 |
 |
- Search
| Asian Spine J > Volume 15(6); 2021 > Article |
|
Abstract
Purpose
Inflammatory cytokines produced at the site of disc herniation are considered as pain generators in patients with lumbar disc disease. Whether a high-sensitivity C-reactive protein (hs-CRP) assay can be used in order to predict the quantum of inflammation surrounding nerve roots is a matter of investigation. This study aimed to evaluate the association of hs-CRP level and functional outcomes measured by the Modified Oswestry Low Back Pain Disability Questionnaire (MODY) before and after epidural steroid injection (ESI) in patients with lumbar disc disease.
Overview of Literature
Although many studies examining the role of hs-CRP levels and lumbar pain have been published previously, the results are equivocal, and there is no clear consensus regarding which patients will benefit from an ESI.
Methods
This was a prospective study, with 77 patients in the study group and 23 participants in the control group. Baseline hs-CRP levels were obtained for both groups. Study group patients received a single ESI and were subjected to detailed pre- and post-procedure evaluation using MODY scores. For this group, hs-CRP levels were measured at 1 and 2 months after injection.
Results
Out of 77 patients, 52 had acute and 25 had chronic low back pain. Thirty-six patients with acute pain obtained significant improvement, while 16 had an insignificant response to the ESI. None of the chronic cases had a significant response. The mean baseline hs-CRP (mg/L) among the study group (29.83±10.43) was significantly higher than for the controls (10.26±2.783). The baseline hs-CRP among acute cases, where post ESI MODY score at 2 months had significant reduction, was 32.19±5.126, and those with insignificant reduction was 18.13±7.949 (p<0.001).
Low back pain (LBP) is a common health problem, and is a major cause of disability affecting work performance and general well-being of an individual. The 2017 Global Burden of Disease Study estimated that LBP remained in the top list of global all age years lived with disability [1]. LBP is experienced by 60%–80% of adults at some point in their lifetime. The prevalence of LBP among young adults in India has been reported to be nearly 42% [2]. Patients with LBP due to structural damage of a disc have been reported to exhibit higher circulating levels of several inflammatory factors [3]. Radicular pain from a herniated disc may result from inflammation surrounding the nerve roots or from compression of nerve roots by the disc herniation. Generally, both components co-exist, with one being predominant. Underlying inflammation in LBP can lead to an increase in C-reactive protein (CRP) levels [4,5]. Treatment options for LBP primarily are analgesics and physiotherapy. Non-responders may be offered epidural steroid injections (ESIs). Steroids, if injected locally, can reduce the production of inflammatory molecules, and thus, can theoretically reduce inflammation around the disc, providing pain relief. Additionally, it has been suggested that steroids may inhibit pain by suppressing ectopic discharges from injured nerve fibers, and by depressing conduction in normal unmyelinated type C fibers [6].
Previous studies aiming to predict the risk of coronary and cerebrovascular disease in an apparently healthy population, much before their occurrence found an elevated level of CRP in the susceptible group [7,8]. The high-sensitivity C-reactive protein (hs-CRP) has been used by obstetricians to predict the outcome of pregnancies complicated by pre-eclampsia [9]. The traditional methods of CRP measurement are capable of measuring CRP in the ranges of 3–5 mg/L, which is useful for infections, but not if there is only a minute increase. The ultrasensitive hs-CRP enzyme-linked immunosorbent assay (ELISA) assay measures the CRP levels in the range of 0.007 mg/L [10]. Inflammatory response in LBP patients in terms of hs-CRP levels has been studied only sparingly.
