|
 |
- Search
| Asian Spine J > Volume 12(5); 2018 > Article |
|
Abstract
Purpose
The purpose of this study was to evaluate the clinical efficacy and safety profile of open-door laminoplasty (ODL) using titanium mesh.
Overview of Literature
The most appropriate surgical management of degenerative spine disorders, particularly ossification of the posterior longitudinal ligament, remains controversial and continues unabated in the neurosurgical community. However, recently, ODL has become popular among surgeons. Many modifications have been developed since Hirabayashi in 1983 to enhance the clinical efficacy and safety of this procedure.
Methods
We reviewed the obtained data of patients with ossification of the posterior longitudinal ligament (OPLL) who underwent ODL using titanium mesh at Neurosurgery Subdivision, the Dr. Sardjito Hospital, Yogyakarta, Indonesia, during January 2013–December 2015. Motor improvement (Nurick score), axial neck pain (neck disability index [NDI]), and incidence of complications were pre- and postoperatively examined, and the clinical efficacy and safety of the procedure was evaluated. Data were analyzed using Wilcoxon signed-rank test and paired t-test.
Results
This study included five patients were included (i.e., four males and one female) with mean age of 47.00±9.68 years, where reassessments were done after mean follow up of 20.2±4.74 months. Mean duration of surgery was 165±12.55 minutes. Pre- and postoperative motor assessments were 3.4±1.52 and 2.0±1.22 (p =0.059), respectively. Axial neck pains using NDI were 23.60±7.44 and 12.40±6.50 (p =0.004) before and after operations, respectively. No infected postoperative scar was found, and only one patient had a left C5 motor palsy.
The most appropriate surgical management of degenerative spine disorders, particularly ossification of the posterior longitudinal ligament (OPLL), remains controversial and continues unabated [1,2]. Laminoplasty was first introduced by Oyama and Hattori in 1972, and further improved as open-door laminoplasty (ODL) by Hirabayashi and colleagues in 1983. This surgical approach has become a critical posterior decompression technique for multisegment cervical canal stenosis without permanently removing dorsal elements of the cervical spine. Subsequently, several further modifications have been proposed, which have improved its the efficacy and safety [3-5].
Recently, ODL has been frequently opted by surgeons because from the long-term follow-up study, it has offered greater patient satisfaction with improvement on the motor scale, less risk than radical anterior approach, and superiority over conventional laminectomy. This procedure can preserve cervical spine stability, prevent canal stenosis due to scar formation, and cause less frequent axial pain [6-8].
Although ODL has fewer complications than laminectomy, there are still several issues that frequently occur in patients undergoing ODL, such as axial neck pain, C5 motor palsy, and canal stenosis [9]. The main factors associated with postoperative C5 motor palsy are tethering, traction, and/or kinking of the nerve root secondary to posterior shift of the spinal cord. Avoidance of excessive decompression and tight fixation of reconstructed laminae are essential in cervical laminoplasty [10-12]. Meanwhile, wider exposed epidural space due to excessive opening of the open-door side can lead to the formation of more epidural scar tissues, resulting in canal stenosis and contributing to axial neck pain development [13]. Therefore, this study proposes a novel technique to maintain the open-door side using titanium mesh to overcome the abovementioned issues. Moreover, clinical efficacy and safety profile were evaluated and discussed to show the potential and feasibility of using this procedure for enhanced ODL with fewer complications.
This cross-sectional study was reviewed and approved by the Ethics Committee of Medical Research and Health, Medical Faculty of Universitas Gadjah Mada (IRB approval no., KE/FK/986/EC/2016). This study included all patients with OPLL showing myelopathy or radiculopathy symptoms who underwent enhanced ODL using titanium mesh performed by a neurosurgeon at the Dr. Sardjito Hospital, Yogyakarta, Indonesia, during January 2013–December 2015. However, patients with (1) preoperatively obtained cervical kyphosis or instability, (2) revision surgery, (3) hybrid anterior–posterior surgery, (4) tumors, (5) ankylosing spondylitis, (6) cerebrovascular disease, and (7) Parkinson’s disease were excluded.
