|
 |
- Search
| Asian Spine J > Volume 17(5); 2023 > Article |
|
Abstract
Posterior methods for cervical myelopathy include laminoplasty and laminectomy with/without fusion. A more recent innovation in these treatments is the use of an ultrasonic bone shaver for osteotomy. In this study, we examined the perioperative results after laminectomy/laminoplasty between conventional methods (rongeur/high-speed drill) vs. piezosurgery-based instruments. PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines were followed and the search was performed on four databases (PubMed, Scopus, EMBASE, and Google Scholar). Seven comparative studies were chosen after thorough screening by the authors and a meta-analysis was performed between piezosurgery and conventional technique to ascertain intraoperative and postoperative results after laminectomy/laminoplasty. The analysis includes four retrospective cohort studies and three randomized controlled trials published between 2015 and 2022. The mean age ranged from 55.5 to 64.2 years. Blood loss was significantly reduced in the piezosurgery group, other findings were not significant. On subgroup analysis, laminoplasty dramatically reduced blood loss and the rate of iatrogenic dural rips in the piezosurgery group. The use of ultrasonic bone shaver for osteotomy in cervical spondylotic myelopathy is related to significantly decreased blood loss and no significant increase in postoperative drainage, operative time, complication rate, and functional outcomes as compared to traditional techniques. We noticed significantly reduced blood and rate of dural tears in the laminoplasty subgroup with the use of ultrasonic bone shaver, which was not mirrored in the laminectomy subgroup. Careful intraoperative handling of the instrument can help prevent iatrogenic dural tears and nerve damage.
Cervical spondylotic myelopathy (CSM) is a common cause of disability in the elderly population with an underlying etiology that includes cervical spondylosis, ossified posterior longitudinal ligament (OPLL), and congenital cervical stenosis [1–3]. Karadimas et al. [4] in a systematic review discovered that 20%–60% of patients on conservative treatment would have neurological deterioration without surgical intervention. The Japanese Orthopaedic Association (JOA) score considerably improved in patients who underwent surgery, according to a meta-analysis by Feng et al. [5]. An individual patient-based surgical method is the suggested mode of treatment for cervical myelopathy [6–8]. Surgical approaches to the condition might be anterior, posterior, or combination. Posterior procedures for CSM include laminectomy with or without fusion and laminoplasty. Some indications of posterior procedures include multilevel disease, and primarily posterior pathology such as OPLL [6]. During these procedures, osteotomy is typically performed using bone rongeurs, bone punches, and high-speed drilling [9,10]. These are related to complications such as thermal injury, and soft tissue entanglement, and can be challenging to control and time-consuming [11,12]. The use of ultrasonic bone scalpels (UBS) for oral and maxillofacial surgery and skull base surgery has been well established [13–15]; this instrument is now being commonly employed in spine surgeries as well [12,16,17]. The theoretical benefits of UBS include greater precision, lesser soft tissue damage, lower blood loss, and reduced operating time [16,17].
The use of UBS in posterior cervical methods is a relatively new development and very few comparative studies are published on this subject. We performed this review and meta-analysis to analyze the intraoperative findings and postoperative result among osteotomies performed using conventional methods and the UBS.
The literature search was carried out on 20th June 2022. It was conducted on four databases—PubMed, Scopus, EMBASE, and Google Scholar, and PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines were followed [18]. The search was conducted using the keywords “Cervical AND Myelopathy AND Ultrasonic OR Piezosurgery.” To locate further material, a secondary search of the shortlisted papers’ references using the same criteria was conducted.
