|
 |
- Search
| Asian Spine J > Volume 11(3); 2017 > Article |
|
Abstract
Purpose
To determine the prevalence of lumbar spondylolysis and spondylolisthesis in a general adult population unrelated to lower back pain as evaluated by multidetector computed tomography.
Overview of Literature
There is a significant paucity of information related to the prevalence of spondylolysis and spondylolisthesis and its degenerative changes in a general adult population unrelated to lower back pain in developing countries.
Methods
A retrospective study was conducted on abdominopelvic computed tomography (CT) scans performed between January 1st 2015 and December 31st 2015 for various clinical indications. Patients with lower back pain, with a history of trauma or road traffic accident, or referred from orthopedic or neurosurgery departments were excluded to avoid any bias. CT scans were reviewed in axial, sagittal, and coronal planes using bone window settings for evaluating spondylolysis and spondylolisthesis.
Results
Of 4,348 patients recruited, spondylolysis and spondylolisthesis were identified in 266 (6.1%) and 142 (3.3%) patients, respectively. Age was significantly higher in both spondylolysis and spondylolisthesis patients than in those without spondylolysis and spondylolisthesis (47.19┬▒15.45 vs. 42.5┬▒15.96, p<0.001 and 53.01┬▒15.31 vs. 42.44┬▒15.88, p<0.001, respectively). Gender was significantly associated with spondylolisthesis (p=0.029) but not spondylolysis. Of patients who were >60 years old, both spondylolysis (p=0.018) and spondylolisthesis (p=0.025) were significantly more prevalent in females.
Anatomical defects in the vertebral pars interarticularis are commonly referred to as spondylolysis, and slippage of the body of the vertebra immediately below is referred to as spondylolisthesis. Lumbar spondylolysis is a frequently encountered problem and usually arises as a result of increased stress on the pars interarticularis. This stress may be related to monotonous extension, flexion, or rotation of the lumbar spine during bipedal movement in humans [12] or activities that aggravate such stresses [34]. Spondylolisthesis has two important causes. The first is associated with the degeneration of the intervertebral disc or posterior facet joints and is referred to as the degenerative type. The second occurs in relation with spondylolysis and is known as the isthmic type. Isthmic spondylolisthesis most commonly occurs at the L5/S1 level [5], while degenerative spondylolisthesis most commonly occurs at the L4/L5 level [67].