Patient characteristics, including age, gender, duration of surgery, amount of bleeding, period of follow-up, and duration of symptoms, were obtained from medical records of each patient. Postoperative clinical evaluations of patients, including motor improvement using Nurick score, axial neck pain employing Visual Analogue Scale (VAS) and Neck Disability Index (NDI) scores, postoperative infections, and C5 motor palsy, were performed during daily follow-up, management of patients after surgery in the hospital, and outpatient care when patients visited the neurosurgery clinic for checkup. Moreover, after obtaining a written informed consent from patients and their families, the latest postoperative clinical evaluation was performed by directly visiting the patients at their residence to ensure optimal recovery after surgery. Postoperative clinical evaluation data were recorded in previously prepared research sheets, documented in the form of photos and videos, and subsequently analyzed using Wilcoxon signed-rank test and paired t-test with IBM SPSS ver. 21.0 (IBM Corp., Armonk, NY, USA).
Prior to the surgery, patients were administered general anesthesia, intubated with endotracheal tube, and placed in the prone position with 30° neck flexion from the elevated horizontal plane table. Incision was performed from the inion to one level below the lowest segment of lesion along the midline. Both paraspinal muscles were detached from the lamina using monopolar diathermy or raspatorium, thereby exposing the lamina (i.e., the junction between lamina and lateral mass and the edge of the lateral mass of all levels of lesion). Interspinous, supraspinous, and flavum ligaments, located between the highest and the lowest segment of cervical lesions, were cut using 1-mm Kerrison punch.
Next, a trough on the open-door side was created using a 3-mm burr (Aesculap, Tuttlingen, Germany) at 4,000 rpm on the left lateral side at the lamina–lateral mass junction corresponding to the level of the lesion. This was then followed by the formation of a gap on the right side using a 1-mm Kerrison punch, thus exposing the opendoor side. Another trough was created on the hinge side, which was located 2 mm distal from the junction (Fig. 1).
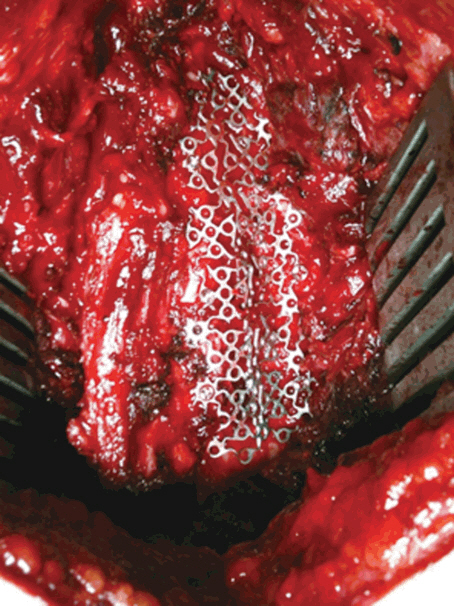
Once the open-door side was generated, it was opened by the surgeon using both thumbs and then held by the assistant operator. The produced bleeding from venous plexus was controlled with a gelatin sponge (Curaspon; Cura Medical, Amsterdam, The Netherlands), collagen fleece (Lyostypt, B Braun; Aesculap), and Surgicel Fibrillar absorbable hemostat (Ethicon; Johnson-Johnson, Brussels, Belgium) and coagulated with bipolar diathermy. Meanwhile, fixation was employed using M4 rigid fixation system (OsteoMed, Addison, TX, USA). S-shaped titanium mesh (Pre-Formed OsteoForm Mesh, OsteoMed), with the length corresponding to the lesion length and a width of 5 cm, was subsequently designed and tailored (Fig. 2). Afterward, the medial side was fixed in the lamina, which had been already opened with a screw having a diameter of 2 mm and a length of 8 mm (Mini Auto-Drive Screw, OsteoMed), and a longer screw, with a diameter of 2 mm and a length of 12 mm (Mini Screw, OsteoMed), was mounted on the lateral masses using Anderson’s technique at all levels of the lesion.
Then, both the paraspinal muscles were resutured and approximated using an absorbable multifilament thread (size, 2/0) as tension sutures. Drain was inserted in the submuscular area, which was subsequently followed by layer-by-layer suturing. The skin was sutured using a nonabsorbable monofilament thread (size, 2/0) with simple interrupted stitch. Lastly, the surgical wound was closed using tulle (sterile gauze) combined with a plaster.
After surgery, the patients were mobilized from the first day using soft neck collar for 3 months. Meanwhile, the submuscular drain was removed after 2–3 days, when the drain product was minimal. Patients were discharged after 7 days of intensive medical care, along with physiotherapy provided during this treatment.
This study included five patients (four males [80%] and one female [20%]; mean age, 47.00±9.68 years; age range, 40–62 years). Clinical symptoms were evident within the mean duration of 6.90±9.9 months. Neck pain radiating to both arms and weakness of the upper and lower limbs were seen in four patients. The symptoms appeared in two patients after trauma, while degenerative processes are dominant for the other subjects.
All patients underwent ODL using titanium mesh, including two patients who experienced trauma and did not have duraplasty. Mean duration of surgery was 165.00±12.55 minutes, and mean blood loss during surgery was 300.00±228.03 mL (range, 100–700 mL) (Table 1).
