [1]. IVDD was previously considered to be the source of non-specific LBP. Schwarzer et al. [17] suggested that 39% of CLBP patients had a discogenic origin of their pain. LBP, which was characterized by pain aggravation in a flexure posture, provided an insight to guide diagnosis, but such findings are less objective and specific. Furthermore, the diagnosis of neuropathic components in LBP is more difficult considering that there exists no gold standard examination for such diagnoses. The diagnostic value of clinical interview, physical examination, and imaging analysis has not been well documented. Previous studies show that NeP is often underdiagnosed and undertreated [18]. Therefore, no specific diagnostic method has been established; as a result, diagnosis and subsequent treatment of this condition is difficult.
MRI is an important imaging technique for diagnosing structural changes in the spinal column. Recent studies have attempted to quantitatively assess and associate IVDD with LBP using MRI techniques such as MRI T2 mapping and MRI T1p mapping [12-14]. In studies using MR relaxometry, increased disc moisture or glycosaminoglycan content, the primary component of proteoglycan, is associated with increased T2 values whereas increased collagen content is associated with decreased T2 values [19]. Recently, some studies have reported that T2 values for the AF decrease with disc degeneration. Welsch et al. [20] demonstrated that the spatial variation (defined by an increase in T2 values from the AF to the NP) was the highest for Pfirrmann grade I IVDD and reduced with increasing Pfirrmann grade (II to IV) IVDD. They explained that the AF is composed of fibro-cartilage and functions as a rigid containment for the NP owing to its fibrous structure comprising collagen lamellae and low moisture content. With IVDD, the collagen lamellae of the AF increases in thickness and becomes fibrillated. Therefore, the fibrillated collagen of the AF is associated with a decrease in T2 values. In the present study, we used MRI T2 mapping of IVD in patients with CLBP to quantitatively investigate a difference between the NocP and NeP groups. The results revealed that T2 values for posterior AF were significantly lower in the NeP group than those in the NocP group. Sinuvertebral nerves originate from spinal nerve roots and are distributed around the posterior AF region. Thus, this area is richly innervated. Freemont et al. [21] reported that the presence of sensory nerve fibers in the deeper layer of the AF may result in discogenic LBP in patients with IVDD. In addition, Kojima et al. [22,23] reported that sinuvertebral nerves innervate both the shallow and deep layers around the posterior longitudinal ligament area. As deep-layer fibers are segmentally located in intervertebral areas of the posterior longitudinal ligament, these fibers control posterior fiber rings. Nakamura et al. [24] reported that when sympathetic nerve trunks were removed from rats, the intervertebral posterior nerve decreased, suggesting that intervertebral posterior nerve fibers pass through the sympathetic nerve trunk. Ohtori et al. [25,26] anteriorly inserted needles with nerve tracers into rat IVDs and demonstrated that the posterior AF was controlled by sinus spinal and sympathetic nerves. Using rat models of IVD compression and injury, Miyagi et al. [27] demonstrated that repetitive trauma or mechanical stress resulted in a long-lasting increase in the levels of inflammatory mediators in IVD and this increase may eventually lead to the pathogenesis of inflammatory pain and long-lasting increase in calcitonin gene-related peptide expression in the sensory nervous system. This could contribute to pain state, neuronal damage, and nerve regeneration, ultimately aiding NeP pathogenesis. Lower T2 values for the posterior AF implied a more severe degeneration. Therefore, results of this study implied that the degeneration of the posterior AF, which is richly innervated with afferent nerve fibers, is more severe in the NeP group than that in the NocP group.
The prevalence of NeP was 37.5% (NocP: n=25; NeP: n=15) in this study. A nationwide study in Japan previously reported that 53.3% of patients with chronic pain related to spine-related disorders presented with NeP, and 29.4 % of patients with LBP were diagnosed with NeP [28]. This high ratio highlights the necessity to appropriately identify NeP in such patients to facilitate appropriate and early treatment. In clinical settings, the findings of this study have important implications for formulating targeted analgesic therapies. Accurate understanding of the mechanism underlying CLBP and appropriate prescription may result in better patient-oriented pain control. Invasive discography has been conventionally used to evaluate discogenic LBP and can cause pain due to the injection of contrast fluid between IVDs and has a high false-positive rate. Therefore, invasive discography is not entirely suitable as a modality for identifying the source of LBP [3,29,30]. Moreover, discography has been reported to cause the progression of IVDD [4]. To the best of our knowledge, there are no reports regarding the efficacy of discography for the diagnosis of NeP. Meanwhile, MRI T2 mapping is a noninvasive quantitative evaluation modality that offers high reproducibility in contrast to discography. The results of the present study suggest that MRI T2 mapping is a quantitative method for diagnosing discogenic pain considering NeP.
This study has several limitations. The Japanese NeP screening questionnaire used in this study may be an inadequate diagnostic utility for detecting NeP caused by spinal disorders [31]. Further studies utilizing an NeP screening tool that specializes in detecting NeP caused by spinal disorders such as the Spine painDETECT questionnaire are warranted [32]. Moreover, there is no evidence justifying that non-specific LBP in the patients enrolled in this study originates from L4ŌĆō5 disc degeneration.
Notes
Author Contributions
Conception and design: Ogon I, Takebayashi T, Takashima H; acquisition of data: Ogon I, Takashima H; analysis and interpretation of data: Ogon I, Takashima H; drafting the article: Ogon I, Takebayashi T; critically revising the article: all authors; reviewed submitted version of manuscript: all authors; approved the final version of the manuscript on behalf of all authors: Takebayashi T; statistical analysis: Ogon I; administrative/technical/material support: Morita T, Iesato N, Tanimoto K, Terashima Y, Yoshimoto M, Yamashita T; and study supervision: Yamashita T.
Fig.┬Ā1.
In the second-echo image, the disc was divided into five areas, designating the front as the anterior AF, the middle as the nucleus pulposus, and the last as the posterior AF (A). Mean T2 values in this region were measured (B). AF, annulus fibrosus.