This research paper was designed to study the pre and post ESI hs-CRP levels in LBP patients. Additionally, the clinical relevance of hs-CRP in LBP patients with radiculopathy is also examined, aiming to identify if it can be used as a marker for the extent of inflammation, and thus as a probable tool to predict the outcomes following ESIs in appropriately selected patients. The basic research question was to evaluate the efficacy of hs-CRP as a marker of inflammation and a predictor of ESI outcomes in LBP patients.
This prospective cohort study included patients presenting to the LBP clinic of a tertiary care center (Post Graduate Institute of Medical Education and Research [PGIMER], Chandigarh, India) over a 1-year period. Institutional ethics committee clearance from PGIMER, Chandigarh (approval no., NK/1627/MS) was obtained. Patients between 20 and 50 years of either gender, who were diagnosed with lumbar disc disease with radiculopathy, and who were consenting to participate were included (study group). These patients had no symptomatic relief after an initial course of physiotherapy and analgesics (minimum 6 weeks), and all complained of pain that interfered with their activities of daily living. Magnetic resonance imaging confirmation of lumbar disc herniation was ensured, and co-related with our clinical findings. Patients suffering from chronic inflammatory diseases, malignancy, uncontrolled diabetes mellitus; having any local and/or systemic source of infection; chronic smokers; morbidly obese patients (body mass index more than or equal to 30 kg/m2) and patients with ischemic heart disease and stroke were excluded. The control group consisted of normal subjects, with no co-morbidities, who had visited the hospital along with a family member. They were matched to the study group in terms of gender and age. Written consent for participation was obtained from all participants. All patients in the study group were evaluated for any systemic or local infection at the injection site, any allergic reaction to contrast agent, lignocaine, or methylprednisolone acetate injection. A coagulation profile and HbA1c levels were obtained prior to the procedure.
Venous blood (3 mL) was collected from the antecubital vein of all participants for hs-CRP measurement, by using a quantitative CRP solid-phase ultrasensitive immunoassay (CRP Ultra EIA; Xema Co. Ltd., Moscow, Russia). The results of these tests were interpreted after deriving optical density (OD) value using the ELISA reader for each sample. A quantitative value of hs-CRP in each sample was derived by using a calibration curve plotted for OD value versus CRP concentration, as per manufacturer’s instruction.
All injections were administered in the operating room by a senior anesthetist, who regularly practiced epidural injections, with the patient in the prone position on a radiolucent table. The interlaminar space between two contiguous vertebrae was identified (the level where injection was planned) on fluoroscopy images. Lignocaine skin infiltration (2%) was completed, and an 18G Tuohy’s epidural needle was inserted using a standard medial approach and loss of resistance technique. Fluoroscopic images were obtained to confirm the needle position and 0.5–1 mL of Iohexol (Omnipaque 300; GE Healthcare, Piscataway, NJ, USA) was injected to confirm the appropriate placement of needle near the desired nerve root (Fig. 1). Following this, 2 mL of methyl prednisolone acetate (80 mg) was injected, without any local anesthetic.