In a symptomatic population, the prevalence of spondylolysis and spondylolisthesis has been adequately studied. The reported frequency of spondylolisthesis associated with low back pain is 67.4% [8], and most previous studies have been conducting using plain radiographs [9]. However, computed tomography (CT) is considered to represent a particularly accurate tool for evaluating pars defects as it can often reveal a pars fracture early without the development of spondylolisthesis [1011]. In a study in an adult community-based population, CT examinations showed that the prevalence of lumbar spondylolysis was 11.5% [12].
This study aimed to evaluate the prevalence of spondylolysis and spondylolisthesis in a general adult population unrelated to lower back pain. Most studies on this topic have been reported from developed countries. As the present study was conducted in a population in a developing country for the first time, our data provide a fresh viewpoint and represent a valuable addition to the existing literature.
This retrospective cross-sectional study was conducted at Dow Institute of Radiology, Dow University of Health Sciences. Patients who underwent CT scans between January 1st, 2015 and December 31st, 2015 were included. Our specific inclusion criteria were (1) patients above the age of 18 years, and (2) patients presenting for CT of the abdomen and pelvis for various abdominal, pelvic, or urological indications. Our exclusion criteria were (1) patients with lower back pain, (2) patients with a history of trauma or road traffic accident, and (3) referred from orthopedic or neurosurgery departments (to avoid any bias). Based upon these inclusion and exclusion criteria, we recruited a total of 4,348 patients. They were divided into six groups based upon their age: group 1, 18ŌĆō30 years; group 2, 31ŌĆō40 years; group 3, 41ŌĆō50 years; group 4, 51ŌĆō60 years; group 5, 61ŌĆō70 years; and group 6, >70 years).
CT scans were performed on one of two 16-slice MDCT machines (Brightspeed [GE Medical Systems, Milwaukee, WI, USA] or Somatom Emotion [Siemens AG, Erlangen, Germany]). Axial slice thickness varied from 0.75 to 5 mm depending on the specific protocol required, which was based on clinical indications.
All CT scans were evaluated in a blinded fashion with respect to the clinical information provided. All scans were reviewed by two radiologists with more than five years of experience in cross-sectional imaging. Images were analyzed on a Picture Archiving and Communication System. The entire lumbosacral spine was evaluated using bone window settings. Axial sections, along with reconstructed sagittal and coronal images, were used for the diagnosis of spondylolysis and spondylolisthesis.
