Introduction
Spondylolysis is a condition defined as a bony defect at the pars interarticularis in the spine [12]. Lumbar spondylolysis is not a rare condition and is reported to occur in around 6% of the general population [345]. In contrast, cervical and thoracic spondylolysis is an uncommon entity [6], and in regard to axis (C2) spondylolysis, only 30 cases have been reported in the literature [17]. The etiology of spondylolysis has not been established, with congenital and a fatigue fracture, but many clinical studies have supported a stress fracture [8].
In patients with lumbar spondylolysis, spondylolisthesis with or without low back pain sometimes occurs once the pars defect is completed [910]. Also, proliferative changes around the pars defects sometimes produce radiculopathy by compressing the nerve root, and surgical treatment is required [11]. In patients with cervical spondylolysis, myelopathy caused by instability or slippage has been reported [1]. However, no English literature has described a case with myelopathy due to proliferative changes around pars defects.
In this paper, we present a case of C2 spondylolysis with myelopathy caused by proliferative changes around the pars defects on the C2 lamina, and not caused by instability.
Case Report
1. History
A 69-year-old male had an 8-year history of paresthesia from forearm to hand on the right side with no experience of any obvious traumatic episodes. He was referred to our hospital because of progressive difficulty in walking and numbness in his extremities.
2. Physical examination
Physical examination revealed normal strength in all limbs but clumsy hands and bilateral numbness on both arms. The deep tendon reflexes were hyperactive bilaterally below C5 level and his gait was spastic. Pathological reflexes including scapulohumeral reflex, Hoffmann's sign, Wartenberg's sign, and Babinski's sign were negative and he had no bladder and bowel dysfunctions.