All injections were performed as day care procedures, and the patients were discharged with Paracetamol 500 mg tablets to be taken thrice daily for 5 days. Aceclofenac (100 mg) was prescribed, to be taken only for breakthrough pain. The patients were warned about feelings of numbness or temporary weakness, and were advised to resume routine activities and back strengthening exercises from the next day and onwards. hs-CRP levels were measured 1 month and 2 months after the procedure. Modified Oswestry Low Back Pain Disability Questionnaire (MODY) scores were calculated before, after 1 month, and after 2 months of the procedure. Data was collected in a pre-designed format, and analyzed using the SPSS for Windows ver. 17.0 (SPSS Inc., Chicago, IL, USA). A Shapiro–Wilk test was performed, and normal-quantile (Q-Q) plots were constructed to determine the normality of data. A Student t-test was used for comparison of mean hs-CRP levels. Repeated measures analysis of variance were used to study the trends of hs-CRP and MODY scores in acute and chronic cases. For comparison of proportions, a chi-square test was used. A p-value of <0.05 was taken as significant.
Of the 160 patients screened, 84 patients received a lumbar ESI. Seven patients were excluded from assessment (Fig. 2). Final assessment was done on 77 patients in our study, and 23 patients from the control group. The mean age was 34.14 years and 30.13 years for the study and control groups, respectively. In the study group, 52 patients had acute (<3 months) and 25 had chronic LBP (>3 months). Fifty-six patients had a single level disc disease whereas, 21 had multiple level disc disease.
The baseline hs-CRP level was significantly higher in the study group as compared to the control group. Patients with chronic LBP had a higher baseline hs-CRP when compared to acute cases (p=0.016). The mean of baseline hs-CRP among cases with a single level disc disease was 28.65±9.59, and among cases with multiple level disc disease, was 32.15±11.7; there was no statistically significant difference in hs-CRP level (p=0.164) for patients with single level versus multiple level disc disease (Table 1).
Difference in reduction of MODY score by >10 or 10 points at 2 months post ESI, when compared with the pre-procedural score, was taken considered as a significant reduction. The MODY score was found to have significantly improved in 36 patients of the acute LBP study group; 16 patients with acute LBP had no significant improvement (Table 2). While the patients with chronic LBP had improvement in their MODY score, none of them had a significant reduction of the score. Significant reduction of MODY score was seen in those acute LBP patients who had higher baseline hs-CRP levels when compared to those with relatively lower baseline hs-CRP levels (Fig. 3). Analysis of the trends of hs-CRP change within the study group showed that patients who had a significant reduction of MODY score had higher baseline hs-CRP level, and had a rapid reduction. Also, in patients with chronic LBP, the rate of reduction in the hs-CRP level was slower; this reduction was not statistically significant. Even though the baseline hs-CRP level was higher in patients with chronic LBP in comparison to the acute LBP cases, the rate of fall in hs-CRP level was faster in the acute patients (blue line) (Fig. 4). The hs-CRP level remained almost the same in chronic LBP patients even after an ESI. No major complications were encountered following epidural injection, except in one case, where transient flushing developed and later settled on its own.