Using bone window settings, a fracture of the pars interarticularis is seen as linear lucency or a defect and is more evident on sagittal images. Fractures were identified and denoted as being present on either the right or left side or bilaterally.
SPSS ver. 20 (IBM, Armonk, NY, USA) was used for statistical analysis. Descriptive statistics were explored using mean and standard deviation for quantitative data and frequency and percentage for qualitative variables. The unpaired t-test was applied to investigate age differences among patients with and without spondylolysis and with and without spondylolisthesis. The chi-square test was applied to investigate association outcomes with general characteristics such as age categories, gender, and the site of damage. A p<0.05 was considered to be statistically significant.
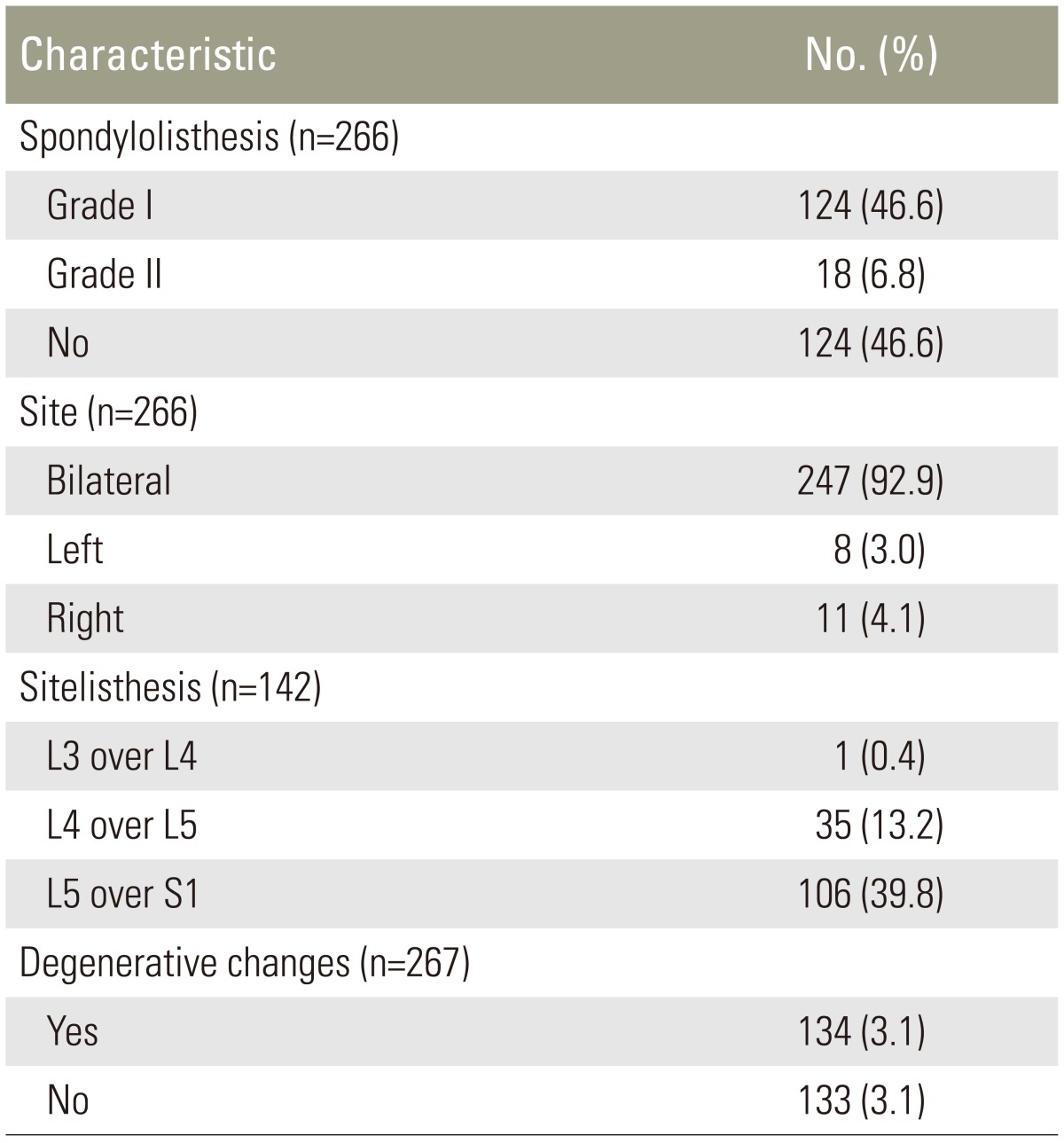
A total of 4,348 patients were included. The mean┬▒standard deviation age was 42.74┬▒16.01 years. Our study featured more males (n=2,320, 53.4%) than females (n=2,028, 46.6%). The clinical characteristics of patients with spondylolysis and those with spondylolisthesis are shown in Table 1.
Spondylolysis was identified in 266 patients (6.1%), while spondylolisthesis was observed in 142 patients (3.3%). Of the 266 patients with spondylolysis, a break in the pars interarticularis at L3 was observed in 5 (1.9%), L4 in 44 (16.5%), and L5 in 217 (81.6%). There were 247 patients (92.9%) with fractures of the bilateral pars interarticularis, 8 patients (3%) with fractures of the pars interarticularis on the left side and 11 (4.1%) with fractures on the right side.
Of the 142 patients with spondylolisthesis, grade I spondylolisthesis was most commonly observed and was identified in 124 patients (87.3%); grade II spondylolisthesis was observed in 18 patients (12.7%). None of our patients had grade III or grade IV spondylolisthesis. Most patients (106, 74.6%) had spondylolisthesis of L5 over S1, followed by L4 over L5 35 (24.6%), and only one patient (0.7%) had spondylolisthesis of L3 over L4 (Figs. 1, 2).
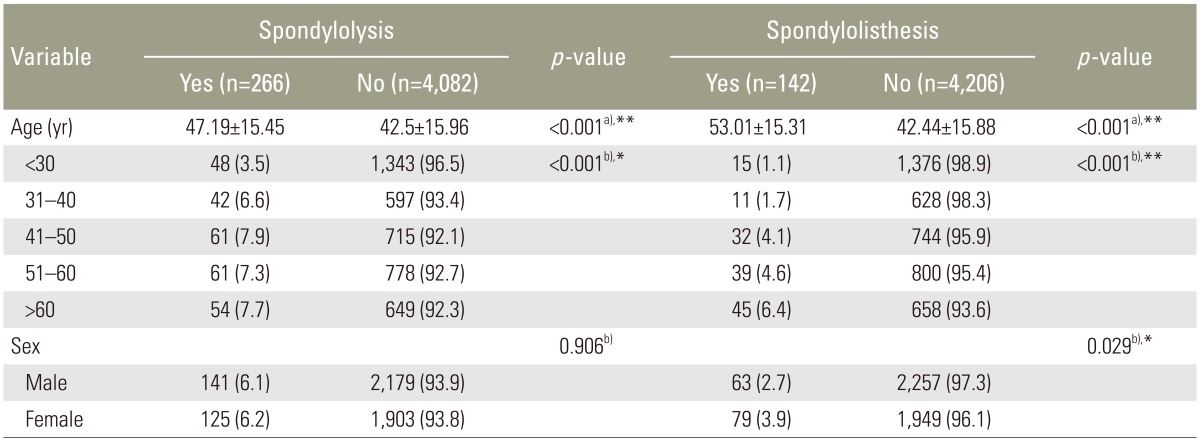
The mean┬▒standard age of patients with spondylolysis was significantly higher than that of patients without spondylolysis (47.19┬▒15.45 vs. 42.5┬▒15.96 years, p<0.001). Similarly, the mean┬▒standard deviation age of patients was higher among patients with spondylolisthesis than those without spondylolisthesis (53.01┬▒15.31 vs. 42.44┬▒15.88 years, p<0.001). However, gender was only significantly associated with spondylolisthesis (p=0.029) (Table 2).
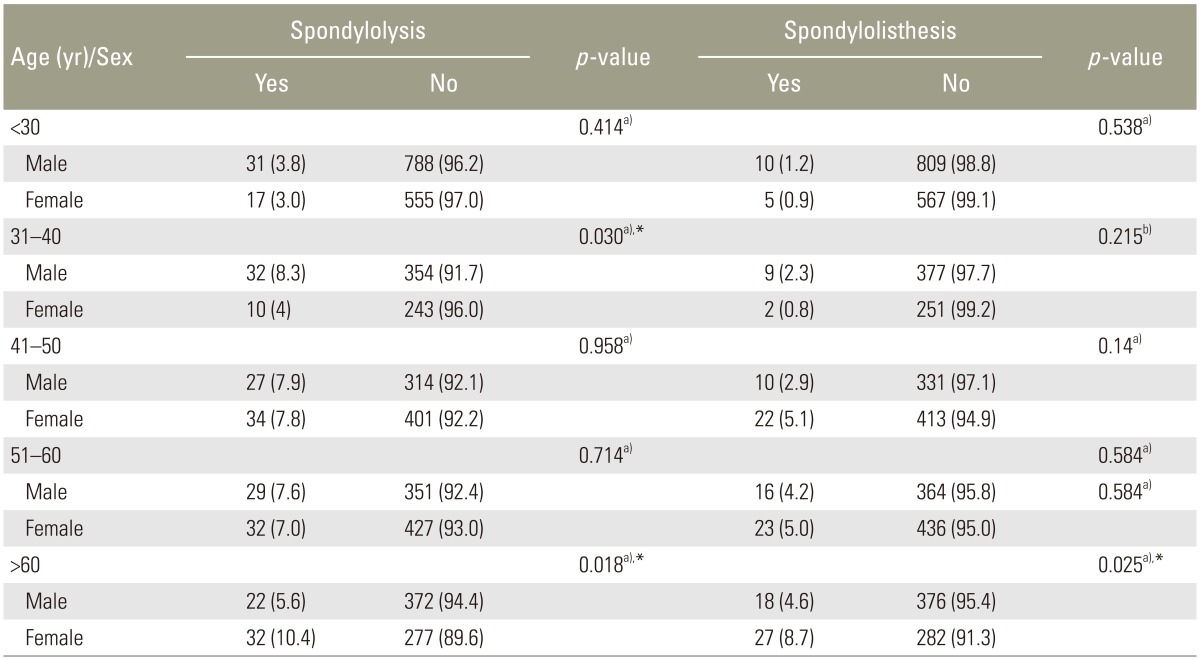