Initial screening of search results was performed to exclude duplicate studies. Non-English literature, case reports, conference abstracts, cadaveric and animal studies, non-comparative studies, and reviews were excluded. Studies in which a comparison between conventional methods (bone rongeur/high-speed drilling) and UBS/piezosurgery instruments for cervical osteotomy via posterior approach were done were included in our analysis. The meta-analysis omitted publications on surgical technique, anterior approaches for CSM, and publications that included all spinal procedures with no distinct results.
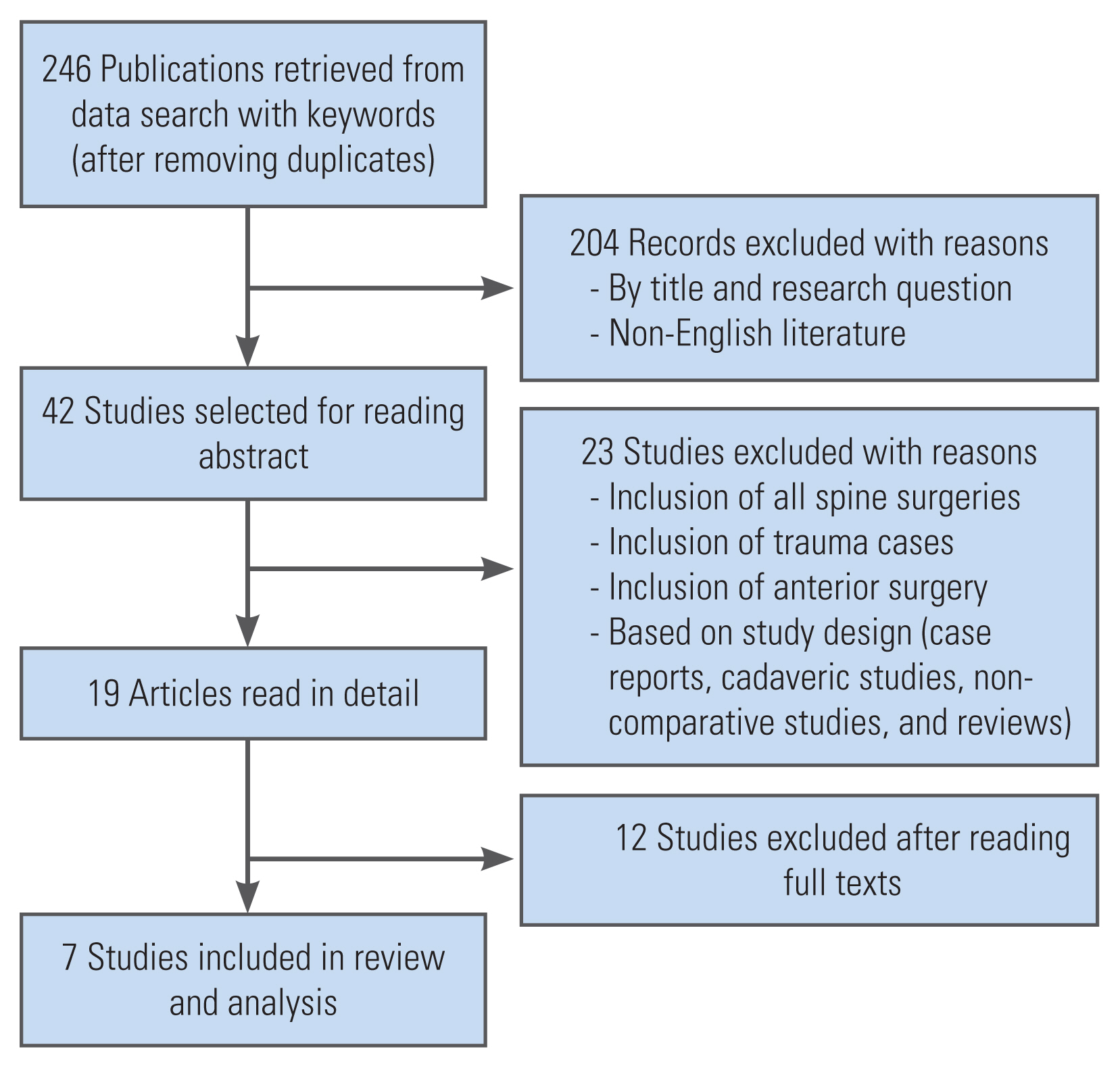
To ascertain the relevance of search results for our analysis, two authors (P.B. and V.K.) performed a screening of all results. Any conflicts between the two were resolved with input and analysis from the remaining co-authors. In our review for meta-analysis, studies that were deemed pertinent to our research topic and having an appropriate study design were included (Fig. 1).
The studies which were chosen for review were thoroughly read and all data from these studies were extracted and entered into a structured format. Table 1 provides an overview of the study’s year of publication, design, pathology it examined, surgical technique, and study groups. Table 2 summarizes the mean age, gender distribution, and the reported intraoperative and postoperative findings. Various studies had given various labels for their study groups but for convenience, we have labeled patients who received osteotomy with UBS/piezosurgery instruments as the piezosurgery group and patients in whom high-speed drill or rongeur was used as the conventional group.
After duplicates were eliminated, 246 articles were assessed. Based on preliminary screening based on title, study design, and language we were left with 42 publications for further evaluation. Following the reading of the abstracts for these, 19 further papers were chosen for a more thorough evaluation. Seven comparative studies published between the years 2015 and 2022 were then included in our final review and meta-analysis [19–25].
Comparative analysis between the piezosurgery group (experimental) and conventional group (control) was performed using Review Manager (RevMan) ver. 5.4 software (The Cochrane Collaboration, London, UK). Comparison of operating time, blood loss, and postoperative drainage were compared using inverse variance weighted meta-analysis. Using Mantel-Haenszel analysis, odds ratios (OR) were generated to compare the frequency of dural tears and postoperative C5 palsy.
Methodological index for non-randomized studies (MINORS) was used to evaluate the risk of bias in included studies [26].
All publications included in the review were comparative studies. Of the seven studies included in our review, four were retrospective cohort studies (level 3 evidence) [19,23–25] and the remaining three were prospective randomized controlled trials (RCT) (level 1/2 evidence) [20–22]. A total of 755 individuals were involved in this research, 355 of whom underwent piezosurgery and 400 of whom underwent conventional osteotomy. The primary pathologies included were CSM, OPLL, and cervical stenosis (Table 1).
Li et al. [20] reported a minimum mean age of 55.5 years for the piezosurgery group, while Sun et al. [24] reported a mean age of 64.2 years. The minimum mean age of patients in the conventional group was 57.6 years [20] and the maximum was 63.4 years [24]. Male predominance was observed in the patient groups with both the piezosurgery group and traditional group having 3–4 times males as compared to females (Table 2).
Onen et al. [19] carried out cervical laminectomy in their study cohort. While using UBS the whole thickness of the bone was cut till the softness of the dura was felt. Similar steps were taken by Dave et al. [23], who used UBS to cut the entire thickness of the bone. In cases with severe canal compromise, they left the inner cortex intact and completed the osteotomy with the help of a thin osteotome. Both authors have emphasized the importance of not applying any undue pressure to the instrument. Laminoplasty was the method performed by the other five authors in our review. Using a spatula blade, Huan et al. [22] finished the osteotomy in with additional osteotomies up to the inner cortex. A dome-like laminoplasty was conducted by Sun et al. [24], which included single open-door laminoplasty from C3 downwards, along with a C2 dome laminectomy.