Fig.┬Ā2.
The second-echo image of magnetic resonance imaging T2 mapping of patients with nociceptive pain (A) and those with neuropathic pain (B).
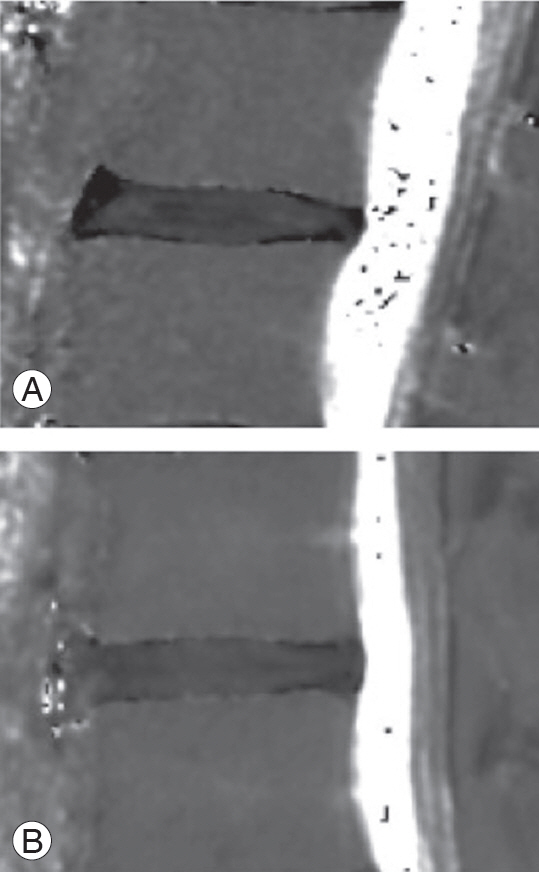
Fig.┬Ā3.
Distribution of NeP score. Patients were categorized into NocP (n=25) and NeP (n=15) groups. NeP, neuropathic pain, NocP, nociceptive pain.
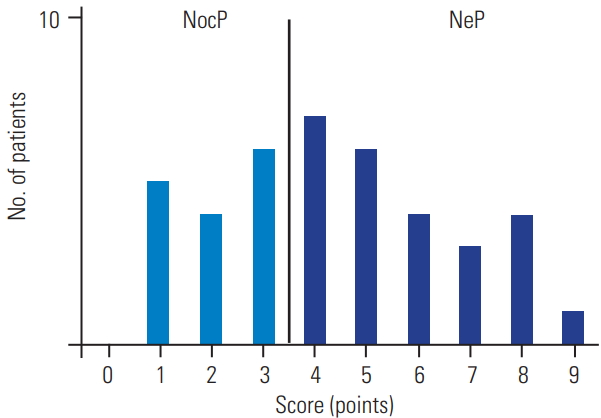
Fig.┬Ā4.
Comparisons of T2 values for the NocP and NeP groups. T2 values for the anterior AF (A), NP (B), and posterior AF (C) in the NeP group were lower than those in the NocP group; T2 values for the posterior AF significantly differed between the groups. NocP, nociceptive pain; NeP, neuropathic pain; AF, annulus fibrosus. *p<0.01.