Stratification of age showed that there was a significant association of spondylolysis and gender among patients aged 31ŌĆō40 years (p=0.03) and patients aged >60 years (p=0.018), while a significant association of spondylolisthesis with gender was found only among patients aged >60 years (p=0.025) (Table 3). A comparison of the anatomical site and spondylolisthesis also showed significant association (p=0.002).
In contrast with earlier studies, the findings in the present study revealed a slightly lower prevalence of spondylolysis [121314]. However, two previous studies conducted in Asia showed a slightly lower prevalence than existing studies, thus concurring with our current findings [1516]. We believe that the lower prevalence in our study is due to the difference in study population and the possible role of genetic factors
In the present study, a greater number of patients with spondylolysis had a bilateral fracture of the pars interarticularis with a predominant involvement of the L5 vertebra. Unilateral spondylolysis was identified in less than 10% of patients, which was lower than that reported in previous studies [1516]; this difference may be attributed to a compensatory response to mechanical stress.
In terms of gender distribution, our study revealed a surprisingly high incidence of spondylolysis among females. This is in contrast to previously published studies, which have shown that spondylolysis is more common in males [14151617]. Previous studies have revealed different male-to-female ratios for spondylolysis, including 1.5:1 [14] and 2:1 [1516], and according to one study, this ratio ranged from 2:1 to 4:1 [2]. All these studies reported a higher chance of developing a break in the pars interarticularis in males. However, in our present study, the male-to-female ratio was approximately 1:1. This may be due to the fact that majority of the females in underdeveloped countries usually begin working from a very young age. These defects are more common at the age of 7 or 8 years [18] and usually occur following chronic repetitive stress at the pars interarticularis. Thus, it can be hypothesized that starting work from an early age and engaging in laborious work leads to continuous stress at the pars interarticularis that may subsequently lead to damage.
Multilevel spondylolysis has been described by some authors [1920], and a high prevalence of multilevel spondylolysis was observed in a radiographic-based study [19]. Nine patients showed spondylolysis at multiple levels in the present study with prevalence almost equal to that in a CT-based study [16] but lower than that in another study [19]. This could have been due to the greater accuracy of CT in depicting pars fractures as well as the different population of patients being evaluated.