All seven studies were included in the comparative analysis. According to statistical analysis, the piezosurgery group experienced significantly less blood loss than the control group, with a mean difference (MD) of 84.4 mL (95% confidence interval [CI], 9.6 to 159.3; p=0.03). The amount of postoperative drainage (MD, 31.8 mL; 95% CI, −9.6 to 73.1; p=0.13) and operative time (MD, 6.5 minutes; 95% CI, −3.7 to 16.8; p=0.21) were also lower in the piezosurgery group, but this did not reach statistical significance. A similar insignificant difference was observed in the rate of dural tears (OR, 0.55; 95% CI, 0.26 to 1.17; p=0.12) and postoperative C5 palsy (OR, 0.67; 95% CI, 0.24 to 1.89; p=0.45). Although percentage increases in JOA scores could not be statistically tested, none of the studies that reported this variable revealed a significant difference between the two groups [19–22,24,25] (Fig. 2A–E).
Subgroup analysis could be conducted for two parameters—blood loss and rate of dural tears. We analyzed for differences based on procedure—laminectomy/laminoplasty. Significantly reduced blood loss and lower risk of dural tears were observed in the piezosurgery groups when laminoplasty was performed (p<0.05). The same significance was not seen in laminectomy procedures in the research by Onen et al. [19] and Dave et al. [23] (Fig. 3A, B).
MINORS scoring was done for studies included in the review [26]. All of the included studies were rated out of 24 points because they were all comparative. Most of the included studies had a moderate risk of bias, with two of the prospective RCTs performed by Li et al. [20] and Kim et al. [21] respectively having a low risk of bias (Table 3).
This meta-analysis was performed to compare the perioperative results after spinal osteotomies (laminectomy/laminoplasty) for CSM using piezosurgery instruments and conventional methods (high-speed drill/rongeur). We discovered that there was a considerable variation in the amount of blood lost during surgery between the two osteotomy procedures. Further, we discovered that this difference along with a decreased rate of intraoperative dural tears with piezosurgery was significantly greater in the laminoplasty group compared to the laminectomy group.
The mean age reported in the study cohorts ranged from 55.5 to 64.2 years, with a male preponderance of subjects. There are very small number of research on the epidemiology of CSM, but the majority of published literature emphasizes an increased incidence with increasing age and greater frequency among males, which is consistent with the results of our review [2,27,28].
Early reports on the use of ultrasonic bone curettes highlighted the usefulness of this instrument in spinal surgery at all vertebral levels [17,27,28]. The lightweight design, lack of operational field obstruction, and capability to utilize the shaver on the inner cortex without worrying about damaging the dura and epidural venous plexus were all highlighted as advantages of the single-handed operation. In addition, due to the absence of any spinning components, there was no fear of entanglements of cotton pieces and no significant heat generation locally. Initial studies indicated little to no intraoperative dural tears with the use of UBS, but subsequent research has demonstrated that they have a similar safety profile to traditional osteotomy techniques [16]. Hazer et al. [29] in a study on the technical aspects and safety profile of UBS in spine surgery speculated that the constant application of the shaver to a single point could be the cause of the iatrogenic dural tears with its use. They suggested lowering the energy output of the device and preventing use at a single point over 10 seconds. Dural injury with the use of UBS is reported in cases of severe canal compromise, and the application of suction from the tip of the instrument on the dura [27]. Although early studies revealed that the use of UBS reduced the incidence of dural tears and postoperative nerve root injury [12,27], these results have not been replicated and supported by more current research [16]. Our analysis also showed no considerable difference in the rate of dural tears and postoperative C5 palsy between the two groups.