LBP causes significant morbidity and disability. The commonest cause of LBP in young adults is a prolapsed intervertebral disc (PIVD), resulting from a rupture of annular fibers and the consequent displacement of nucleus pulposus. The periphery of the disc possesses nociceptive innervation; pain may be produced by mechanical or degenerative pressure on the outer annular fibers. PIVD can also cause nerve root compression. Local inflammation around the protruded disc leads to an inflammatory response, and a consequent increase in inflammatory markers. Treatment in the form of analgesics and exercise-based physical therapy is recommended during the initial weeks of management, in the absence of severe neurological deficits [11]. In case of inadequate response, patients can be offered a lumbar ESI, but an equivocal response obtained in many patients is a reason for dissatisfaction both among patients and clinicians. This is primarily because, while most LBP has an inflammatory component, some episodes may comprise a mechanical component as well. Recent studies have focused on the use of serum inflammatory markers, such as hs-CRP, interleukin (IL)-6, tumor necrosis factor-α, IL-8, IL-1β, IL-21, and IL-17 as potential biomarkers of LBP due to disc herniation [12]. Pedersen et al. [13] co-related the serum concentration of IL-6 and IL-8 with pain intensity (using Visual Analog Scale [VAS]) in patients with chronic lumbar radicular pain due to disc herniation. Cheng et al. [14] found that T helper 17 lymphocyte levels were higher in patients with ruptured versus non-ruptured lumbar discs.
The use of epidural steroids for radicular and LBP was first reported by Lievre et al. [15]. Heyse-Moore [16] showed a 62% success rate and Watts and Silagy [17] achieved 75%–95% relief in their series of patients with LBP. In our study, 72 out of 77 patients, those with either acute or chronic LBP, obtained improvement in terms of MODY scores at 2 months, thus showing an efficacy of 93%. Previous studies examining the role of hs-CRP levels and lumbar LBP which have been published are summarized in Table 3 [18–26].
Our study utilized methylprednisolone, a particulate steroid possessing a longer duration of action, due to a local depot effect as compared to nonparticulate steroids like dexamethasone, which has a rapid clearance and a short duration of action [27]. Although, the current trend favors a transforaminal approach, there is not much evidence to support its superiority [28,29]. The interlaminar route ESIs are commonly practiced at our institute. The interlaminar route has been reported to be safe for delivery of methylprednisolone, and the possibility of adverse events with methylprednisolone via the interlaminar route is less than via the trans-foraminal route. If a transforaminal route is being used, then a nonparticulate steroid should preferably be used [30]. A single injection was used in this study instead of cumulative multiple injections; recent literature suggests that there is no evidence to favor a series of injections [31].
Sturmer et al. [18] concluded that mean pain intensity assessed by VAS was independently associated with high levels of hs-CRP in patients with acute sciatic pain, but not in those with chronic LBP. Thus, pain severity in patients with acute sciatic pain may be linked more to inflammatory changes than in patients with chronic LBP, where additional factors might also come into play. Gebhardt et al. [19] concluded that there was no difference in mean hs-CRP levels in acute versus chronic LBP patients, but the acute group displayed a decline in hs-CRP over 3 months, while remaining static in the chronic group.