3. Radiological findings
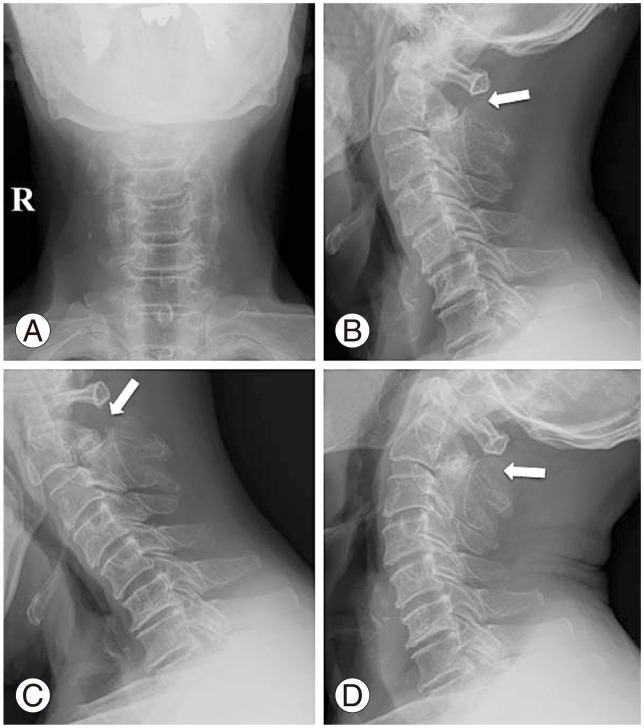
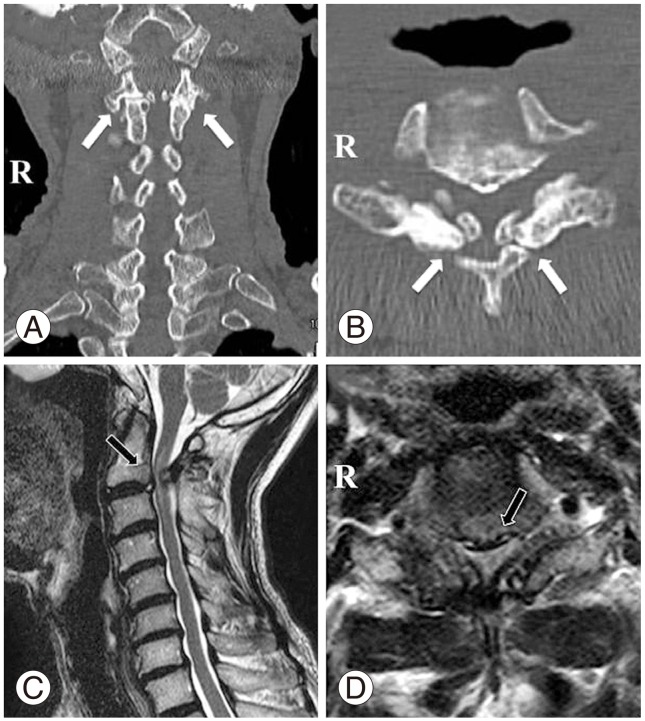
Plain radiographs of the cervical spine showed bilateral spondylolysis at C2 and bony fusion between the C2 and C3 spinous processes (Fig. 1A, B). Dynamic views revealed mobility between C2 and C3 through the spondylolysis. Obvious intervertebral instability was not found at any spinal levels (Fig. 1C, D). Computed tomography (CT) of the cervical spine revealed a sclerotic margin with a triangular configuration of the pillar fragments on both sides the spondylolytic defect. Proliferative "ragged edge" changes were detected around the bilateral pars defects, which protruded into spinal canal (Fig. 2A, B). Magnetic resonance imaging (MRI) of the cervical spine revealed cervical spinal canal stenosis. The spinal cord was severely compressed at the C2 level, and high signal change was found in the spinal cord on T2 weighted-images (Fig. 2C, D).
4. Surgical treatment
We performed C2ŌĆōC3 posterior decompression for C2 spondylolysis. C2 spondylolysis was recognized and proliferation of synovial membrane existed around the pars defect. We performed total laminectomy at the C2 and partial laminectomy at C3. Ragged edge existed at the ventral aspect of the pars defect and compressed the dura mater bilaterally. Complete decompression of the dura mater was achieved.
5. Postoperative course
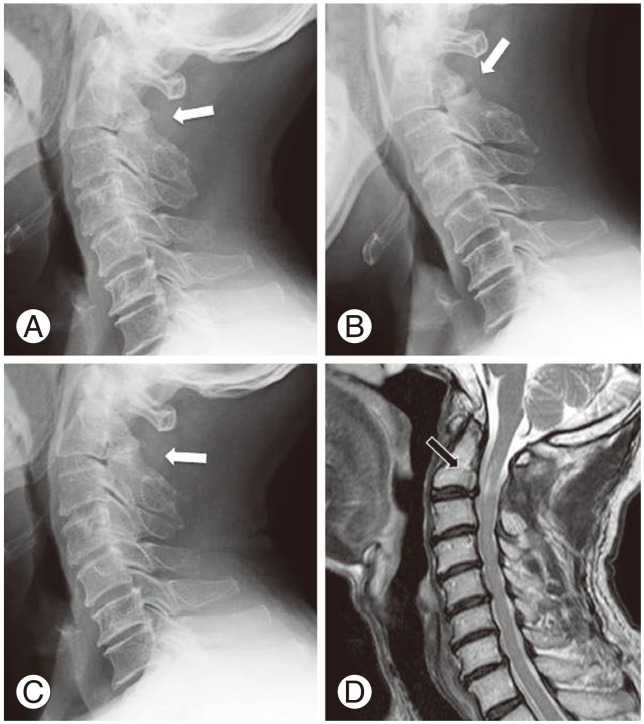
The postoperative course was uneventful. Clumsiness of both hands and difficulty in walking were alleviated. Plain radiography taken after one year postoperatively revealed no apparent instability (Fig. 3AŌĆōC). MRI scan two months postoperatively showed sufficient decompression of C2ŌĆōC3 (Fig. 3D).