In our study, the prevalence of spondylolisthesis was very similar to that reported by an earlier study [15]. However, the prevalence of spondylolisthesis in patients with a fracture of the pars interarticularis was slightly lower than that reported in a previous study [16].
Defects in the pars interarticularis do not always progress to spondylolisthesis. This was observed in our study, where approximately more than 45% of patients with spondylolysis did not develop spondylolisthesis. Other authors have also reported a similar finding: up to 55% of patients diagnosed with spondylolysis did not progress to spondylolisthesis [212223].
The prevalence of isthmic spondylolisthesis was also higher among females in the current study. This was also surprisingly high compared to a previous study [17]. Spondylolisthesis, or slippage of the vertebral body, is more common in a person who has not yet reached maturity [24]. Slippage usually occurs between the bony and cartilaginous end plates and can also include the growth plate, which represents the weak link to straining forces [2526]. Thus, we can speculate that fragile growth plates in females are more prone to slippage and thus led to the higher prevalence of spondylolisthesis observed in the current study.
Our study demonstrated that with advancing age, there is a gradual increase in the prevalence of spondylolysis. These findings are not in agreement with those previously reported in a large CT-based study, which stated that the prevalence of spondylolysis is not significantly different between younger and older patients [14]. However, a study based on large plain radiographs reported that the prevalence of lumbar spondylolysis increased throughout life [9].
Among those patients identified with spondylolysis, approximately half had degenerative changes at multiple spinal levels. These changes included anterior and posterior osteophytes, vacuum phenomena, and facet joint arthrosis. Other significant findings associated with vertebral bodies were found in patients with spondylolysis.
A major limitation of our study was that it was a single institution retrospective study. Despite this limitation, we believe that this is represents the largest CT-based study to determine the prevalence of spondylolysis and spondylolisthesis from a developing country such as Pakistan. However, prospective studies in developing countries are recommended to further validate the findings of this study.
Notes
Conflict of Interest: No potential conflict of interest relevant to this article was reported.
References
1. Leone A, Cerase A, Lauro L, Cianfoni A, Aulisa L. Postoperative lumbar spine. Rays 2000 25:125ŌĆō136. PMID: 10967640.