The MODY score was used for measurement of outcomes in our study, as it is a more objective measure than VAS. We found that the chronic LBP patients had higher mean hs-CRP levels and these values did not reduce, even after ESI as in the acute group, thus reaffirming the findings of Gebhardt et al. [19]. Furthermore, limitations of previous studies included not having an appropriate control group, not considering factors such as obesity, smoking, or alcohol consumption, all of which are known to affect the hs-CRP levels. However, an appropriate control group was included in our study, and the confounding factors were kept to a minimum.
Studies by Sugimori et al. [20] and Le Gars et al. [21] found no significant difference in the hs-CRP levels in a single or multiple disc involved back pain. Our results also confirmed this. Sugimori et al. [20], Le Gars et al. [21], and Rathod et al. [22] have studied the relation between preoperative and postoperative hs-CRP levels in patients who underwent discectomy. Sugimori et al. [20] and Le Gars et al. [21] used Japanese Orthopaedic Association scoring, whereas Rathod et al. [22] used the MODY score for outcome analysis. Sugimori et al. [20] and Rathod et al. [22] used ultrasensitive latex assay for measuring hs-CRP levels, whereas Le Gars et al. [21] used the ELISA test.
All three studies showed that patients with high preoperative hs-CRP levels had insignificant improvement in postoperative pain scores. The probable reason for this finding is that a high hs-CRP indicates a primary inflammatory component, which is not addressed by discectomy. In the current study, ELISA method for hs-CRP calculation was used. MODY score for outcome measurement demonstrated that all patients in the study group had a higher baseline hs-CRP as compared to the members of the control group. Patients with acute LBP who had an improvement on outcome parameters following also ESI, had a significant decline in hs-CRP levels. One can infer that the high hs-CRP levels are an indication of a predominantly inflammatory etiology of LBP. If LBP patients fail to respond to analgesics and physiotherapy, the hs-CRP level can be estimated, and then used as a tool to decide if these patients would benefit from ESI or not. Based on the outcomes of the present study, patients with acute LBP with high hs-CRP levels can be considered as good candidates for ESI, and they may be counseled as such before offering the injection. Patients with chronic LBP can also be offered an ESI, but with an explanation provided to the patient beforehand regarding the possibility of improvement.
The study was not without its limitations. Short-term follow-up of 2 months, non-recording of the final outcomes of patients (such as how many required surgery), non-randomization of cases and that the patients were allowed to take analgesics for breakthrough pain, which theoretically might alter the hs-CRP levels, are few notable limitations. Additionally, MRI was used to confirm the presence of a lumbar disc herniation, but we applied no specific classification system. No separate sub-group analysis was thus performed for evaluating the role of different types of disc conditions, and the hs-CRP levels. The strength of this study is having baseline hs-CRP levels from our control group for comparison, as well as the use of ESI performed by a senior anesthetist, who has been routinely performing such injections. A future study evaluating the association of hs-CRP level with different levels of MRI-inferred disc conditions, and the course of disease over a longer time frame, can be conducted to further explore this investigation modality.