Mean preoperative Nurick score was 3.40±1.52 (range, 1–5). Two patients had moderate neck disability dysfunction, and the remaining three patients had severe degree problems, with a mean preoperative NDI value of five patients is 23.60±7.44 (range, 15–30). Moreover, the mean VAS score was 30.20±21.47 mm (range, 0–59 mm) (Table 2). In this study, clinical evaluation was performed using follow-up and visitation with a mean value follow-up are 20.2±4.74 months postoperative.
Mean postoperative Nurick score was 2.00±1.22. Bivariate analysis with Wilcoxon signed-rank revealed a Z-value of −1.890 (p=0.059). There was also postoperative improvement in axial neck pain symptom, with mean NDI of 12.40±6.50 (range, 4–21) and mean and VAS score of 7.80±4.86 mm (range 0–12.5). Statistical analysis using paired t-test revealed t=6.04 (p=0.004) for NDI score and t=2.72 (p=0.053) for VAS score (Table 2). These complaints (axial neck pain) have arisen before the patient underwent surgery and persisted postoperatively with reduced intensity. Surgical wound infection was not observed in any patient. One patient had a C5 motor palsy on the left side with a motor strength of 4/5. However, the remaining patients did not develop C5 motor palsy.
Cervical laminoplasty is used for decompression with a posterior approach in cases of compression myelopathy caused by canal stenosis of some degree because of OPLL or cervical spondylosis. Several laminoplasty approaches have been introduced; among them, unilateral ODL has been considered to be the easiest and safest approach [8,14,15]. This technique, first introduced by Hirabayashi and colleagues in 1983, used sutures to successfully maintain the open-door side, regardless of the reported springback phenomena. To complement it, the use of miniplates adapted from cranial fixation systems for securing the cervical laminoplasty was described by Frank and Keenen. O’Brien subsequently quantified the expanded canal area after laminoplasty action, which made this procedure well known and favorable in surgery [16,17]. Nevertheless, excessive opening of the open-door side may still lead to the formation of more epidural scar tissue [13], which is the gap between the titanium plates, providing space for scar tissue to enter into cervical canal and promoting canal stenosis. These issues can contribute to radiological as well as neurological deteriorations of the obtained results [18,19].
Therefore, in this study, the use of titanium mesh instead of titanium plate was proposed to maintain the patency of the open-door side. Using this method, the construction of open-door side will be more rigid, thereby preventing postoperative kyphosis and paraspinal muscle fibrosis from entering the gap between titanium plates. Based on the pre- and postoperative Nurick scale results, it can be said that the enhancement of postoperative motor function using a titanium mesh is prominent.
Highsmith et al. [17] used a modified O’Brien’s technique and reported preoperative and postoperative Nurick scores of 2.9±1.2 and 1.5±1.1, respectively (p<0.01). Meanwhile, Yang et al. [20] employed a similar procedure and reported preoperative and postoperative Nurick scores of 2.40±0.96 and 0.65±0.71, respectively (p>0.05). Furthermore, another study using Hirabayashi’s technique reported preoperative and postoperative Nurick scores of 3.23 and 1.71, respectively (p=0.002) [21]. Therefore, by comparing the results of the present study with those of the aforementioned studies, it is obvious that enhanced ODL using titanium mesh has agreed well with the already widely used O’Brien’s and Hirabayashi’s surgical methods, confirming its usability as a promising alternatives of ODL.
However, the widely applied laminoplasty methods reportedly have the incidence of complications of 5.2%–57.5%. The frequent complications include axial neck pain and C5 motor palsy [9,22,23]. Axial neck pain may originate from several sources, i.e., denervation of deep extensor muscle, release of cervical muscle from C2 to C7, discharge of nuchal ligament, partially damaged zygapophysial joints for making grooves, nerve fibers, and excessive use of external immobilization [24,25]. In another study, Hosono et al. [24] reported axial symptoms that appeared within 1 year after laminoplasty in 60% of patients. Meanwhile, Ohnari and colleagues had shown more axial symptom of the patients (i.e., 42 of the 51 subjects, 82%) after surgery in their research investigation [26]. Similarly, four of five patients (80%) in the present study exhibited axial symptoms. However, it should be noted that the symptoms had only occurred in patients who previously already experienced identical symptoms prior to surgery. Therefore, they continued to exhibit the symptoms after surgery but with different intensities. Compared with the preoperative condition (i.e., VAS score=30.20±21.47 