Table┬Ā1.
Questions on the nature of pain
References
3. Carragee EJ, Tanner CM, Yang B, Brito JL, Truong T. False-positive findings on lumbar discography: reliability of subjective concordance assessment during provocative disc injection. Spine (Phila Pa 1976) 1999 24:2542ŌĆō7.


4. Carragee EJ, Don AS, Hurwitz EL, Cuellar JM, Carrino JA, Herzog R. 2009 ISSLS Prize winner: does discography cause accelerated progression of degeneration changes in the lumbar disc: a ten-year matched cohort study. Spine (Phila Pa 1976) 2009 34:2338ŌĆō45.


5. Woolf CJ, Bennett GJ, Doherty M, et al. Towards a mechanism-based classification of pain? Pain 1998 77:227ŌĆō9.


6. Freynhagen R, Baron R, Tolle T, et al. Screening of neuropathic pain components in patients with chronic back pain associated with nerve root compression: a prospective observational pilot study (MIPORT). Curr Med Res Opin 2006 22:529ŌĆō37.


7. Baron R, Binder A, Wasner G. Neuropathic pain: diagnosis, pathophysiological mechanisms, and treatment. Lancet Neurol 2010 9:807ŌĆō19.


8. Haanpaa ML, Backonja MM, Bennett MI, et al. Assessment of neuropathic pain in primary care. Am J Med 2009 122:S13ŌĆō21.


9. Urban JP, McMullin JF. Swelling pressure of the lumbar intervertebral discs: influence of age, spinal level, composition, and degeneration. Spine (Phila Pa 1976) 1988 13:179ŌĆō87.


10. Zou J, Yang H, Miyazaki M, et al. Dynamic bulging of intervertebral discs in the degenerative lumbar spine. Spine (Phila Pa 1976) 2009 34:2545ŌĆō50.


11. Pfirrmann CW, Metzdorf A, Zanetti M, Hodler J, Boos N. Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine (Phila Pa 1976) 2001 26:1873ŌĆō8.


12. Perry J, Haughton V, Anderson PA, Wu Y, Fine J, Mistretta C. The value of T2 relaxation times to characterize lumbar intervertebral disks: preliminary results. AJNR Am J Neuroradiol 2006 27:337ŌĆō42.


13. Zuo J, Joseph GB, Li X, et al. In vivo intervertebral disc characterization using magnetic resonance spectroscopy and T1Žü imaging: association with discography and Oswestry Disability Index and Short Form-36 Health Survey. Spine (Phila Pa 1976) 2012 37:214ŌĆō21.



14. Takashima H, Takebayashi T, Yoshimoto M, et al. Correlation between T2 relaxation time and intervertebral disk degeneration. Skeletal Radiol 2012 41:163ŌĆō7.