Baseline hs-CRP levels are raised significantly in patients with LBP indicating a considerable inflammatory component. Baseline hs-CRP can be used as an indicator of severity and a prognosticator of efficacy in patients with acute LBP, who are refractory to physiotherapy and analgesics. It can assist in determining which patients will likely experience improvement in symptoms following an ESI, thus adding a tool to the armamentarium of spinal surgeons.
Conflict of Interest
Conflict of Interest
No potential conflict of interest relevant to this article was reported.
Notes
Author Contributions
Rajesh Gopireddy: concept and design of the study; Karthick Rangasamy: data acquisition and analysis, writing–original draft preparation; Vijay G. Goni: supervision and critical revision of manuscript; Pulak Vatsya: manuscript writing–review and editing; Prateek Behera: data analysis and critical revision of manuscript; Yatindra K. Batra: performing an ESI procedure; Chetana Vaishnavi: data acquisition and helps in measuring hs-CRP values from lab side; and all authors read and approved the final manuscript.
Fig. 1
Anteroposterior (A) and lateral (B) view of lumbar spine showing needle in epidural space. Contrast dye was used to ensure needle position in epidural space and near desired nerve root.
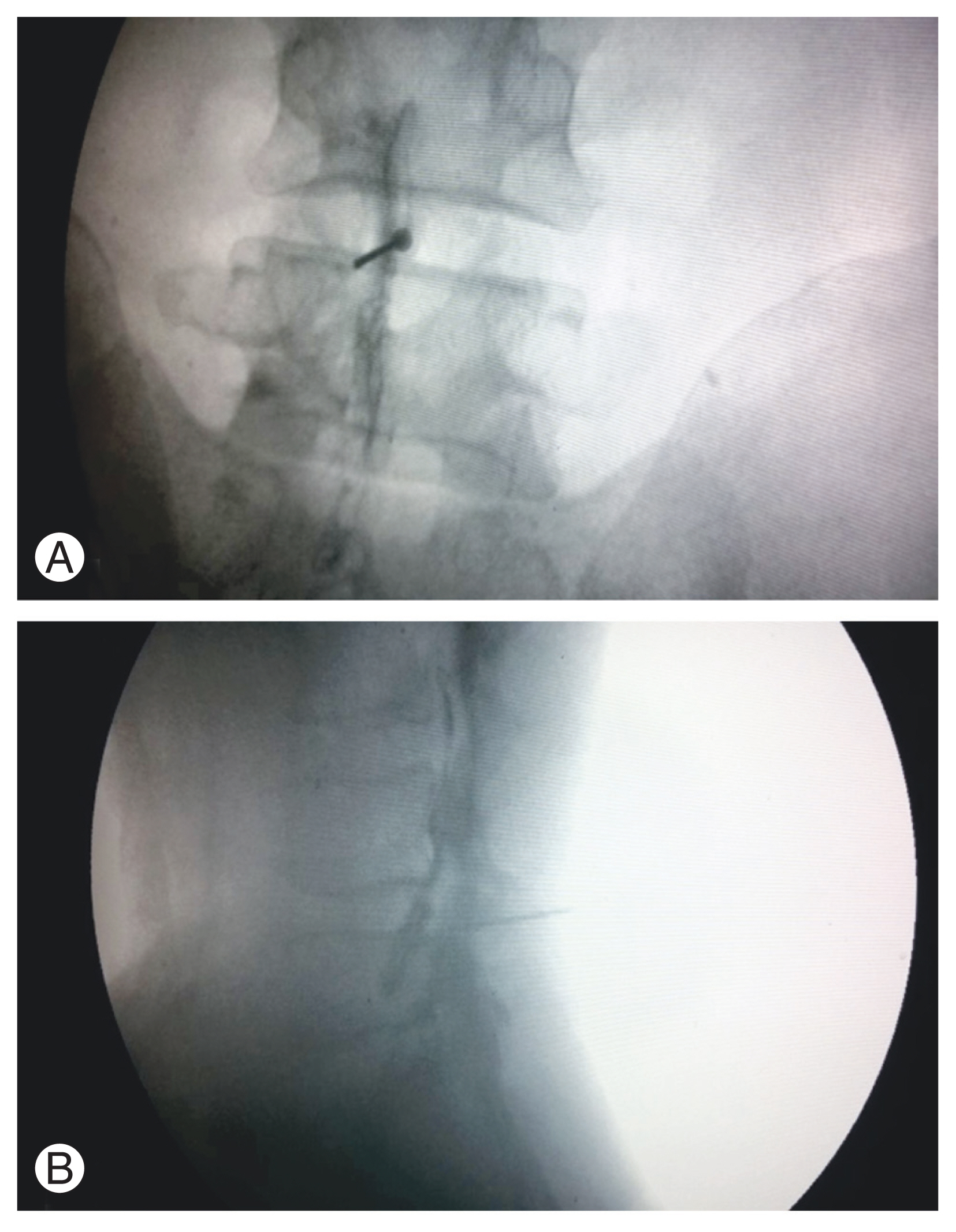
Fig. 2
Flow diagram illustrating the selection process of patients for epidural steroid injection and for final assessment. hs-CRP, high-sensitivity C-reactive protein; FU, follow-up; MODY, Modified Oswestry Low Back Pain Disability Questionnaire.
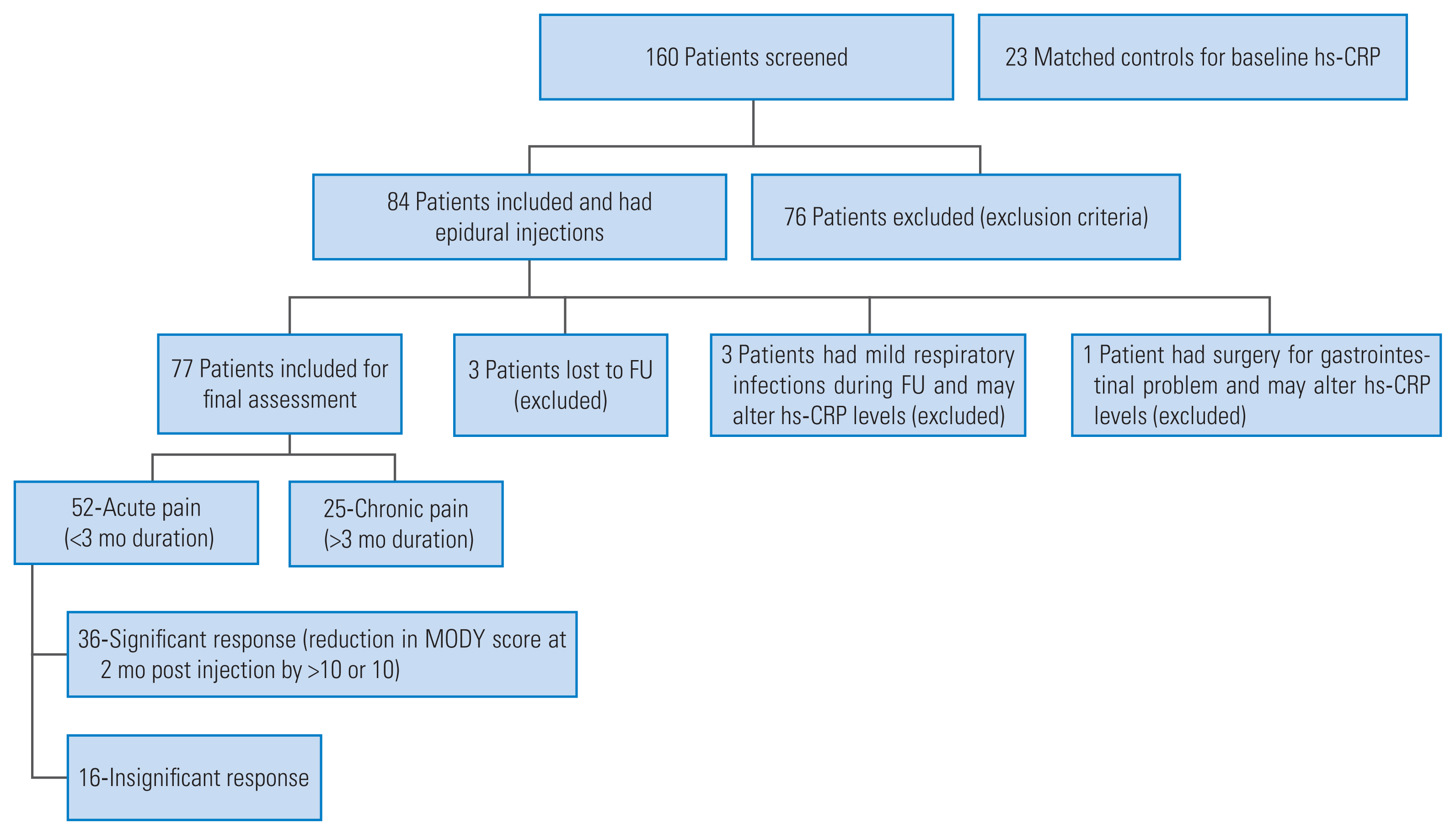
Fig. 3
Trend of hs-CRP levels in acute low back pain cases with significant and insignificant reduction of MODY scores. hs-CRP, high-sensitivity C-reactive protein; MODY, Modified Oswestry Low Back Pain Disability Questionnaire.
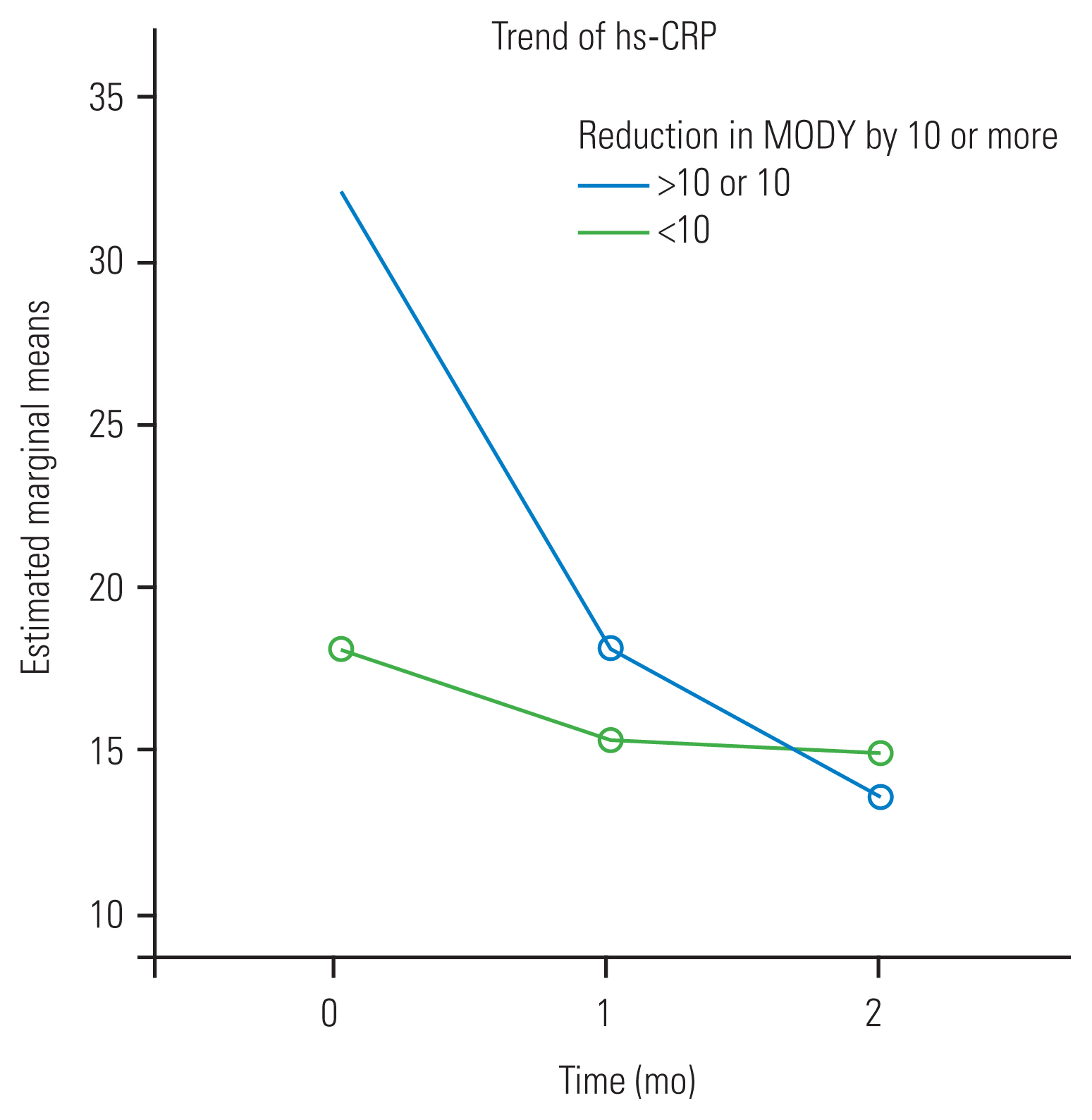
Fig. 4
Trend of hs-CRP in acute and chronic low back pain cases. hs-CRP, high-sensitivity C-reactive protein.
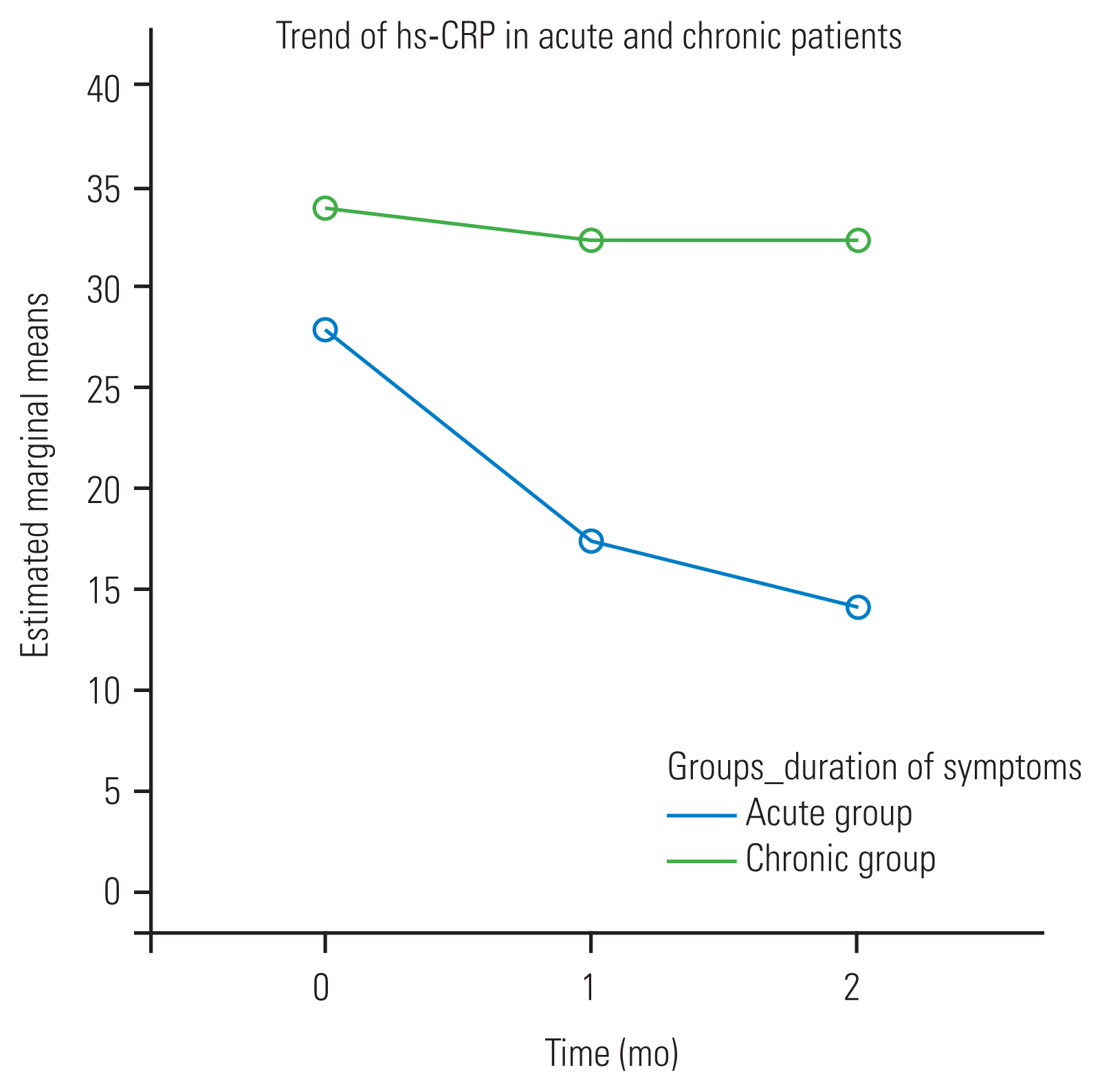
Table 1
Baseline hs-CRP levels in different groups
Table 2
Baseline hs-CRP in relation to MODY score in acute cases
| Reduction in MODY scorea) | Mean baseline hs-CRP level (mg/L) in acute cases |
|---|---|
| >10 or 10 | 32.19±5.126 |
| <10 | 18.13±7.949 |
| p-value | <0.001 |
Table 3
Table showing multiple studies showing relation of hs-CRP levels to lumbar disc disease
| Author | Level of evidence | Sample size | hs-CRP used as | Low back pain | ESI | Result/inference |
|---|---|---|---|---|---|---|
| Benny and Patel [23] (2014) | Systematic review | 50 Articles | Predictor of outcome | + | Used | No significant relation |
| Park and Lee [24] (201) | Case series | 55 | Predictor of VAS | + | Used | No correlation |
| Ackerman et al. [25] (2006) | Case-control | 60 | Predictor of outcome | + | Used | Negative correlation |
| Le Gars et al. [21] (2000) | Case-control | 70 | Predictor of symptoms | + | Used | Positive correlation |
| Gebhardt et al. [19] (2006) | Case series | 72 | Predictor of outcome | + | Used | Negative correlation |
| Sturmer et al. [18] (2005) | Prospective case series | 72 | Predictor of VAS | + | Used | Po_sitive with acute and negative with chronic symptoms |
| Rannou et al. [26] (2007) | Cohort | 36 | Relation to disc changes | + | No | Ra_ised in patients with Modic type 1 changes |
| Sugimori et al. [20] (2003) | Case-control | 48 | Predictor of outcomes | + | No | Positive correlation |
| Rathod et al. [22] (2014) | Case-control | 50 | Predictor of outcomes | + | No | Positive correlation |
References
1. GBD 2017 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 2018 392:1789–858.