2. Rauch RA, Jinkins JR. Lumbosacral spondylolisthesis associated with spondylolysis. Neuroradiol Clin North Am 1993 3:543ŌĆō553.
3. Iwamoto J, Abe H, Tsukimura Y, Wakano K. Relationship between radiographic abnormalities of lumbar spine and incidence of low back pain in high school rugby players: a prospective study. Scand J Med Sci Sports 2005 15:163ŌĆō168. PMID: 15885037.


4. Lundin DA, Wiseman DB, Shaffrey CI. Spondylolysis and spondylolisthesis in the athlete. Clin Neurosurg 2002 49:528ŌĆō547. PMID: 12506568.

5. Wiltse LL, Winter RB. Terminology and measurement of spondylolisthesis. J Bone Joint Surg Am 1983 65:768ŌĆō772. PMID: 6863359.


6. Fitzgerald JA, Newman PH. Degenerative spondylolisthesis. J Bone Joint Surg Br 1976 58:184ŌĆō192. PMID: 932080.


7. Bookhout MR. Evaluation and conservative management of spondylolisthesis. J Back Musculoskelet Rehabil 1993 3:24ŌĆō31. PMID: 24573137.


8. Ahmad S, Danish SH, Ahmad F, Naz S, Tahir A, Ali SMS. Frequency of spondylolisthesis among patients of chronic low back pain in karachi. J Dow Uni Health Sci 2013 7:101ŌĆō106.
9. Sonne-Holm S, Jacobsen S, Rovsing HC, Monrad H, Gebuhr P. Lumbar spondylolysis: a life long dynamic condition? A cross sectional survey of 4.151 adults. Eur Spine J 2007 16:821ŌĆō828. PMID: 17120072.


10. Teplick JG, Laffey PA, Berman A, Haskin ME. Diagnosis and evaluation of spondylolisthesis and/or spondylolysis on axial CT. AJNR Am J Neuroradiol 1986 7:479ŌĆō491. PMID: 3085451.


11. Krupski W, Majcher P, Tatara MR. Computed tomorgaphy diagnostic of lumbar spondylolysis. Ortop Traumatol Rehabil 2004 6:652ŌĆō657. PMID: 17618216.

12. Kalichman L, Kim DH, Li L, Guermazi A, Berkin V, Hunter DJ. Spondylolysis and spondylolisthesis: prevalence and association with low back pain in the adult community-based population. Spine 2009 34:199ŌĆō205. PMID: 19139672.



13. Ko SB, Lee SW. Prevalence of spondylolysis and its relationship with low back pain in selected population. Clin Orthop Surg 2011 3:34ŌĆō38. PMID: 21369476.



14. Brooks BK, Southam SL, Mlady GW, Logan J, Rosett M. Lumbar spine spondylolysis in the adult population: using computed tomography to evaluate the possibility of adult onset lumbar spondylosis as a cause of back pain. Skeletal Radiol 2010 39:669ŌĆō673. PMID: 19911181.


15. Belfi LM, Ortiz AO, Katz DS. Computed tomography evaluation of spondylolysis and spondylolisthesis in asymptomatic patients. Spine (Phila Pa 1976) 2006 31:E907ŌĆōE910. PMID: 17108819.


16. Sakai T, Sairyo K, Takao S, Nishitani H, Yasui N. Incidence of lumbar spondylolysis in the general population in Japan based on multidetector computed tomography scans from two thousand subjects. Spine (Phila Pa 1976) 2009 34:2346ŌĆō2350. PMID: 19934813.


17. Takao S, Sakai T, Sairyo K, et al. Radiographic comparison between male and female patients with lumbar spondylolysis. J Med Invest 2010 57:133ŌĆō137. PMID: 20299752.


18. Hensinger RN. Spondylolysis and spondylolisthesis in children and adolescents. J Bone Joint Surg Am 1989 71:1098ŌĆō1107. PMID: 2668295.


19. Sakai T, Yamada H, Nakamura T, et al. Lumbar spinal disorders in patients with athetoid cerebral palsy: a clinical and biomechanical study. Spine 2006 31:E66ŌĆōE70. PMID: 16449890.


20. Al-Sebai MW, Al-Khawashki H. Spondyloptosis and multiple-level spondylolysis. Eur Spine J 1999 8:75ŌĆō77. PMID: 10190858.