On statistical comparison, the amount of blood loss significantly favored the use of piezosurgery instruments for osteotomy with a MD of 84.4 mL (95% CI, 9.6–159.3). The literature concerning this finding is mostly consistent with five out of seven studies in our cohort reporting significantly decreased blood loss in the piezosurgery group. Similar findings have been reported in other trials on the effects of using UBS in cervical, thoracic, and lumbar procedures, with much more blood loss in the traditional groups [17,29–32]. The possible reasons for decreased blood loss with the use of piezosurgery include lower trauma to the surrounding soft tissue due to tissue selectivity, heat generation during usage which results in micro vascular coagulation, and an air-water cavitation effect that closes the small blood vessels [20,25,33]. Although the meta-analysis showed a similar tendency of less postoperative drainage, this was not statistically significant. Findings of lower postoperative drainage have been reported in the literature before [34] and were statistically significant in the evaluation by Li et al. [20] but no other articles from our analysis revealed significance.
The literature with regards to operative time with the use of UBS is conflicting with reports ranging from decreased operative time with UBS to those significantly favoring the conventional techniques [30–32,35], Although this was not statistically significant, Li et al. [20] and Lin et al. [25] reported shorter surgical times using conventional procedures in our population. Wahlquist et al. [32] attributed the quicker surgical time to the decreased blood loss leading to improved operative field visualization and less time spent on obtaining hemostasis. Simultaneously, the surgeon’s inexperience with the instrument and the need for prolonged application of the shaver to the bone might be the reason for the increased operative time. Although a combination of these factors along with individual patient-related factors may be at play, our meta-analysis indicates that there is no significant difference in the operating time with the use of these two procedures.
A unique finding which we noticed in the subgroup analysis was the significantly decreased blood and rate of dural tears in the laminoplasty subgroup with the use of UBS, which was not mirrored in the laminectomy subgroup. This seems to imply that the use of UBS has a more significant benefit when doing laminoplasty; however, we were unable to determine the basis for this conclusion. It could be because of just two studies in the laminectomy subgroup, which necessitates the need for further prospective studies to ascertain whether this finding is reproduced or not.
Very few comparative studies have been published to examine the use of piezosurgery and conventional methods for posterior cervical procedures for CSM. Additionally, our meta-analysis has limitations due to the variability of study designs, operating procedures, and surgical techniques. Despite these limitations, the studies included in our review had a moderate to low risk of bias, and analysis showed valuable findings which can help in decision-making for spine surgeons with regard to the use of UBS. This analysis should form the basis of potential future research in the form of prospective RCTs to confirm these initial findings.
According to our meta-analysis, we ascertained that the use of UBS for osteotomy in CSM is related with significantly reduced blood loss and no significant increase in operative time as compared to traditional methods. Along with the ease of handling of the instrument, these results make UBS a viable alternative for osteotomies in the cervical spine. Simultaneously, it is essential to be well-versed in the use of this instrument to prevent iatrogenic dural tears and other complications.
Notes
Author Contributions
PB assisted in conducting the literature search, performed the statistical analysis, and drafted the initial version of the article. VK contributed to the study’s conceptualization, edited the drafts, and provided final approval. AJV participated in conceptualizing the review, conducting the literature search, and editing the drafts. AG aided in the literature search and contributed to drafting the initial version of the article. SSD contributed to the study’s conceptualization, edited the drafts, and provided final approval.
Fig. 2
Comparative analysis between piezosurgery (experimental) and conventional (control) groups. (A) On the basis of mean operative time. (B) On the basis of estimated blood loss. (C) On the basis of postoperative drainage. (D) On the basis of rate of dural tears. (E) On the basis of postoperative C5 palsy. SD, standard deviation; IV, inverse variance; CI, confidence interval; df, degrees of freedom; M–H, Mantel-Haenszel.