mm), postoperative neck pain symptoms had improved (i.e., VAS score=7.80±4.86 mm); however, this was not statistically significant (p=0.053). In a study conducted by Yeh et al. [16], using laminoplasty using miniplate, axial neck pain was reportedly enhanced from 5.1±1.8 to 2.3±2.2 postoperatively. However, different results were obtained by Lee et al. [27], wherein the neck pain did not have much progress after 5 years of evaluation, with mean pre- and postoperative VAS scores of 2.7±0.6 and 2.8±0.4, respectively. Chronic neck pain and stiffness are two of the persistent symptoms in patients with cervical spine lesions [28]. Compared with some of the above data about postoperative axial neck pain and a research of Kawaguchi et al. [15], there is an equal number of 80% for patients with similar postoperative complaints [26,29].
In this study, titanium mesh modification significantly improved the neck pain (NDI). In comparison with other studies using titanium miniplate, in which the obtained results had varying NDI values [5,20,26], results from this study depict similar trends in terms of NDI enhancement results.
The axial pain in this series of cases might be attributed to the prolonged use of the soft neck collar, which could lead to neck muscle contractures and osteoarthritis. This was exacerbated by some patients having weakness in all four limbs, thereby limiting the neck movements. Some patients were frightened to move their neck freely; thus, the exercise provided was inadequate and could have reduced muscle mass [28]. Besides, another common complication was C5 motor palsy, with no worsening of myelopathy symptoms. Many theories have been proposed to understand this phenomenon (e.g., direct damage in C5 nerve fibers during surgical procedures, heat generated during drilling, or use of Kerrison rongeur). Another possible cause is the traction of nerve fibers, known as tethering, which is due to excessive posterior shift of the spinal cord after the decompression procedure [10,22,24,30].
Among the investigated subjects, one patient exhibited a postoperative weakness in C5 nerve fibers, occurring on the left side where the hinge of the ODL was located. Based on the literature, the incidence of clinical complications is 5%–12.5%, in which a higher incidence value can originate from the small number of examined cases. Meanwhile, for various types of laminoplasty, mean volume of intraoperative bleeding is approximately 52–370 mL and mean duration of surgery is approximately 50–223 minutes [16]. In this study, the mean volume of intraoperative bleeding as well as duration of surgery were within the normal range compared to previous studies from Yeh et al. [16] in 2014. No patient had superficial or deep infections. The incidence of surgical wound infection was 3%–4%. Administration of perioperative antibiotics and good surgical techniques could minimize the incidence of surgical wound infection [25].
This study has the following limitations: the small number of research subjects within a limited research area, short period of patient evaluation, lack of control group, incomplete medical records of some patients due to low postoperative patient visits, and unscheduled visit. Despite the limitations, the surgical technique of enhanced ODL using titanium mesh proposed in this study has shown promising results; therefore, it can be utilized as an alternative to the commonly used ODL using miniplate. However, further studies with more subjects and also another examination such as postoperative radiologic evaluation, amount of fibrosis that invades the open-door side, long-term follow-up for axial neck pain, and motor improvement should be conducted for further optimizing the results and understanding some unclear phenomena.
The clinical results of the present study obtained from the motor evaluation, NDI, and VAS score suggest that enhanced ODL using titanium mesh has favorable outcome and safety profile compared to the conventional method using miniplate. A detailed procedure of the surgery has been described involving the titanium mesh engineering, bleeding treatment, and stitching mechanism. Further investigation with a larger number of patients is necessary in the future to strengthen the experimental results and confirm the advantages of the proposed surgical technique.
Table 1.
Demographic data of the patients observed in this study of open-door laminoplasty surgery with titanium mesh
Table 2.
Clinical outcomes from the observed patients in terms of motoric evaluation, NDI, and VAS
References
1. Wang MY, Shah S, Green BA. Clinical outcomes following cervical laminoplasty for 204 patients with cervical spondylotic myelopathy. Surg Neurol 2004 62:487–92.