21. Fredrickson BE, Baker D, McHolick WJ, Yuan HA, Lubicky JP. The natural history of spondylolysis and spondylolisthesis. J Bone Joint Surg Am 1984 66:699ŌĆō707. PMID: 6373773.


22. Beutler WJ, Fredrickson BE, Murtland A, Sweeney CA, Grant WD, Baker D. The natural history of spondylolysis and spondylolisthesis: 45-year follow-up evaluation. Spine (Phila Pa 1976) 2003 28:1027ŌĆō1035. PMID: 12768144.


23. Saraste H. Spondylolysis and spondylolisthesis. Acta Orthop Scand Suppl 1993 251:84ŌĆō86. PMID: 8451998.


24. Sairyo K, Katoh S, Ikata T, Fujii K, Kajiura K, Goel VK. Development of spondylolytic olisthesis in adolescents. Spine J 2001 1:171ŌĆō175. PMID: 14588344.


25. Kajiura K, Katoh S, Sairyo K, Ikata T, Goel VK, Murakami R-I. Slippage mechanism of pediatric spondylolysis: biomechanical study using immature calf spines. Spine 2001 26:2208ŌĆō2213. PMID: 11598509.


26. Konz RJ, Goel VK, Grobler LJ, et al. The pathomechanism of spondylolytic spondylolisthesis in immature primate lumbar spines in vitro and finite element assessments. Spine (Phila Pa 1976) 2001 26:E38ŌĆōE49. PMID: 11224899.


Fig.┬Ā1
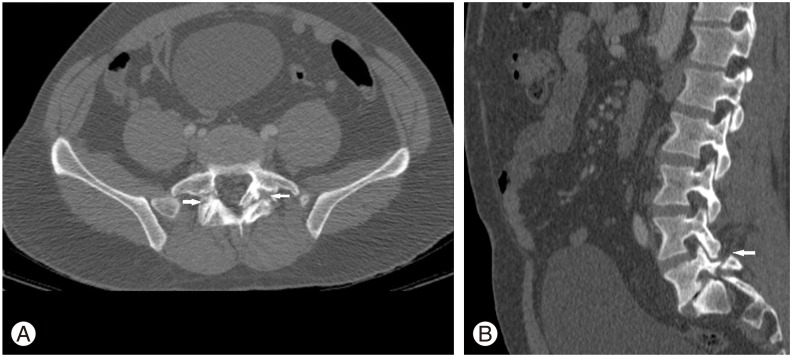
Computed tomography scan bone window image of a 19-year-old male presenting with abdominal pain. (A) Axial sections showing a bilateral break in the pars interarticularis (arrows). (B) Sagittal reconstructed image of the same patient showing a break of the pars interarticularis at the L5 level (arrow).
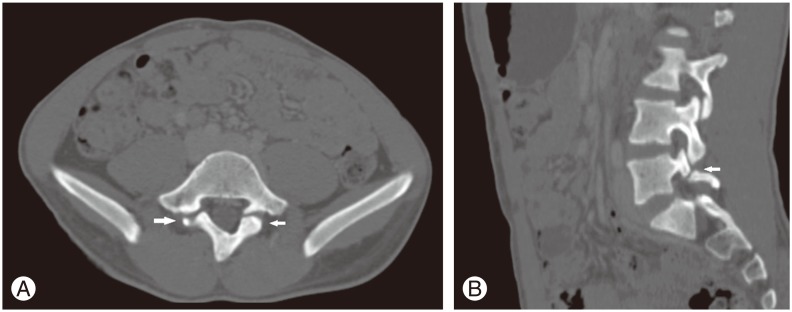
Fig.┬Ā2
Computed tomography scan bone window of a 38-year-old male presenting with severe pain in the epigastric region. (A) Axial images showing a bilateral pars interarticularis fracture (arrows). (B) Sagittal reconstruction of the same patient showing a fracture of the pars interarticularis involving L5 with grade II spondylolisthesis (arrow). Mild degenerative changes were also seen with vacuum phenomena at the L5/S1 level.
- TOOLS