Fig. 3
Subgroup analysis between laminoplasty and laminectomy. (A) On the basis of estimated blood loss. (B) On the basis of rate of dural tears. SD, standard deviation; IV, inverse variance; CI, confidence interval; df, degrees of freedom; M–H, Mantel-Haenszel.
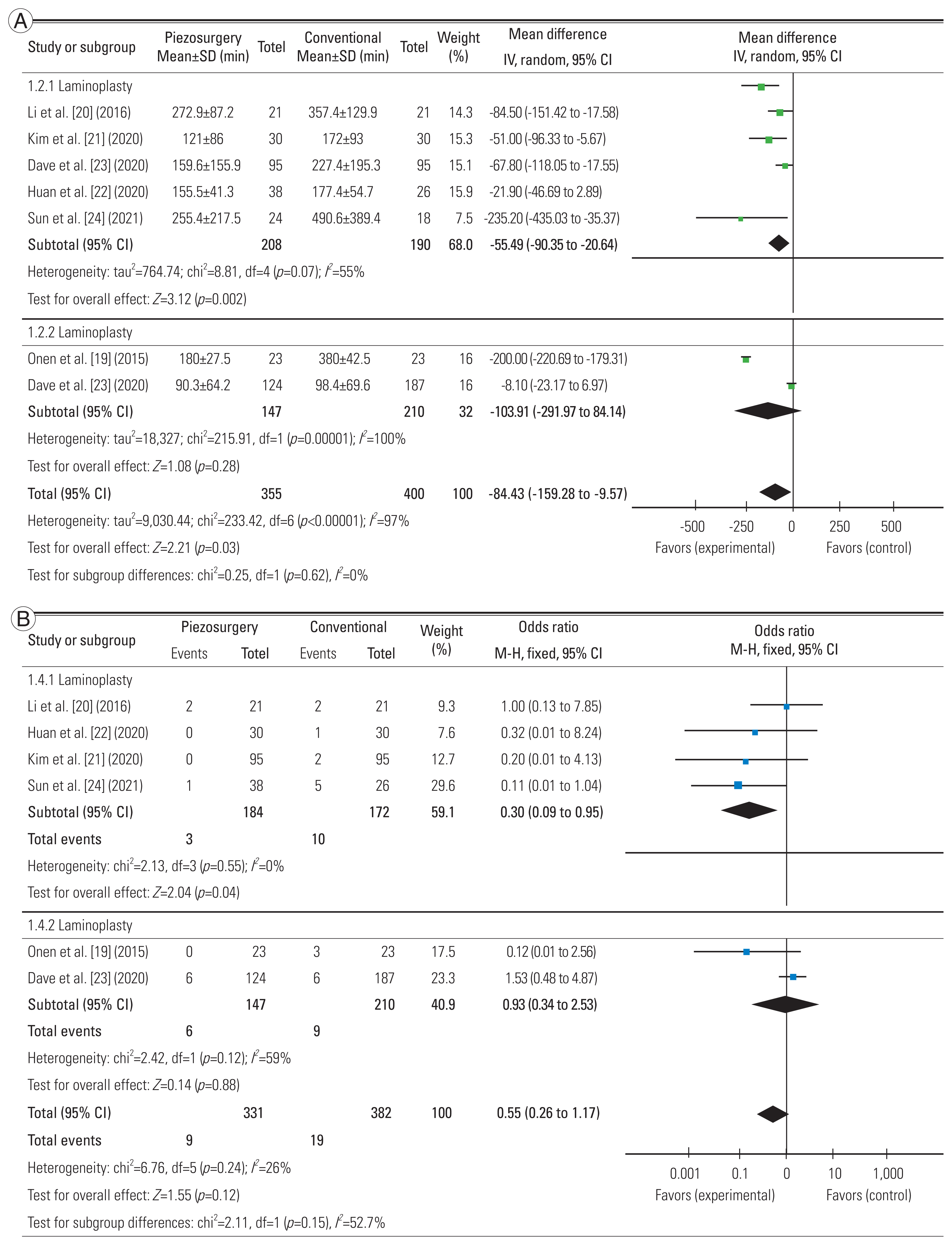
Table 1
Study characteristics of included studies (2015–2022)
| Study | Study design | Pathology | Procedure | Study groups |
|---|---|---|---|---|
| Onen et al. [19] (2015) | Retrospective cohort | CSM | Laminectomy+lateral mass screw fixation | UBS group (23), HSD group (23) |
| Li et al. [20] (2016) | Prospective RCT | CSM, OPLL, cervical stenosis | Expansive open door laminoplasty with titanium cage fixation | Piezosurgery group (21), drill group (21) |
| Kim et al. [21] (2020) | Prospective RCT | CSM, OPLL, cervical stenosis | Open door laminoplasty | UBS group (95), drill group (95) |
| Huan et al. [22] (2020) [22] | Prospective RCT | CSM | Posterior cervical expansive laminoplasty with a titanium plate | Piezosurgery group (30), high speed drill group (30) |
| Dave et al. [23] (2020) | Retrospective cohort | CSM, OPLL | Cervical laminectomy | UBS group (124), conventional methods (187) |
| Sun et al. [24] (2021) | Retrospective cohort | C2 involved OPLL | C2 dome like laminoplasty | UBC group (38), HSD group (26) |
| Lin et al. [25] (2022) | Retrospective cohort | CSM | Expansive open door laminoplasty | UBS group (24), HSD group (18) |
Table 2
Summary of reported outcomes
| Author | Study group | No. | Age (yr) | M:F | JOA score improvement (%) | Operation time (min) | Blood loss (mL) | Postop drainage (mL) | Complications | Miscellaneous |
|---|---|---|---|---|---|---|---|---|---|---|
| Onen et al. [19] (2015) | Piezosurgery group | 23 | 61 (41–87) | 18:5 | 47.6 | - | 180 (140–250) | - | Dural tear (0), C5 palsy (1) | Length of stay (3.0±0.0), duration of laminectomy (2.2±0.4 min/level) |
| Conventional group | 23 | 62.4 (49–74) | 16:7 | 48.8 | - | 124 | - | Dural tear (3), C5 palsy (1) | Length of stay (3.7±1.3), duration of laminectomy (7.9±2.6 min/level) | |
| Li et al. [20] (2016) | Piezosurgery group | 21 | 55.5±9.7 | 15:6 | 54.3 | 138.2±26.6 | 272.9±87.2 | 127.9±28.6 | Dural tear (2), C5 palsy (2) | Preop VAS (6.2±1.4), postop VAS (2.2±0.8) |
| Conventional group | 21 | 57.6±11.0 | 16:5 | 61.1 | 125.8±23.5 | 357.4±129.9 | 153.2±29.5 | Dural tear (2), C5 palsy (1) | Preop VAS (6.4±1.3), postop VAS (2.2±0.8) | |
| Kim et al. [21] (2020) | Piezosurgery group | 95 | 59.1±12.1 | 65:30 | - | 70 (30–240) | 159.6±155.9 | 153.3±76.6 | Dural tear (0), C5 palsy (0) | Patients with intraop lamina fracture (23) |
| Conventional group | 95 | 58.0±12.1 | 63:32 | - | 70 (40–195) | 227.4±195.3 | 139.5±53.2 | Dural tear (2), C5 palsy (0) | Patients with intraop lamina fracture (25) | |