2. Vitzthum HE, Dalitz K. Analysis of five specific scores for cervical spondylogenic myelopathy. Eur Spine J 2007 16:2096–103.



4. Thakur NA. Laminoplasty: indication, techniques, and complications. Semin Spine Surg 2014 26:91–9.

5. Chen H, Deng Y, Li T, Gong Q, Song Y, Liu H. Clinical and radiography results of mini-plate fixation compared to suture suspensory fixation in cervical laminoplasty: a five-year follow-up study. Clin Neurol Neurosurg 2015 138:188–95.


6. Gu Z, Zhang A, Shen Y, Li F, Sun X, Ding W. Relationship between the laminoplasty opening size and the laminoplasty opening angle, increased sagittal canal diameter and the prediction of spinal canal expansion following open-door cervical laminoplasty. Eur Spine J 2015 24:1613–20.


7. Mizuno J, Nakagawa H. Ossified posterior longitudinal ligament: management strategies and outcomes. Spine J 2006 6(6 Suppl): 282S–8S.


8. Seichi A, Hoshino Y, Kimura A, et al. Neurological complications of cervical laminoplasty for patients with ossification of the posterior longitudinal ligament: a multi-institutional retrospective study. Spine (Phila Pa 1976) 2011 36:E998–1003.


9. Ratliff JK, Cooper PR. Cervical laminoplasty: a critical review. J Neurosurg 2003 98(3 Suppl): 230–8.


10. Chiba K, Toyama Y, Matsumoto M, Maruiwa H, Watanabe M, Hirabayashi K. Segmental motor paralysis after expansive open-door laminoplasty. Spine (Phila Pa 1976) 2002 27:2108–15.


11. Ogawa Y, Toyama Y, Chiba K, et al. Long-term results of expansive open-door laminoplasty for ossification of the posterior longitudinal ligament of the cervical spine. J Neurosurg Spine 2004 1:168–74.


12. Tanaka S, Tashiro T, Gomi A, Ujiie H. Cervical unilateral open-door laminoplasty with titanium miniplates through newly designed hydroxyapatite spacers. Neurol Med Chir (Tokyo) 2011 51:673–7.


13. Wang XY, Dai LY, Xu HZ, Chi YL. Prediction of spinal canal expansion following cervical laminoplasty: a computer-simulated comparison between single and double-door techniques. Spine (Phila Pa 1976) 2006 31:2863–70.


14. Satomi K, Ogawa J, Ishii Y, Hirabayashi K. Short-term complications and long-term results of expansive open-door laminoplasty for cervical stenotic myelopathy. Spine J 2001 1:26–30.


15. Kawaguchi Y, Matsui H, Ishihara H, Gejo R, Yoshino O. Axial symptoms after en bloc cervical laminoplasty. J Spinal Disord 1999 12:392–5.


16. Yeh KT, Yu TC, Chen IH, et al. Expansive open-door laminoplasty secured with titanium miniplates is a good surgical method for multiple-level cervical stenosis. J Orthop Surg Res 2014 9:49.



17. Highsmith JM, Dhall SS, Haid RW Jr, Rodts GE Jr, Mummaneni PV. Treatment of cervical stenotic myelopathy: a cost and outcome comparison of laminoplasty versus laminectomy and lateral mass fusion. J Neurosurg Spine 2011 14:619–25.


18. Wang HQ. Laminoplasty: a review of its role in compressive cervical myelopathy. Spine J 2009 9:426.


19. Choi BW, Song KJ, Chang H. Ossification of the posterior longitudinal ligament: a review of literature. Asian Spine J 2011 5:267–76.



20. Yang L, Gu Y, Shi J, et al. Modified plate-only opendoor laminoplasty versus laminectomy and fusion for the treatment of cervical stenotic myelopathy. Orthopedics 2013 36:e79–87.


21. Yang SC, Niu CC, Chen WJ, Wu CH, Yu SW. Opendoor laminoplasty for multilevel cervical spondylotic myelopathy: good outcome in 12 patients using suture anchor fixation. Acta Orthop 2008 79:62–6.


22. Hirabayashi K, Satomi K. Operative procedure and results of expansive open-door laminoplasty. Spine (Phila Pa 1976) 1988 13:870–6.


23. Li H, Dai LY. A systematic review of complications in cervical spine surgery for ossification of the posterior longitudinal ligament. Spine J 2011 11:1049–57.


24. Hosono N, Yonenobu K, Ono K. Neck and shoulder pain after laminoplasty: a noticeable complication. Spine (Phila Pa 1976) 1996 21:1969–73.


25. Thakur NA, Heller JG. Cervical laminoplasty: review of complications and strategies to avoid them. Semin Spine Surg 2013 25:209–13.

26. Mesfin A, Park MS, Piyaskulkaew C, et al. Neck pain following laminoplasty. Global Spine J 2015 5:17–22.


27. Lee DG, Lee SH, Park SJ, et al. Comparison of surgical outcomes after cervical laminoplasty: open-door technique versus French-door technique. J Spinal Disord Tech 2013 26:E198–203.


28. Yoshida M, Tamaki T, Kawakami M, et al. Does reconstruction of posterior ligamentous complex with extensor musculature decrease axial symptoms after cervical laminoplasty? Spine (Phila Pa 1976) 2002 27:1414–8.


- TOOLS