Discussion
Spondylolysis commonly occurs in the lumbar spine and is present in around 6% of the population [34512]. However, cervical spondylolysis is exceedingly rare, and in regard to spondylolysis of C2, only 30 cases have been reported in the literature [16]. Gehweiler et al. [13] reported the first case of spondylolysis of C2 in 1977. Various symptoms of the cervical spondylolysis have been reported and include a clicking neck, neck pain, motion-associated pain, radiculopathy, and myelopathy that is sometimes diagnosed incidentally [214].
In the absence of specific symptoms, radiological findings are vital for making a correct diagnosis of cervical spondylolysis. In addition, the diagnosis should be distinguished from an acute fracture, such as a hangman's fracture. Previous reports outlined several points in this point. Nishimura et al. [1] proposed a differentiation based on CT involving a well-margined cleft or a sclerotic margin with a triangular configuration of the pillar fragments on either side of the spondylolytic defect, compensatory hyper- or hypoplasia of the ipsilateral articular pillars at the level above and/or below the defect, and the presence of associated dysplastic changes at the involved level. MRI is ineffective in delineating the bony architecture of the cervical spine, but is useful for assessment of the acuteness of the injury according to the presence of edema in the softtissue and bony structures, condition of the spinal cord, and presence of associated disc herniations around the involved segment [21516].
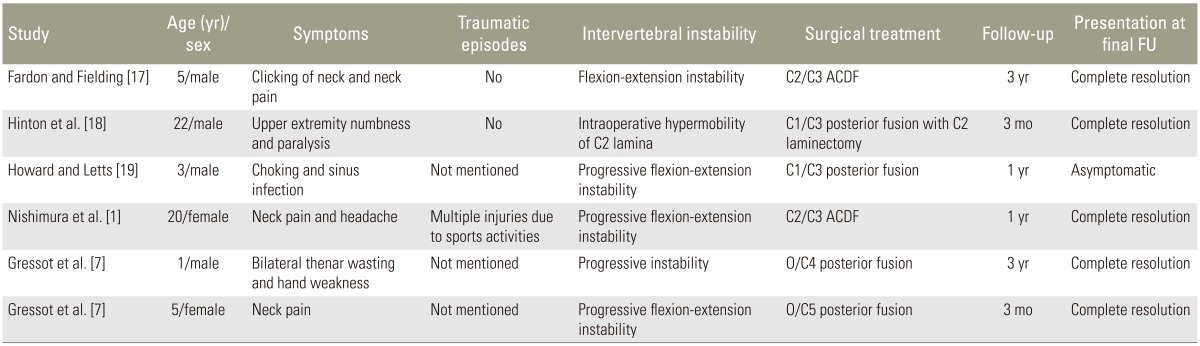
Basically, surgical treatment for the cervical spondylolysis is directed in cases with symptoms, instability, spinal cord compression, and neurologic deficit [16]. Among 30 patients with C2 spondylolysis who have been reported previously, only six underwent surgery. In addition, all of the patients required intervertebral fusion due to C2ŌĆōC3 instability. None of 21 patients without C2ŌĆōC3 instability required surgical treatment (Table 1) [171213171819].
In lumbar spondylolysis, once the pars defect is completed, two pathological entities are considered. The first is slippage and low-back pain. The second is pseudarthrosis of a fractured pars defect produces radiculopathy by compressing the nerve root [9101120]. Ragged edge around the pars defect is the most frequent contributing factor for radiculopathy and surgical treatment is sometimes required [11]. However, such an entity has not been reported in the cervical spine. In our case, it was considered as the proliferative changes due to the mobility around the pars defects, which is a mechanism similar to pseudoarthrosis of the long bone. We believe this is the first case with myelopathy due to the ragged edge at the ventral aspect of bilateral pars defects, not due to C2ŌĆōC3 intervertebral instability.