| Huan et al. [22] (2020) | Piezosurgery group | 30 | 61±9 | 18:12 | - | 87±22 | 121±86 | 155±87 | Dural tear (0) | - |
| Conventional group | 30 | 59±11 | 16:14 | - | 96±35 | 172±93 | 246±95 | Dural tear (1) | - | |
| Dave et al. [23] (2020) | Piezosurgery group | 124 | 61.2±9.9 | 112:12 | - | 65.5±18.6 | 90.3±64.2 | - | Dural tear (6), C5 palsy (2) | Length of stay (4.8±1.6), preop Nurick grade (3.6±1.0), postop Nurick grade (2.1±0.9) |
| Conventional group | 187 | 62.0±11.1 | 166:21 | - | 80.9±20.1 | 98.4±69.6 | - | Dural tear (6), C5 palsy (3) | Length of stay (3.7±1.3), preop Nurick grade (3.7±1.0), postop Nurick grade (2.2±1.0) | |
| Sun et al. [24] (2021) | Piezosurgery group | 38 | 64.2±6.6 | 24:14 | 58.4 | 52.3±18.2 | 155.5±41.3 | - | Dural tear (1), C5 palsy (1) | Preop VAS (5.2±1.5), postop VAS (2.8±1.6) |
| Conventional group | 26 | 63.4±5.4 | 18:18 | 56.5 | 76.0±21.8 | 177.4±54.7 | - | Dural tear (5), C5 palsy (4) | Preop VAS (5.4±1.3), postop VAS (3.9±1.7) | |
| Lin et al. [25] (2022) | Piezosurgery group | 24 | 59.2±13.5 | 19:5 | 62.0 | 198.5±48.0 | 255.4±217.5 | 370.9±184.4 | 2 | Length of stay (18.5±5.9), preop NDI (20.0±11.0), postop NDI (9.0±5.6), preop VAS (5.2±1.4), postop VAS (1.6±1.6) |
| Conventional group | 18 | 60.8±8.4 | 12:6 | 60.5 | 188.9±32.4 | 490.6±389.4 | 430.5±192.9 | 2 | Length of stay (19.7±7.1), preop NDI (19.5±8.9), postop NDI (9.2±4.0), preop VAS (5.9±1.7), postop VAS (2.0±1.5) |
Table 3
Risk of bias summary based on MINORS criteria
| Study | Clearly stated aim | Inclusion of consecutive patients | Prospective collection of data | Endpoints appropriate to the aim of the study | Unbiased assessment of the study endpoint | Follow-up period appropriate to the aim of the study | Loss to follow-up less than 5% | Prospective calculation of the study size | An adequate control group | Contemporary groups | Baseline equivalence of groups | Adequate statistical analysis | Global score |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Onen et al. [19] (2015) | 2 | 2 | 1 | 2 | 0 | 0 | 0 | 0 | 2 | 2 | 2 | 2 | 15 |
| Li et al. [20] (2016) | 2 | 2 | 2 | 2 | 2 | 2 | 0 | 0 | 2 | 2 | 2 | 2 | 20 |
| Kim et al. [21] (2020) | 2 | 1 | 2 | 2 | 2 | 2 | 1 | 2 | 2 | 2 | 2 | 2 | 22 |
| Huan et al. [22] (2020) | 2 | 1 | 2 | 2 | 1 | 1 | 0 | 0 | 2 | 2 | 2 | 2 | 17 |
| Dave et al. [23] (2020) | 2 | 2 | 1 | 2 | 0 | 2 | 1 | 0 | 2 | 2 | 2 | 2 | 18 |
| Sun et al. [24] (2021) | 2 | 1 | 2 | 2 | 2 | 2 | 0 | 0 | 2 | 2 | 2 | 2 | 19 |
| Lin et al. [25] (2022) | 2 | 2 | 2 | 2 | 0 | 2 | 0 | 0 | 2 | 2 | 2 | 2 | 18 |
References
1. Bakhsheshian J, Mehta VA, Liu JC. Current diagnosis and management of cervical spondylotic myelopathy. Global Spine J 2017 7:572–86.