2. Ganesan S, Acharya AS, Chauhan R, Acharya S. Prevalence and risk factors for low back pain in 1,355 young adults: a cross-sectional study. Asian Spine J 2017 11:610–7.




3. Zhang Y, Sun Z, Liu J, Guo X. Advances in susceptibility genetics of intervertebral degenerative disc disease. Int J Biol Sci 2008 4:283–90.



4. Kang JD, Georgescu HI, McIntyre-Larkin L, Stefanovic-Racic M, Donaldson WF 3rd, Evans CH. Herniated lumbar intervertebral discs spontaneously produce matrix metalloproteinases, nitric oxide, interleukin-6, and prostaglandin E2. Spine (Phila Pa 1976) 1996 21:271–7.


5. Mulleman D, Mammou S, Griffoul I, Watier H, Goupille P. Pathophysiology of disk-related sciatica: I. evidence supporting a chemical component. Joint Bone Spine 2006 73:151–8.


6. Johansson A, Hao J, Sjolund B. Local corticosteroid application blocks transmission in normal nociceptive C-fibres. Acta Anaesthesiol Scand 1990 34:335–8.


7. Ridker PM. High-sensitivity C-reactive protein: potential adjunct for global risk assessment in the primary prevention of cardiovascular disease. Circulation 2001 103:1813–8.