15. Ogon I, Takebayashi T, Takashima H, et al. Analysis of chronic low back pain with magnetic resonance imaging T2 mapping of lumbar intervertebral disc. J Orthop Sci 2015 20:295ŌĆō301.


16. Ogawa S. Development of new screening questionnaire to identify neuropathic components in Japanese patients with chronic pain. Pain Clin 2010 31:1187ŌĆō94.
17. Schwarzer AC, Aprill CN, Bogduk N. The sacroiliac joint in chronic low back pain. Spine (Phila Pa 1976) 1995 20:31ŌĆō7.


19. Nightingale T, MacKay A, Pearce RH, Whittall KP, Flak B. A model of unloaded human intervertebral disk based on NMR relaxation. Magn Reson Med 2000 43:34ŌĆō44.


20. Welsch GH, Trattnig S, Paternostro-Sluga T, et al. Parametric T2 and T2* mapping techniques to visualize intervertebral disc degeneration in patients with low back pain: initial results on the clinical use of 3.0 Tesla MRI. Skeletal Radiol 2011 40:543ŌĆō51.


21. Freemont AJ, Peacock TE, Goupille P, Hoyland JA, OŌĆÖBrien J, Jayson MI. Nerve ingrowth into diseased intervertebral disc in chronic back pain. Lancet 1997 350:178ŌĆō81.


22. Kojima Y, Maeda T, Arai R, Shichikawa K. Nerve supply to the posterior longitudinal ligament and the intervertebral disc of the rat vertebral column as studied by acetylcholinesterase histochemistry: I. distribution in the lumbar region. J Anat 1990 169:237ŌĆō46.


23. Kojima Y, Maeda T, Arai R, Shichikawa K. Nerve supply to the posterior longitudinal ligament and the intervertebral disc of the rat vertebral column as studied by acetylcholinesterase histochemistry: II. regional differences in the distribution of the nerve fibres and their origins. J Anat 1990 169:247ŌĆō55.


24. Nakamura S, Takahashi K, Takahashi Y, Morinaga T, Shimada Y, Moriya H. Origin of nerves supplying the posterior portion of lumbar intervertebral discs in rats. Spine (Phila Pa 1976) 1996 21:917ŌĆō24.


25. Ohtori S, Takahashi Y, Takahashi K, et al. Sensory innervation of the dorsal portion of the lumbar intervertebral disc in rats. Spine (Phila Pa 1976) 1999 24:2295ŌĆō9.


26. Ohtori S, Takahashi K, Chiba T, Yamagata M, Sameda H, Moriya H. Sensory innervation of the dorsal portion of the lumbar intervertebral discs in rats. Spine (Phila Pa 1976) 2001 26:946ŌĆō50.


27. Miyagi M, Ishikawa T, Kamoda H, et al. ISSLS Prize winner: disc dynamic compression in rats produces long-lasting increases in inflammatory mediators in discs and induces long-lasting nerve injury and regeneration of the afferent fibers innervating discs: a pathomechanism for chronic discogenic low back pain. Spine (Phila Pa 1976) 2012 37:1810ŌĆō8.


28. Yamashita T, Takahashi K, Yonenobu K, Kikuchi S. Prevalence of neuropathic pain in cases with chronic pain related to spinal disorders. J Orthop Sci 2014 19:15ŌĆō21.


29. Carragee EJ, Paragioudakis SJ, Khurana S. 2000 Volvo Award winner in clinical studies: lumbar high-intensity zone and discography in subjects without low back problems. Spine (Phila Pa 1976) 2000 25:2987ŌĆō92.


30. Carragee EJ, Hannibal M. Diagnostic evaluation of low back pain. Orthop Clin North Am 2004 35:7ŌĆō16.


- TOOLS
-
METRICS

- Related articles in ASJ
-
Magnetic Resonance Imaging of the Lumbar Spine in Young Arabs with Low Back Pain2012 December;6(4)