2. Nouri A, Tetreault L, Singh A, Karadimas SK, Fehlings MG. Degenerative cervical myelopathy: epidemiology, genetics, and pathogenesis. Spine (Phila Pa 1976) 2015 40:E675–93.

4. Karadimas SK, Erwin WM, Ely CG, Dettori JR, Fehlings MG. Pathophysiology and natural history of cervical spondylotic myelopathy. Spine (Phila Pa 1976) 2013 38(22 Suppl 1): S21–36.


5. Feng S, Zheng B, Zhang L, Wang W. A systematic review and meta-analysis compare surgical treatment and conservative treatment in patients with cervical spondylotic myelopathy. Ann Palliat Med 2021 10:7671–80.


6. Bajamal AH, Kim SH, Arifianto MR, et al. Posterior surgical techniques for cervical spondylotic myelopathy: WFNS Spine Committee recommendations. Neurospine 2019 16:421–34.




7. Lawrence BD, Jacobs WB, Norvell DC, Hermsmeyer JT, Chapman JR, Brodke DS. Anterior versus posterior approach for treatment of cervical spondylotic myelopathy: a systematic review. Spine (Phila Pa 1976) 2013 38(22 Suppl 1): S173–82.

8. Asher AL, Devin CJ, Kerezoudis P, et al. Comparison of outcomes following anterior vs posterior fusion surgery for patients with degenerative cervical myelopathy: an analysis from quality outcomes database. Neurosurgery 2019 84:919–26.


9. Komotar RJ, Mocco J, Kaiser MG. Surgical management of cervical myelopathy: indications and techniques for laminectomy and fusion. Spine J 2006 6(6 Suppl): 252S–267S.


10. Hirabayashi K, Watanabe K, Wakano K, Suzuki N, Satomi K, Ishii Y. Expansive open-door laminoplasty for cervical spinal stenotic myelopathy. Spine (Phila Pa 1976) 1983 8:693–9.


11. Hosono N, Miwa T, Mukai Y, Takenaka S, Makino T, Fuji T. Potential risk of thermal damage to cervical nerve roots by a high-speed drill. J Bone Joint Surg Br 2009 91:1541–4.