8. Ridker PM, Cushman M, Stampfer MJ, Tracy RP, Hennekens CH. Inflammation, aspirin, and the risk of cardiovascular disease in apparently healthy men. N Engl J Med 1997 336:973–9.


9. Mishra N, Pradhan K, Sahoo GD, Rohilla M, Meena M. Can hsCRP be the sole investigation for predicting the severity and outcome in women with pre‐eclampsia presenting late in pregnancy? Trop J Obstet Gynaecol 2019 36:54–60.

10. Rifai N, Tracy RP, Ridker PM. Clinical efficacy of an automated high-sensitivity C-reactive protein assay. Clin Chem 1999 45:2136–41.



11. Deyo RA, Mirza SK. Clinical practice: herniated lumbar intervertebral disk. N Engl J Med 2016 374:1763–72.


12. Khan AN, Jacobsen HE, Khan J, et al. Inflammatory biomarkers of low back pain and disc degeneration: a review. Ann N Y Acad Sci 2017 1410:68–84.



13. Pedersen LM, Schistad E, Jacobsen LM, Roe C, Gjerstad J. Serum levels of the pro-inflammatory interleukins 6 (IL-6) and -8 (IL-8) in patients with lumbar radicular pain due to disc herniation: a 12-month prospective study. Brain Behav Immun 2015 46:132–6.


14. Cheng L, Fan W, Liu B, Wang X, Nie L. Th17 lymphocyte levels are higher in patients with ruptured than non-ruptured lumbar discs, and are correlated with pain intensity. Injury 2013 44:1805–10.


15. Lievre JA, Bloch-Michel H, Pean G, Uro J. L’hydrocortisone en injection locale. Rev Rhum 1953 20:310–1.
16. Heyse-Moore GH. A rational approach to the use of epidural medication in the treatment of sciatic pain. Acta Orthop Scand 1978 49:366–70.


17. Watts RW, Silagy CA. A meta-analysis on the efficacy of epidural corticosteroids in the treatment of sciatica. Anaesth Intensive Care 1995 23:564–9.


18. Sturmer T, Raum E, Buchner M, et al. Pain and high sensitivity C reactive protein in patients with chronic low back pain and acute sciatic pain. Ann Rheum Dis 2005 64:921–5.



19. Gebhardt K, Brenner H, Sturmer T, et al. The course of high-sensitive C-reactive protein in correlation with pain and clinical function in patients with acute lumbosciatic pain and chronic low back pain: a 6 months prospective longitudinal study. Eur J Pain 2006 10:711–9.


20. Sugimori K, Kawaguchi Y, Morita M, Kitajima I, Kimura T. High-sensitivity analysis of serum C-reactive protein in young patients with lumbar disc herniation. J Bone Joint Surg Br 2003 85:1151–4.


21. Le Gars L, Borderie D, Kaplan G, Berenbaum F. Systemic inflammatory response with plasma C-reactive protein elevation in disk-related lumbosciatic syndrome. Joint Bone Spine 2000 67:452–5.

22. Rathod TN, Chandanwale A, Ladkat KM, Chavan S, Chavan A, Bhosale PB. High sensitive C-reactive protein: effective tool in determining postoperative recovery in lumbar disc disease. Indian J Orthop 2014 48:354–9.



23. Benny BV, Patel MY. Predicting epidural steroid injections with laboratory markers and imaging techniques. Spine J 2014 14:2500–8.


24. Park CH, Lee SH. Prognostic usefulness of high sensitivity C-reactive protein for transforaminal epidural steroid injection in patients with radicular pain. Pain Med 2011 12:219–23.



25. Ackerman WE 3rd, Zhang JM. Serum hs-CRP as a useful marker for predicting the efficacy of lumbar epidural steroid injections on pain relief in patients with lumbar disc herniations. J Ky Med Assoc 2006 104:295–9.

26. Rannou F, Ouanes W, Boutron I, et al. High-sensitivity C-reactive protein in chronic low back pain with vertebral end-plate Modic signal changes. Arthritis Rheum 2007 57:1311–5.


27. Benzon HT, Chew TL, McCarthy RJ, Benzon HA, Walega DR. Comparison of the particle sizes of different steroids and the effect of dilution: a review of the relative neurotoxicities of the steroids. Anesthesiology 2007 106:331–8.



28. American Academy of Pain Medicine. Transforaminal vs. interlaminar epidural steroid injections: both offered similar pain relief, function for radiating low-back pain. ScienceDaily [Internet] 2014 Mar 6 [cited 2020 Jun 8]. Available from: https://www.sciencedaily.com/releases/2014/03/140306211032.htm
29. Manchikanti L, Pampati V, Falco FJ, Hirsch JA. Growth of spinal interventional pain management techniques: analysis of utilization trends and Medicare expenditures 2000 to 2008. Spine (Phila Pa 1976) 2013 38:157–68.