12. Ito K, Ishizaka S, Sasaki T, et al. Safe and minimally invasive laminoplastic laminotomy using an ultrasonic bone curette for spinal surgery: technical note. Surg Neurol 2009 72:470–5.


13. Sherman JA, Davies HT. Ultracision: the harmonic scalpel and its possible uses in maxillofacial surgery. Br J Oral Maxillofac Surg 2000 38:530–2.


14. Sawamura Y, Fukushima T, Terasaka S, Sugai T. Development of a handpiece and probes for a microsurgical ultrasonic aspirator: instrumentation and application. Neurosurgery 1999 45:1192–7.


15. Horton JE, Tarpley TM Jr, Jacoway JR. Clinical applications of ultrasonic instrumentation in the surgical removal of bone. Oral Surg Oral Med Oral Pathol 1981 51:236–42.


16. Bydon M, Xu R, Papademetriou K, et al. Safety of spinal decompression using an ultrasonic bone curette compared with a high-speed drill: outcomes in 337 patients. J Neurosurg Spine 2013 18:627–33.


17. Nakagawa H, Kim SD, Mizuno J, Ohara Y, Ito K. Technical advantages of an ultrasonic bone curette in spinal surgery. J Neurosurg Spine 2005 2:431–5.


18. Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 2009 339:b2700.



19. Onen MR, Yuvruk E, Akay S, Naderi S. The reliability of the ultrasonic bone scalpel in cervical spondylotic myelopathy: a comparative study of 46 patients. World Neurosurg 2015 84:1962–7.


20. Li K, Zhang W, Li B, et al. Safety and efficacy of cervical laminoplasty using a piezosurgery device compared with a high-speed drill. Medicine (Baltimore) 2016 95:e4913.



21. Kim CH, Chung CK, Choi Y, et al. The efficacy of ultrasonic bone scalpel for unilateral cervical open-door laminoplasty: a randomized controlled trial. Neurosurgery 2020 86:825–34.



22. Huan Y, Liu J, Xing W, Zhu Z, He Y. Application of piezosurgery osteotomy in cervical laminoplasty: prospective, randomized, single-blind, clinical comparison study. Clin Surg Res Commun 2020 4:32–8.

23. Dave BR, Krishnan A, Rai RR, Degulmadi D, Mayi S, Gudhe M. The effectiveness and safety of ultrasonic bone scalpel versus conventional method in cervical laminectomy: a retrospective study of 311 patients. Global Spine J 2020 10:760–6.




24. Sun B, Xu C, Wu S, et al. Efficacy and safety of ultrasonic bone curette-assisted dome-like laminoplasty in the treatment of cervical ossification of longitudinal ligament. Orthop Surg 2021 13:161–7.




25. Lin Q, Lin T, Wang Z, Chen G, Liu W. Safety and effectiveness of modified expansive open-door laminoplasty using a ultrasonic bone scalpel compared with a high-speed drill. Clin Spine Surg 2022 35:E223–9.


26. Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J. Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 2003 73:712–6.



27. Kim K, Isu T, Matsumoto R, Isobe M, Kogure K. Surgical pitfalls of an ultrasonic bone curette (SONOPET) in spinal surgery. Neurosurgery 2006 59(4 Suppl 2): ONS390–3.



28. Nakase H, Matsuda R, Shin Y, Park YS, Sakaki T. The use of ultrasonic bone curettes in spinal surgery. Acta Neurochir (Wien) 2006 148:207–13.



29. Hazer DB, Yasar B, Rosberg HE, Akbas A. Technical aspects on the use of ultrasonic bone shaver in spine surgery: experience in 307 patients. Biomed Res Int 2016 2016:8428530.




30. Lu XD, Zhao YB, Zhao XF, et al. Efficacy and safety analysis of ultrasonic bone curette in the treatment of thoracic spinal stenosis. Orthop Surg 2019 11:1180–6.




31. Krishnan A, Samal P, Mayi S, Degulmadi S, Rai RR, Dave B. Thoracic spine stenosis: does ultrasonic osteotome improve outcome in comparison to conventional technique? Malays Orthop J 2021 15:62–9.



32. Wahlquist S, Nelson S, Glivar P. Effect of the ultrasonic bone scalpel on blood loss during pediatric spinal deformity correction surgery. Spine Deform 2019 7:582–7.


33. Schaller BJ, Gruber R, Merten HA, et al. Piezoelectric bone surgery: a revolutionary technique for minimally invasive surgery in cranial base and spinal surgery?: technical note. Neurosurgery 2005 57(4 Suppl): E410.